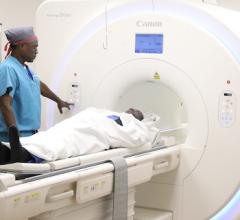
Real-time imaging allows users to acquire a new MR image during surgery after the brain has shifted, providing a more accurate view of the brain.
When a hospital or freestanding outpatient facility purchases a CT or an MR system, it needs an infrastructure that can support it, physicians who understand the new technology and an education and training program to prepare clinical staff – and all of that needs to be integrated within its clinical priorities.
“I shudder to think of a hospital administrator’s dilemma when he looks at how quickly this equipment is going to be evolving over the next few years,” said Amit Sharma, imaging intelligence lead, Sg2, a healthcare research firm.
As medical technology is evolving at light speed, hospital and outpatient administrators need to anticipate how the market is going to develop by looking at clinical advances, market trends and their goals as an entity. These factors lay the foundation for a solid five to 10-year strategic plan and for effectively allocating capital dollars, which for every organization, is often a challenge.
To render a clearer picture of what to expect in imaging modalities and their clinical applications in the next five to 10 years, Imaging Technology News asked Sg2 and clinicians to outline their vision of the future.
1. Coronary CTA and MRA will experience significant growth
Coronary computed tomography angiography (CTA) and magnetic resonance angiography (MRA) are rapidly growing as diagnostic procedures. While standard catheter angiography is still considered the gold standard for diagnosing arterial disease, CTA and MRA are viable alternatives to a catheter angiogram. Both scanners provide detailed images of blood vessels and blood flow without having to insert a catheter directly into an artery, and the procedure and recovery time are also much shorter and less costly.
CTA will see large growth in peripheral and carotid studies, and early detection will lead to increased utilization of interventional procedures.
2. CT will continue growing in a multitude of applications
As volumes shift from X-ray and interventional diagnostic procedures to CT, the modality is slated by Sg2 to grow by 57 percent between 2006-2016, with a population-based growth of 15 percent.
CT will be increasingly used in emergency departments as a rapid diagnostic tool for chest and abdominal pain. 64-slice CT will revolutionize cardiac diagnostic work, decreasing cardiac SPECT over the next two to five years and diagnostic cardiac catheterization over the next four to eight years. As cancer patients live longer, CT will be used for frequent staging and monitoring. Computer-aided detection will make multislice CT use for screening more appealing. The largest volume growth will occur in chest CT, virtual colonoscopy and coronary CTA.
“I think a fundamental change that is happening with the CT is looking at being able to dramatically increase the temporal resolution,” said Chris Farr, vice president of Sg2. “The first commercial attempt would be the Siemens dual-source scanner. I think you are going to see almost a split in the CT market where you will see very high-end general purpose machines that have significant organ coverage in a single rotation, but are really designed for a wide range of applications, and then ultimately I expect you will see machines that are really dedicated to cardiovascular work. Those will be designed with the highest possible temporal resolution so they basically can stop motion as effectively as possible and handle very high heart rates.”
3. MR use will rise 44 percent from 2006-2016
MR imaging will mushroom by 44 percent over the next 10 years, according to Sg2. There will be continued growth in spine and joint studies with the increases in patient activity and obesity, and Baby Boomers’ expectations for activity as they age, will raise demand. Minimally invasive procedures will increase the number of patients opting for surgery, further increasing MR volumes. New MR applications, such as functional and diffusion MR, will be used to stage cancer and stroke patients. Expect also expanded adoption of breast MR.
While a large amount of the growth in MR angiography has already occurred, expect continued national growth in studies on lower extremities. Cardiac MR studies post–congestive heart failure (CHF) and post–acute myocardial infarction will nearly triple.
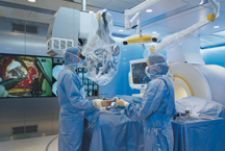
Another emerging role for MR will appear in the OR. Intraoperative MRI has very recently become a reality for neurosurgeons on the medical staff at Presbyterian Hospital of Dallas (PHD) who removed a brain tumor using BrainLAB’s new intraoperative magnetic resonance imaging (iMRI) neurosurgical suite, BrainSuite. Doctors performed the surgery using real-time imaging during brain surgery.
