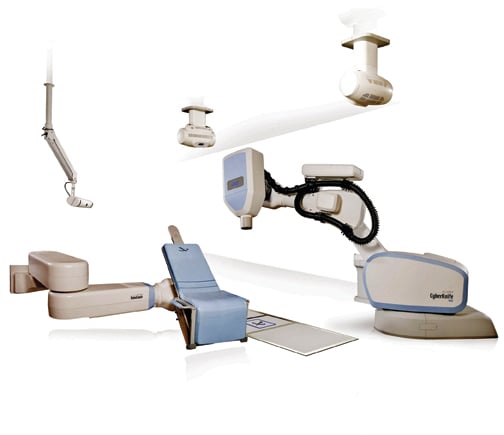
The CyberKnife radiosurgery/SBRT system is a noninvasive alternative to conventional surgery for the treatment of many tumors, including the prostate, lung, brain, spine, liver, pancreas and kidney.
Hypofractionated radiotherapy regimens are emerging as an effective treatment option for many prostate cancer patients. Currently, hypofractionated radiation can be delivered via several methods, including high dose rate (HDR) brachytherapy and noninvasive stereotactic body radiotherapy (SBRT). HDR brachytherapy involves the placement of a radiation source — typically a radioactive isotope — inside or next to the area requiring treatment. High doses of radiation (usually exceeding 12 Gy.hr-1) are delivered directly to the site of the cancer, ensuring that the radiation affects a localized area and minimizing impact to surrounding healthy tissue.
SBRT is similarly capable of delivering a large, but very precise, dose of radiation through the use of arcs or non-coplanar beams intersecting at the tumor. The accuracy allows clinicians to reduce treatment margins and maximally spare critical normal tissue (including rectum, bladder, urethra and penile bulb) from the high-dose treatment field.
Hypofractionation with brachytherapy has demonstrated excellent efficacy and toxicity profiles as both monotherapy and post-external beam radiation therapy (EBRT) boost for localized prostate cancer. In fact, the University of California San Francisco (UCSF) recently reported its HDR brachytherapy boost experience in mostly intermediate- to high-risk disease, achieving five-year biochemical no evidence of disease (bNED) rates of 93 percent with minimal toxicity. [1]
A randomized phase III trial has reported superior bNED rates with HDR brachytherapy boost compared with EBRT alone [2], and a recent systematic review of the world literature has concluded that the combination of EBRT and HDR brachytherapy results in superior bNED and overall survival (OS) compared with EBRT alone or EBRT plus permanent prostate seed implant (PPI) boost. [3]
Nevertheless, despite clinical studies demonstrating excellent results, HDR brachytherapy has been slow to achieve widespread adoption because of its invasive nature, the need for hospitalization and anesthesia, as well as the significant time, resources and technical expertise required for planning and delivery. SBRT, on the other hand, has demonstrated promise in achieving the benefits of hypofractionated radiation therapy, without many of HDR brachytherapy’s disadvantages.
Study Results Show Value of SBRT
A new study from UCSF recently published in the International Journal of Radiation Oncology Biology & Physics demonstrates that standalone treatment with Accuray’s CyberKnife robotic radiosurgery system (an advanced modality for the delivery of SBRT), as well as treatment with the CyberKnife System as a boost following whole pelvis external beam radiation, delivers favorable results (minimal toxicity and excellent prostate-specific antigen [PSA] response) for prostate patients comparable to those achieved with more invasive HDR brachytherapy.
The CyberKnife radiosurgery/SBRT system is a noninvasive alternative to conventional surgery for the treatment of many tumors anywhere in the body. This robotic system delivers beams of high-dose radiation to tumors with extreme accuracy, providing a pain-free, nonsurgical option for patients who have inoperable or surgically complex tumors, or who may prefer an alternative to surgery.
The UCSF study reported on 38 patients ranging in age from 54 to 82.4 years with a minimum followup of 12 months. Twenty of 38 patients were treated with SBRT monotherapy (9.5 Gy × 4 fractions) and 18 were treated with SBRT boost (9.5 Gy × 2 fractions) post-EBRT and androgen deprivation therapy. As a descriptive comparison, PSA nadir to date for 44 HDR brachytherapy boost patients with disease characteristics similar to the SBRT boost cohort were also analyzed.
