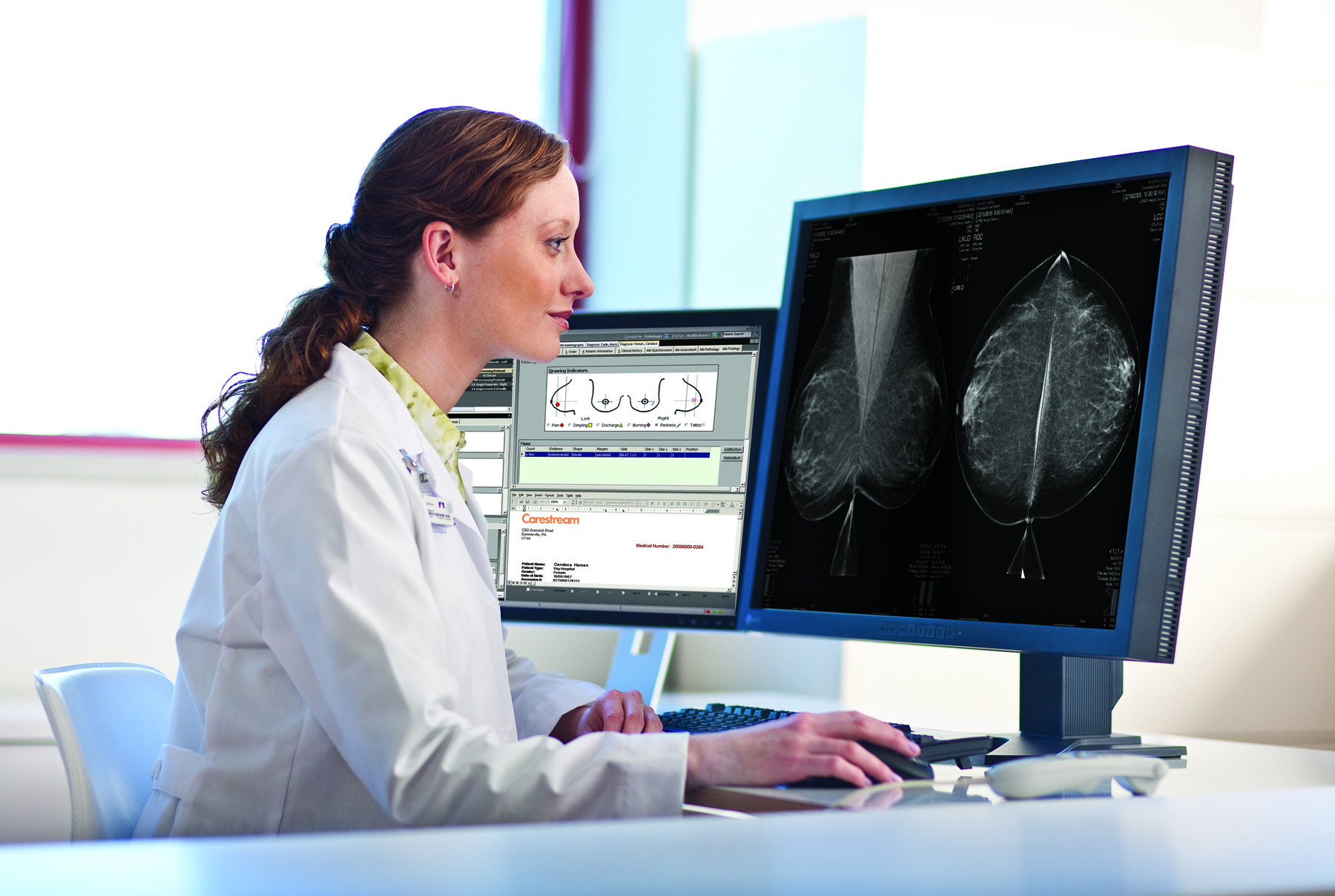
The practice of breast imaging and screening in women at risk for breast cancer is evolving as new imaging modalities are incorporated and researchers continue to study the implications of dense breast tissue in patients. At the 2013 annual meeting of the Radiological Society of North America (RSNA) in Chicago, there were several sessions highlighting trials and studies that brought breast density and cancer detection to the forefront.
Understanding Breast Density
It has been established that dense breast tissue is associated with a higher rate of missed cancers, particularly early-stage cancers, due to the similarities in appearance on mammograms. Women with dense tissue are also said to have an elevated risk of developing cancer in the breast. In a special interest session at RSNA 2013, presenters reported on research that examined breast density and the risks for breast cancer it may pose to patients.1
According to presenter Jennifer A. Harvey, M.D., FACR, professor of radiology at University of Virginia, dense breast tissue can be common among women, but not all occurrences of dense breast tissue link directly to a high risk for cancer. Rather, the elevated risk potentially can vary by age, race, geography and other factors such as eating and smoking habits. With assessment of breast density and the risk for breast cancer becoming an international area for study, it is important for all parties involved to understand the relationship between density and cancer, said Harvey.
In the session, Harvey reported on collaborative research performed throughout the years that continues to dive into the subject of breast density. Mammographic studies, dating from the 1980s and performed around the United States and other countries, were assessed for breast density and cancer incidence. Some of the findings revealed the varied nature of breast density: It is known that breast density declines with age, but the risk for cancer does not necessarily correlate with the decrease and may remain the same throughout a woman’s lifespan. And while dense breast tissue is known to mask cancers on mammograms, breast density did not translate directly to higher risks of cancer for all women. For example, Asian women were found to have denser breasts but reported fewer cancer incidences, said Harvey.