“I would describe real-time imaging for surgery as the wave of the future,” said Neurosurgeon J. Michael Desaloms, M.D. from Presbyterian Hospital, Dallas. “One of the limitations we had before is that we would base our stereotactic navigation based to navigate in the brain on an image done before the surgery. As soon as you open up the skull and start removing brain, there is brain shift. What’s happening is the brain that you are working on is no longer the same on the MR scan that you are using to navigate.
Real-time imaging allows users to acquire a new MR image during surgery after the brain has shifted, providing a more accurate view of the brain. “This helps you know the borders of the tumor more precisely in different areas of the brain. Also, once you finish removing the tumor, you do another real-time scan to see if you have removed the entire tumor. At that point, if you left some of the tumor, you can go back in right then and take out the part that was left over. And that’s what we couldn’t do before,” said Dr. Desaloms.
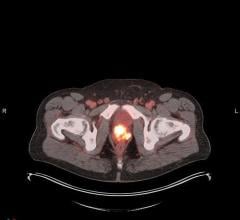
4. PET applications will explode 120 percent in the next 10 years
Positron emission tomography (PET) will grow as PET/CT is further adopted around the nation. PET imaging helps to provide an enhanced understanding of cancer, cardiovascular disease and neurological disorders. As PET is an excellent tool for quantitative diagnosis of disease at the cellular and molecular level, it can positively impact patient management by improving the sensitivity and specificity of anatomical imaging. PET will be increasingly utilized for new indications and applications, particularly in oncology, to closely monitor disease and tailor treatments according to the response of the patient. Cancer patients will be identified earlier in the course of their disease and live longer, causing PET volumes to more than double over the next 10 years. PET also will have an increased role in Parkinson’s disease and Alzheimer’s disease.
“When you look at PET, which is a technology that has been around a very long time, but really only in the last few years has emerged as pretty much the gold standard today for staging a lot of cancers, you can now see this next revolution within the same market, which is the oncology imaging market, but for basically monitoring and personalizing the treatment side of the equation,” said Farr.
The biggest challenge for PET is that it is not used to its full potential because, as Farr sees it, there is a lack of understanding of how the modality actually impacts clinical care. Another barrier is limited reimbursement for PET. Despite these obstacles, Sg2 anticipates “very aggressive growth in this particular modality area over the next 10 years.”
As for PET/CT, Sg2 sources foresee moderate growth, particularly in oncology where the applications include diagnosis and staging of cancer and therapy monitoring of patients on chemotherapy and radiation therapy, where treatment regimes are adjusted according to response very early in the cycle.
“PET/CT for treatment planning is still relatively rare, probably because the resources are only just really moving into the radiation therapy department,” said Sharma. “But I think that is going to be another important application of PET in oncology, and one that — particularly with tumors that are fast growing that are being treated by radiation — will really have an impact. An example would be head or neck tumors, or tumors in the lungs.”
5. Cone-beam CT will transform X-ray into a volumetric modality
There will be a convergence of X-ray and CT with a kind of volumetric imaging. “We have seen cone-beam CT find its way into the fixed interventional stands, but over the long term, it will integrate with almost all of X-ray, mobile C-arms and so forth,” indicated Sharma. “With the angiographic CT capability like DynaCT, you can start imaging a wealth of applications that would now be done in one room as opposed to having to move patients back and forth between a traditional diagnostic CT scanner and an interventional suite.”
Volumetric imaging will work its way down the food chain, says Sharma. “Right now it is really on the very high-end expensive rooms, but I think you are going to see that technology rapidly work its way down so it becomes much more the province of very routine pieces of equipment and sort of where we see it going,” said Sharma. One example of volumetric applications is where cardiologists look at 4-D images to see if a valve is sealing properly. “4-D is basically volumetric changing over time,” noted Sharma, “like the portable C-arm you bring into a surgical suite.”
6. Expect an expansion in applications for SPECT/CT
By 2016, the use of SPECT will drop by 14 percent, as cardiac SPECT studies will lose significant volumes to more advanced diagnostics such as coronary CTA over the next five years. Sg2 indicates that this trend will accelerate throughout the forecast period.