The treatment protocol included placing three prostate fiducial markers into the prostate gland a minimum of one week before simulation for SBRT and/or EBRT and use of both computed tomography (CT) and magnetic resonance imaging (MRI) for treatment planning and optimal target and organ at risk (OAR) delineation. Treatment planning was carried out with dosimetric constraints comparable to UCSF’s inverse-planned HDR brachytherapy technique, achieving similarly strict target-volume coverage, dose heterogeneity and normal tissue sparing parameters. The majority of patients were treated on consecutive working days.
Post-treatment, patients were followed every three to four months for PSA response, testosterone levels and physician-assessed and patient-reported acute and late toxicity.
Highlights of the results include:
• SBRT was well tolerated in all patients.
• All patients are without evidence of biochemical or clinical progression to date.
• PSA response as defined by PSA nadir to date has been excellent. With a median followup of 18.3 months and a median of five post-treatment PSA measurements, the entire cohort has achieved a median PSA nadir of 0.35 ng/mL (the monotherapy cohort has achieved a current median PSA nadir of 0.47 ng/mL and the SBRT boost patients achieved a current median PSA nadir of 0.10 ng/mL). With a median followup of 48.6 months, the comparable HDR brachytherapy boost cohort has achieved a median PSA nadir of 0.09 ng/mL.
Organ motion management is a key consideration for prostate cancer SBRT. As a result of gas or fluid in the bowels, the prostate is subject to random and significant target motion that can make accurate treatment delivery difficult to achieve. To account for prostate movement, the CyberKnife system utilizes online imaging during radiation beam delivery designed to track, in real time, implanted fiducials in the prostate gland, and it automatically adjusts the robotic beam delivery in response to interfraction and intrafraction prostate motion. This technology was employed for patients treated as part of this study, allowing researchers to maximize normal tissue sparing with minimal planning treatment volume (PTV) expansion, while minimizing the risk of a geographic miss due to prostate motion. This technology, as well as additional capabilities, are now part of the CyberKnife system’s InTempo adaptive imaging system, an intelligent and adaptive technology designed from the ground up to track and correct for prostate movement.
To note, although promising results also have been published with conventional linear accelerator-based SBRT platforms for non-prostate sites (including lung, liver and spine), the prostate gland’s unpredictable intrafractional motion and the minimal PTV expansions required for safe HDR brachytherapy–like dosimetry may preclude the use of conventional systems for prostate SBRT without real-time target tracking and beam-correction to account for intrafraction motion.
This study demonstrates the feasibility, promising PSA nadir and low acute toxicity of definitive SBRT as a standalone therapy or as a boost following whole pelvis EBRT for patients with localized prostate cancer. The CyberKnife system is unique in its ability to deliver SBRT in a manner that effectively reproduces the dose distribution of HDR brachytherapy with real-time tracking and beam adjustment for organ motion. Because the system is able to deliver precise dose sculpting of a moving target in which highly targeted beams of radiation “paint” only the tumor while tracking tumor motion and avoiding surrounding healthy tissue, patients benefit from the accuracy of HDR brachytherapy while eliminating the invasive aspects of catheter placement under transrectal ultrasound guidance.
In conclusion, a significant — and for some, controversial — paradigm shift may be under way in the radiotherapeutic management of localized prostate cancer. Emerging evidence suggests hypofractionated SBRT and HDR brachytherapy may yield outcomes comparable to conventional EBRT, including intensity-modulated radiotherapy (IMRT), but in far fewer treatment sessions completed in much less time. With the proof of principle that SBRT can recreate HDR brachytherapy dosimetry4, early results suggest excellent clinical outcomes with SBRT despite decreased invasiveness, incurring less risk of bleeding and infection, and requiring less pain medication, no anesthesia and no overnight hospital stay. Pending long-term clinical data, SBRT may represent a radical change in the treatment of localized prostate cancer.
Siavash Jabbari, M.D., practices at Advocate Lutheran General Hospital in Park Ridge, Ill. Jabbari is a productive researcher in the fields of prostate, head and neck, and children’s cancer. He has been a devoted advocate for cancer patients and the field of radiation oncology. He has authored numerous book chapters, publications and invited presentations, co-moderated the Presidential Symposium of the annual meeting of the American Society of Radiation Oncology (ASTRO) and served on the Executive Board of the Association of Residents in Radiation Oncology (ARRO).
