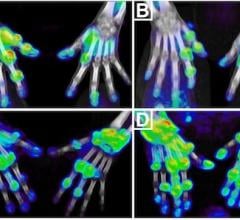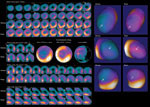
A novel imaging agent for PET, BMS747158 detects more ischemia than technetium SPECT/CT imaging.
When digital electronic devices are first released on the market, they are sold at a premium. Gradually, as their capabilities improve, they become less expensive and more accessible to the masses. Such is the case in molecular imaging with positron emission tomography/computed tomography (PET/CT) and single photon emission computed tomography/computed tomography (SPECT/CT).
Both systems capture the heart’s functional data, including the rate of blood flow and the metabolism of the heart. This data helps with the diagnosis of coronary artery disease (CAD).
Yet, while PET/CT generates significantly higher quality images than SPECT/CT, of the two, SPECT/CT is much more widely used for cardiac imaging. This is due to the higher cost of the PET/CT modality and its imaging agents. However, new research and novel imaging agents are paving the way for PET/CT to eventually replace SPECT/CT as the test of choice for cardiac imaging.
Game Changer
A major game changer in the practice of medicine in the United States is comparative effectiveness research (CER). The Institute of Medicine (IOM) defines CER as “evidence that compares the benefits and harms of alternative methods to prevent, diagnose, treat, and monitor a clinical condition or improve the delivery of care.” As the U.S. government strives to balance health care costs and effectiveness, it will use CER to determine reimbursement for diagnostic imaging and treatments.
One of the CER research priorities is cardiovascular and peripheral vascular disease as they relate to ischemia, heart failure and arrhythmias.
In support of this initiative, the Society of Nuclear Medicine (SNM) has established a task force to develop high quality, comparative effectiveness PET/CT imaging studies. This July, SNM will discuss cost and comparative effectiveness studies in cardiology, neurology and oncology at the Agency for Healthcare Research and Quality (AHRQ) sponsored meeting.
“The biggest challenge [in CER] is relating the imaging study to the patient outcome,” explained Michael M. Graham, Ph.D., M.D., president, SNM, professor of radiology, director of nuclear medicine and the department of radiology.
This new research will demonstrate the importance of PET/CT in guiding the management of CAD.
PET/CT Outperforms SPECT/CT
There is an overall trend toward better patient outcomes when using molecular imaging in diagnostic work up.
Currently, SPECT/CT is the most commonly used molecular imaging test for CAD. However, in head-to-head studies between the modalities, researchers are discovering the advantages of PET/CT over SPECT/CT for acquiring cardiac images.
One of the key differences between the modalities is time, according to Jamshid Maddahi, M.D., FACC, professor of molecular and medical pharmacology, professor of medicine at UCLA’s David Geffen School of Medicine.
“PET/CT protocols for imaging are faster,” Dr. Maddahi told Imaging Technology News in an exclusive interview.
“SPECT/CT imaging takes between two to two-and-a-half hours to complete a rest–stress study. There are two reasons for this. One is that we need to wait about 30 to 45 minutes between injection and imaging to allow clearance of technetium-99 (Tc-99m) labeled SPECT/CT agents from the liver,” he said. “Second, we need to wait 30 to 60 minutes between the rest and stress imaging. This allows enough decrease in counts on the resting image so that it does not interfere with the counts on the stress image.”
He added, “In contrast, PET/CT imaging is done a few minutes after injection, and the waiting period between the rest and stress studies is shorter due to shorter half-life of the fluorine-18 (F-18) label. It takes 110 minutes, as compared to Tc-99m, which takes six hours.”
Specificity is another point of differentiation. Dr. Maddahi said studies on PET/CT have shown it has less false positives than SPECT/CT, resulting in higher specificity.
“Tissues surrounding the heart, such as the diaphragm, breasts and subcutaneous fat, cause attenuation, which may appear as reduced perfusion. With PET/CT, attenuation correction is routinely done, which removes these artifacts. Overall, the specificity of PET/CT for detecting coronary artery disease has been shown to be higher than SPECT/CT,” he concluded.
