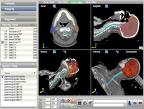
OncoView is an oncology-specific image management and storage solution that integrates images from diagnosis to radiation therapy, and in the same view provides data on the location where dose was delivered in a follow-up exam.
In a short time, the field of radiation oncology has experienced an explosion in imaging data. With large volumes of images generated across the course of treatment — from diagnosis to treatment planning, real-time treatment and follow-up — clinicians are grappling with what many refer to as a data tsunami.
While providing greater and more comprehensive information to help clinicians make decisions and monitor progress, managing and storing all the data poses a formidable challenge. The latest upgrades to oncology information management systems seek to streamline the flood of scans, from CT and MR to PET and all points in between, through better integration of multiple imaging modalities and more sophisticated storage solutions.
In the old “record and verify” days, images were usually acquired during diagnosis and treatment planning stages. Since image-guided radiation therapy has become an established treatment, large volumes of image data are generated at each stage of the process, from patient positioning and treatment planning to tumor tracking through post-therapy monitoring.
“The fundamental question is how are we going to handle all these images?” noted Tim Fox, Ph.D., director of medical physics and associate professor of radiology oncology at Emory University School of Medicine. “[All these images] are a blessing and a curse. I think we’re at the stage now where we want to integrate all this information together. This has always been the ultimate goal.”
A new product Varian Medical Systems launched at the Radiological Society of North America (RSNA) 2008 is designed specifically to archive information covering the entire treatment process.
OncoView is an oncology-specific image management and storage solution, for which Fox helped develop some of the technology. It supports the archiving of the most commonly used images in oncology care, including CT, MR, PET and X-ray. It also stores other important data, such as radiotherapy treatment plans and dose levels. OncoView is designed to supplement a hospital’s existing PACS or can be used as a stand-alone solution for centers that don’t have a PACS.
The system aims to address the limitations of traditional PACS by presenting a bigger picture. “With OncoView, you can now not only store the images but integrate them from diagnosis to radiation therapy to looking at where dose was delivered in the follow-up exam,” Fox said. “Without that information integrated into one view, you’re sort of guessing. What we’ve done is take a treatment planning system and a typical PACS viewer and bring that all together into one view — and also provide storage.”
A key benefit of the system is its ability to offer higher quality without sacrificing efficiency, he added. “We can do things we couldn’t do before, [like] integrate radiation dose distribution with PET or CT scans, but don’t have to hire another position or change department workflow.”
Gordon Ray, M.D., a radiation oncologist at Palo Alto Medical Foundation in Palo, Alto, Calif., says OncoView is the only product he knows of that addresses the “explosion of imaging” facing the rapidly changing field today. “To [provide] sophisticated multimodality care, you have to use multiple sources: MRI, CT, PET/CT,” Dr. Ray said. “We have seen an explosion of digital imaging in the diagnostic stage, pretreatment evaluation, and during onboard imaging, while the patient is undergoing treatment. It allows you to be precise and verify what you are treating. And after treatment, it generates another explosion.”
The ability to generate images on the spot helps clinicians make the best decisions regarding treatment in less time than before.
“The ability to manage and access this data is such that it increases efficiencies dramatically. We have a way to access information that is time oriented. We can get the digital images in a stored fashion that is also scalable,” he said.
Images Integrate Into RT
Since going completely electronic in 2006, a cancer center in Baton Rouge, La., estimates the amount of imaging it has generated would occupy an office 10 feet high, 14 feet long and 12 feet wide from floor to ceiling.
When Baton Rouge General Medical Center’s Pennington Cancer Center decided to open a second facility seven miles away, its board decided to make both facilities completely paperless. The oncologist workstation, provided by Siemens Healthcare, basically mini-physicians workstations that allow physicians to review images wherever they are at whatever stage, proved instrumental in this quest.
“We leverage our electronic medical records, in this case it is an OIMS, to provide the information we need to care for any of our patients regardless of which campus or physician. We can do our treatment planning, our simulation, all our work and build [the] charts. And we can do all this wherever we are,” said Zachary D. Smith, RT, MBA, director of radiation oncology and respiratory care. “Things have gotten so fast, the image has gotten so good, tools have gotten so much better. Now we’re finally able to catch up to making the information electronic, accessible, fast.”
It’s a completely different world than in the eighties when Smith began his radiation therapy practice. “We’re imaging patients so much more than we were. [Back then] you made a lot of assumptions based on external landmarks to treat internal targets,” Smith said.
