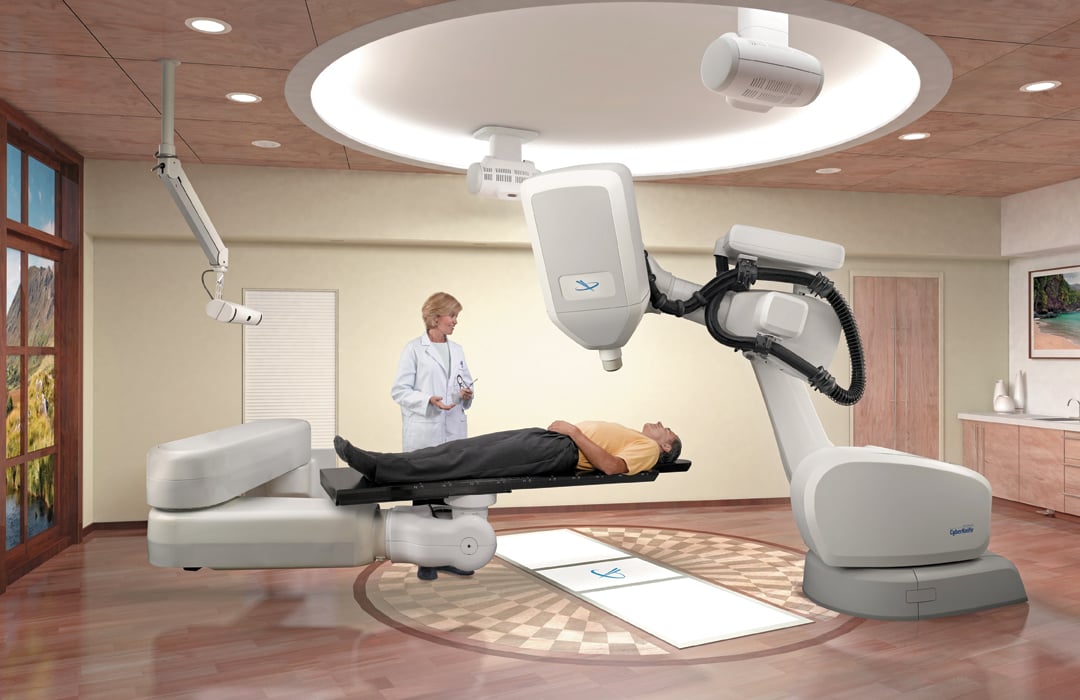
A CyberKnife treatment plan for lung cancer.
The preferred treatment for patients with operable lung cancer is surgical resection. However, many lung cancer patients whose tumors are technically resectable have other medical problems, such as chronic obstructive pulmonary disease, which make it difficult to endure lung cancer surgery. Until the last decade these patients were treated with conventional radiotherapy, but more recently stereotactic body radiotherapy (SBRT), or the accurate delivery of high doses of radiation over a short period of time, has emerged as an alternative treatment.
SBRT has been shown to be effective in the treatment of lesions in the peripheral region of the lungs.[1] Extending SBRT to the central lung is much more complicated. SBRT delivered to lesions located within 2 cm of the primary central airways of the lung can result in pneumonia, pericardial effusion, hemoptysis or even death.[2] Given these risks, it would be understandable if centers shied away from treating patients with central lesions with SBRT.
Observing this trend, and in light of features available with the CyberKnife SBRT system, the Erasmus MC – Daniel den Hoed Cancer Center in Rotterdam launched a study in July 2006 focused specifically on the use of SBRT to treat central lung tumors. The study, "Outcome of Four-Dimensional Stereotactic Radiotherapy for Centrally Located Lung Tumors," reported on 56 patients (39 with primary lung cancer and 17 with metastatic tumors) treated with the CyberKnife system.[3] All of these patients were ineligible for surgery or chemotherapy, refused surgery or chemotherapy, or had an inoperable tumor.
Unlike other SBRT treatment methods, the CyberKnife system is equipped with a technology called the Synchrony respiratory tracking system, making it uniquely suited to treating central lung tumors. The Synchrony system correlates the position of the chest as it rises and falls during breathing with the position of the tumor as revealed with the CyberKnife's image-guidance system. This allows Synchrony to guide the radiation beam so that it remains locked onto the moving tumor, thus allowing clinicians to significantly reduce treatment volumes and spare healthy tissue without the need for gating, breath holding, body frames or abdominal compression.
The treatment accuracy of the Synchrony system allows the margins necessary to account for uncertainty in target position to be narrow (at Erasmus MC, the total clinical error is routinely less than 1.5 mm), so that high SBRT doses can be delivered with relatively low toxicity to the central chest region. Keeping toxicity low is especially important for these patients, many of whom are treated with SBRT precisely because they are unable to withstand the rigors of surgery.
Study Details
The study found that tracking and correcting for respiratory motion with CyberKnife SBRT allowed clinicians to deliver treatment to the central lung with minimal toxicity, sparing surrounding healthy tissue, while also providing high levels of tumor control. In fact, the toxicity was among the lowest reported to date for central lung lesions.
Local tumor control was 91 percent for the entire group at one year and 76 percent for the entire group at two years. For the patients treated with at least 50 Gy, two-year local control was 85 percent. The overall two-year survival rate was 60 percent. The analysis of toxicity rates demonstrated that there were no serious complications (especially no life-threatening/disabling or fatal toxicities).
Conclusions
Historically, research has shown that even SBRT doses as low as 40 Gy can cause significant complications when treating lesions in the central chest. These findings point to the critical importance of careful treatment planning, accurate patient setup and precise radiation delivery.
For this study, the patients benefited from the team’s ability to use small error margins around the clinical target volume, with the CyberKnife system. The small margins could only be achieved with the Synchrony system.


 May 19, 2026
May 19, 2026 