According to Dr. Maddahi, PET/CT is superior in detecting mild coronary disease as well as the extent of the ischemia by revealing the number of diseased coronary arteries.
“It’s important to know if an individual has one, two or three vessels with the disease. With SPECT/CT we often underestimate how many vessels or coronary arteries are involved. The extent of the disease can be better assessed with PET/CT,” he said.
New Agent Gives PET/CT a Boost
Despite the superior quality of PET/CT imaging, adoption of the technology for cardiac imaging has been slowed by the cost and the logistics of producing the agents.
The Centers for Medicaid and Medicare Services currently reimburses existing agents for myocardial PET/CT imaging. This includes rubidium-82 (82Rb), fluorodeoxyglucose (FDG), and [13N]Ammonia. However, each agent has it’s challenges.
With ammonia, the half-life is just 10 minutes, requiring an onsite cyclotron, which is expensive. Similarly, the rubidium tracer requires a generator, which carries with it a fixed overhead cost of $35,000 to $40,000 per month. To cover this cost, a center must perform between seven and eight exams a day consistently.
In an effort to produce an affordable and accessible imaging agent for PET/CT, Lantheus Imaging is developing a fluorine 18-labeled (F-18) agent with a two hour half-life. The novel F-18 PET/CT tracer is designed for myocardial perfusion imaging (MPI). Like FDG, the new agent, called BMS747158, can be manufactured by a regional cyclotron and then shipped to several PET/CT imaging centers. According to Dr. Maddahi, this eliminates the need for an onsite cyclotron or generator.
The data from a Phase I study showed high myocardial uptake at rest that significantly increases with pharmacologically induced stress and a ratio of myocardial to background radioactivity that is favorable and improved over time. These findings suggest that BMS747158 has potential to be used as a myocardial perfusion PET/CT agent for patients both at rest and under stress.
“More that 80 percent of the U.S. population is within the range of a regional cyclotron,” he added. “Like technetium, BMS747158 can be shipped to imaging centers as a unit dose. Therefore, you do not need a minimum number of patient studies per day to make the cost of the tracer economical.”
In preliminary Phase 2 studies, Dr. Maddahi and his team have found BMS747158 detects more ischemia than Technetium SPECT/CT imaging.
Feasibility of Cardiac PET
Even if the cost of the tracer drops, the price of a new PET/CT system ranges in the millions, which is cost-prohibitive for many centers. However, the one bright spot is the widespread adoption of PET/CT for oncology.
“There are many nuclear medicine centers that already have PET/CT devices due to increasing use of PET/CT in oncology,” noted Dr. Maddahi. “FDG is an F-18 labeled tracer that is available through regional cyclotrons and is already approved for assessment of myocardial viability. FDG PET is considered the gold standard for assessing myocardial hibernation and viability, which has been shown to be an important evaluation in patients with heart failure.”
The increased use of PET/CT for oncology amongst nuclear medicine physicians will facilitate the transition to F-18 PET/CT imaging in the future, according to Dr. Maddahi. He also anticipates many imaging centers that have consistent volumes of seven to eight patients a day will start by using rubidium PET/CT for MPI, and then transition to BMS747158.
“Their familiarity with rubidium PET will make it easier to adopt BMS747158 in the future,” he added.
Transition to PET/CT
The transition from SPECT/CT to PET/CT for cardiovascular imaging may come gradually, but for Dr. Maddahi, it is inevitable.
“I believe because of the superiority of PET/CT, it will ultimately dominate SPECT/CT for cardiac imaging,” he said.
“We witnessed a similar phenomenon when SPECT became available as an alternative to planar imaging. The field went through many scientific comparisons of the two modalities until SPECT became the primary imaging modality in nuclear medicine,” said Dr. Maddahi.
“When both SPECT/CT and PET/CT devices are available in nuclear medicine centers, PET/CT will gradually expand to more and more patient subgroups as an alternative to SPECT/CT,” said Dr. Maddahi
He added, “Obviously, the underlying motivation is to use a superior technology to provide superior patient care.”


 May 18, 2026
May 18, 2026