The prospects of SPECT/CT, however, and the introduction of the new SPECT/CT64 hybrid for cardiology, Precedence by Philips, are very exciting. Farr is quick to point out, however, that the SPECT/CT16 version for cancer and infection has yet to reach its full potential.
“Cardiologists are largely evidence driven and it will take some time before Philips can demonstrate how the fused SPECT/CT64 system will impact clinical care,” noted Farr. “Cardiologists who looked at the SNM image of the year – a fusion of SPECT and CT64 done on a workstation with GE equipment – thought it was very pretty, but could not easily understand how it would fit in their practice. It may well be in the ED that this technology takes off. This is also an expensive system, so routine adoption will be slow.”
Farr concluded that he believes that absolute SPECT numbers will drop, while SPECT/CT will become important. “But I think it will mature first in cancer and take much longer in cardiology,” he added.
7. Portable ultrasound systems will match the performance of cart-mounted systems
While the introduction of 4-D ultrasound is an important advancement, the modality’s greatest utility will stem from its miniaturization and portability – the ability to have advanced application on a laptop sized system or a much more handheld portable system.
“The site of care for ultrasound is going to change. Instead of having to go to an outpatient department for an image, that image could come to you,” indicated Farr. “Think about the implications for patients in a nursing home, for example, or even looking at healthcare clinics that are remote. The ability to take high-end imaging conveniently to where that patient is, bedside or in a residential care facility, is significant.”
On the whole, greater awareness of and more screenings for vascular disease will increase ultrasound volumes for abdominal aortic aneurysm, carotid and extremity vascular studies.
8. Oncology applications using CT, MR, PET, SPECT will expand
Advanced imaging applications in CT, MR, PET and SPECT for cancer will broaden. As cancer patients live longer and radiation becomes increasingly accurate and precise, outpatient radiation services will grow by 24 percent. Traditional external beam radiation therapy will grow at the population-based rate of 19 percent, while more precise approaches — including image-guided radiation therapy, intensity-modulated radiation therapy and radiosurgery — will increase rapidly as the number of applications expand. Brachytherapy volumes will rise as cancer is detected earlier and evidence of efficacy increases.
“Imaging for cancer will show robust growth, particularly for the advanced modalities. More imaging will be used in managing a cancer patient than in any other service line — and that trend will continue to grow. If you put in all the CT, all the MR, all the PET work that is going to be done for cancer in the next 10 years,” noted Sharma, “there is going to be a very significant growth rate.”
Farr added that the growth rate is higher than the number of new cancer patients. “What that is saying is that imaging is becoming much more intertwined with the actual management of the cancer patients. There are many more imaging procedures being done during the time of their treatment and treatment monitoring.”
9. Interventional cardiovascular procedures will drop by nine percent
Significant reductions in diagnostic catheterizations from noninvasive imaging will outweigh growth in outpatient interventional volumes. Noninvasive angio procedures such as CTA and MRA will increase. Uterine artery embolization, as well as outpatient carotid stenting, coronary interventions and peripheral interventions, will multiply substantially. Increased vascular screening and survivability of CAD/CHF will lead to a larger peripheral vascular disease patient pool. Increased CAD medical therapy will eliminate the need for interventions in some patients.
10. PET/MR will be available commercially in the next five years
While there is mounting interest in the capabilities and applications for a hybrid PET/MR modality, currently, there are no systems commercially available. PET/MR imaging is fairly limited today and is achieved by manually fusing images on a workstation – a very time intensive process.
While there are manufacturers, namely Siemens, developing PET/MR systems, there are technical challenges involved with merging the two modalities. PET uses photo multiplier tubes to pick up the light that is submitted from the crystal. These multipliers do not work well in high magnetic fields, and require the use of fiber optics and light pipes to separate the photo multipliers from the magnetic field.
“I am sure we will see a PET/MR between now and 10 years out, but I think it is going to be five years plus at least before they are really available commercially,” said Farr.





 April 07, 2026
April 07, 2026