References:
1 Kaprealian T, Weinberg V, Speight J, et al. “High dose rate brachytherapy boost for prostate cancer: Comparison of two different fractionation schemes.” Paper presented at the 2008 Annual Meeting of the American Society of Radiation Oncology (ASTRO); November 2008, Boston, Mass.
2 Hoskin PJ, Motohashi K, Bownes P, et al. “High dose rate brachytherapy in combination with external beam radiotherapy in the radical treatment of prostate cancer: Initial results of a randomized phase three trial.” Radiother Oncol, 2007; 84:114–120.
3 Pieters BR, de Back DZ, Koning CC, Zwinderman AH. “Comparison of three radiotherapy modalities on biochemical control and overall survival for the treatment of prostate cancer: A systematic review.” Radiother Oncol, 2009; 93:168–173.
4 Fuller DB, Naitoh J, Lee C, et al. “Virtual HDR CyberKnife treatment for localized prostatic carcinoma : Dosimetry comparison with HDR brachytherapy and preliminary clinical observations.” Int J Radiat Oncol Biol Phys, 2008; 70:1588–1597.
SIDEBAR:
More Studies on SBRT for Prostate Cancer
Results of two clinical studies demonstrate that real-time tumor tracking with the Calypso system during five-day stereotactic body radiotherapy (SBRT) for prostate cancer enabled clinicians to reduce treatment margins and minimize dosimetric impact of prostate motion. Data from one of the studies was presented at the recent congress of the European Society for Therapeutic Radiology and Oncology in London.
“Stereotactic body radiation therapy requires significantly fewer treatment sessions compared to conventional radiation therapy, making it an increasingly appealing option for a number of cancers, including prostate,” said Kenneth Russell, M.D., chief medical officer of Calypso Medical. “Results from these studies and others suggest that continuous tracking of the target during radiation delivery with Calypso’s real-time tracking technology can safeguard radiation delivery and spare surrounding healthy tissue.”
Researchers in the study highlighted at ESTRO treated eight patients and used the Calypso system to track and manage motion of the prostate during radiation therapy. Patients received a dose of 10 Gy per treatment (a.k.a. fraction) for a total of 50 Gy. Study authors retrospectively analyzed the intrafraction prostate motion recorded by the Calypso system during treatment and demonstrated that it is feasible to decrease the margin (extra space added around the planned target volume) because they could adequately manage the intrafraction prostate motion with Calypso’s continuous targeting. The effect was sparing more of the anterior rectum’s exposure to radiation. Reducing the dose to the rectum may decrease toxicity or allow higher doses to be used to better fight the cancer.
“As stereotactic body radiotherapy involves higher radiation doses than conventional intensity-modulated radiation therapy, reducing treatment margins is an important step in limiting side effects,” said Ryan Foster, Ph.D., an investigator in the study and assistant professor of radiation oncology at the University of Texas Southwestern Medical Center in Dallas. “This study demonstrates that the dosimetric impact of intrafraction motion during prostate SBRT delivery is not clinically significant when a rectal balloon is combined with Calypso for assessment and monitoring of intrafraction motion. Real-time tumor tracking may be an important tool in reducing treatment margins during SBRT for prostate cancer.”
In another five-day prostate SBRT study using Calypso real-time tracking to guide radiation therapy, authors reported favorable quality-of-life and toxicity outcomes. The study results of this fifty-four patient Phase II trial were presented at the annual meeting of the American Society for Radiation Oncology (ASTRO) last fall and published in the November 2010 edition of the International Journal of Radiation Oncology Biology & Physics.
The Calypso system uses GPS for the Body technology to safely guide radiation delivery during prostate cancer treatment. Beacon electromagnetic transponders, smaller than a grain of rice, are permanently placed in a patient’s prostate or prostatic bed. Each transponder emits a unique radio frequency signal to the system, which then determines the exact location and motion information about the tumor target. Because the tumor can be accurately tracked and monitored, precise targeted radiation can be delivered to the tumor while sparing surrounding healthy tissue and organs.


 May 06, 2026
May 06, 2026 