A series of innovations introduced in the last three to five years have enabled the integration of all diagnostic imaging with planning information and radiation therapy imaging. “We’re now able to take not only what was imaged with diagnostic but marry that with treatment, with almost near live imaging of the patient in the treatment position,” he added.
And with treatment regimes lasting an average of six weeks, it can make a critical difference. “Imagine trying to lay on your bed every day for six weeks [in the exact same position] within a millimeter,” Smith described. “Every time you didn’t do that right, a percentage point of ability to be cured goes down. That’s the level of accuracy we need.”
The FDA-approval pending ImageGrid PACS-RT system from Candelis — distributed through Siemens Healthcare — brings all the pieces together.
The appliance provides radiation therapy and oncology centers an effective DICOM-RT image management and archiving solution. A fully integrated 2D/3D RT viewer enables oncologists to review, approve and sign-off on treatment plans from any workstation.
“Integration is the wave of the future,” Smith said. “We have finally evolved past the record and verify system. We’re picky people; this is high radiation we use, and we have to make sure it’s right. Now it has all the pathology, all the documentation, dictation, treatment planning information, billing and scheduling.”
ImageGrid meets all the center’s clinical needs for flexibility and concurrent use, he says.
Going Green
The need to quickly and easily track down patient records prompted the transition to a paperless environment at the Hux Cancer Center, Terra Haute, Ind. To facilitate the transition and achieve the IT infrastructure to streamline its complex workflow, the center implemented Elekta’s MOSAIQ 2.0. This latest version of MOSAIC includes electronic recording of the mandatory time-out, more easily available patient setup information and batch processing of documentation.
“The features of 2.0 will eliminate the need for never-ending searches [for files],” said Michelle Verst, medical physicist. “In a non-paperless environment, there is always a search for the chart or some document that should have been filed.
With the batch processing, this data is much more quickly available, and multiple users can access the data simultaneously. We will be able to make informed clinical decisions without the wasted time of trying to find the data.”
All of these features provide avenues for quickly processing the data and making it available immediately to the appropriate staff, she adds.
The center has a central repository for all imaging needs within the department called the MOSAIQ Oncology PACS. In addition, it is moving toward a central repository for all clinical data, such as dictation, lab results and nursing assessments, and more, using MOSAIQ 2.0.
“As we compile an ever-increasing amount of information, a central location is vital to maintain the integrity of the patient data,” she said. “Accessibility, timeliness and usability are paramount to provide quality, informed patient care. If the information is not centrally located, we risk loss of data and less than optimal patient care.”
Some challenges that Elekta faces include enhancing support for brachytherapy and HDR treatments, improving “the management of complex treatments such as IMRT and VMAT, and evolving the MOSAIQ Oncology PACS into a fully robust and essential product. “As we push forward to become fully electronic, tools to audit and evaluate the integrity of the data will become vital,” Verst said. “We must have a process that does not rely so heavily on an individual’s review of the data.”
In concert with MOSAIQ 2.0’s debut at the 51st Annual Meeting of the American Society for Radiation Oncology ASTRO in Chicago, Elekta unveiled additional tools for improved clinical precision, workflow efficiency and patient comfort. These include Intuity and Symmetry advanced image-guidance solutions.
Intuity, Elekta’s new IGRT software release, will allow clinicians to understand continuous changes in the positional relationships of both tumor and healthy tissues at the time of treatment. This is designed to enable accurate patient repositioning to ensure target coverage without inadvertently damaging organs.
Symmetry is an image guidance solutions for motion management. This technology lets clinicians quantify the set-up changes required to accommodate ‘baseline shifts’ (tumor path changes between treatments). It uses anatomically correlated guidance as an alternative to gating and offers shorter treatment times due to an easier set-up.
A sixth-generation digital treatment control system, Integrity, takes advantage of a complete re-engineering into the LynX OS platform by adding MLC interdigitation, continuously variable dose rate for VMAT and enhanced virus protection. All three tools are currently 510(k) pending and not yet available in the United States.
Technological advances in oncology information systems are offering increasingly effective and integrated solutions for clinicians to make sense of the deluge of imaging data they sort through each day.
“As the field of imaging continuously evolves, so must the OIMS evolve to support it,” said Verst.


 May 19, 2026
May 19, 2026