Measuring Breast Density
Part of the mission to understand breast density is the drive to measure and monitor it. Martin Yaffe, Ph.D., professor of medical biophysics at the University of Toronto, spoke on methods of deriving breast density from a variety of imaging modalities, including mammography, digital tomosynthesis and ultrasound. In order to improve screening practices, providers should identify strategies for proper screening of both women with dense breast tissue and women with fatty breast tissue, Yaffe said. Two-dimensional assessment of breast density is more commonly performed with traditional mammography, but 3-D volumetric analysis is believed to offer a more accurate look at density. The focus in the radiology community now, said Yaffe, is to develop a new predictive model of which patients at high risk are more likely to have breast cancer.
Mammography is known to have lower sensitivity for high-risk patients because dense breast tissue can be mistaken for cancers on mammograms. Supplemental imaging is often recommended for those patients in need of further analysis. Identifying cancers at earlier stages improves patient outcomes, but for women with dense breasts, cancers are often not found until later when they are more metastatic.
“No one is talking about replacing mammography at this time,” said Wendie Berg, M.D., Ph.D., FACR, professor of radiology at the University of Pittsburgh. But often the question becomes not whether to perform supplementing imaging, but which imaging modality to pursue for further screening.
In addition to traditional mammography, clinicians have the option of using contrast-enhanced spectral mammography (CESM), ultrasound (such as automated breast ultrasound or ABUS), digital tomosynthesis, molecular breast imaging (MBI), magnetic resonance imaging (MRI) and computed tomography (CT), among others, for imaging the breast. Some offer a more detailed look at irregular-shaped masses in the breast while other modalities provide more ease and comfort for patients. A recent KLAS brief, “3 Things You Need to Know About Breast Imaging,” reported that while mammography remains first in line for breast cancer screening, ultrasound and tomosynthesis are making strides, with 90 percent of providers surveyed indicating that they rely on ultrasound for breast imaging after mammography. The brief also reported that 87 percent of providers stated they had a positive ROI when using tomosynthesis products, even without receiving reimbursements.
One technique offered during RSNA 2013 as a possible option for assessment of density is a noninvasive optical tool developed for breast imaging. “Non-invasive Optical Assessment of Breast Density and Identification of High-risk Subjects,”2 presented by Paola Taroni, Ph.D., professor of physics at Politecnico di Milano in Milan, Italy, revealed that the optical mammography tool can provide functional and structural information on breast tissue through noninvasive means and with no ionizing radiation. Researchers in the Milan study compared women already identified from mammographic studies as BI-RADS categories 1 to 3 and as category 4. The team observed craniocaudal and oblique views of both breasts using multi-wavelength optical mammography, and found that amounts of water and collagen content observed optically increased by BI-RADS category. The observations were consistent with known differences in composition and microscopic structure between dense and fatty tissue, according to Taroni. She concluded that optical estimation of breast density is feasible enough for clinical practice and could provide effective assessment of breast density to complement other imaging modalities in screening practices.
Getting Patients to Understand
Breast density “inform” legislation efforts continues to grow in the United States, with many states working on bills and others already enacting laws to require providers to send breast density notification letters to patients. But sometimes, there is little written about what to do when letters are sent and patients are faced with the information that their dense breasts leave them at higher risk for cancer.
The subject of dense breast patients choosing to pursue supplemental imaging was highlighted at RSNA 2013 during the session “Patient Awareness of Breast Density and Interest in Supplemental Screening Tests for Women With Dense Breasts Among Women at a County Hospital Compared to Women at an Outpatient Radiology Clinic of an Academic Medical Center,”3 where presenters reported on a study that compared women who obtained mammograms in different geographic and hospital settings. In that study, a survey was given to 153 women at a county hospital before their screening appointments, asking whether they were aware of the breast density topic and whether they were interested or willing to pay for additional tests (such as ultrasound or CESM) if they had dense breasts. A similar survey was also conducted at an outpatient radiology clinic at an academic medical center. The study found that women who obtained screening at the county hospital were interested in their breast density, but less willing to incur expenses for additional imaging than women at the outpatient clinic.
“Patient awareness is worse in county hospital settings,” concluded Long Trinh, M.D., currently at Stanford University in Stanford, Calif. “We found that a majority of women were not willing or able to do supplementary imaging.” This is often explained by the fact that women who visit county hospitals for routine mammograms typically do not pursue more care than what is covered under insurance. Women from more rural backgrounds also face longer travel times if they choose to undergo supplemental imaging tests, said Trinh. The disparity shows that if breast density notification and supplemental imaging are to be successful, providers and insurance companies need to ensure that the correct information is communicated and that patients in need of additional screening can afford it.
References
1. Berg W M.D., Ph.D., Harvey J M.D., Yaffe M Ph.D, Smith, R Ph.D,
“Special Interest Session: Breast Density: Risk Assessment,
Communication, and Approaches to Supplemental Imaging,” session presented at RSNA 2013.
2. Taroni, P Ph.D., “Non-invasive Optical Assessment of Breast Density and Identification of High-risk Subjects,” session presented at RSNA 2013.
3. Trinh L M.D. et al, “Patient Awareness of Breast Density and Interest in Supplemental Screening Tests for Women with Dense Breasts among Women at a County Hospital Compared to Women at an Outpatient Radiology Clinic of an Academic Medical Center,” session presented at RSNA 2013.


 May 22, 2026
May 22, 2026