Henry Wagner, M.D., Johns Hopkins University in Baltimore
One of the most prominent figures in nuclear medicine in the last half-century is Dr. Henry Wagner of Johns Hopkins University in Baltimore, MD. Dr. Wagner has conducted pioneering research in imaging the perfusion and ventilation of the lungs, kidney and spleen scanning, myocardial perfusion scanning with potassium-43, gated blood pool imaging and imaging brain receptors with PET. His new autobiography, A Personal History of Nuclear Medicine (Springer, New York City, 2006), tracks his many accomplishments and provides his perspectives on the challenges facing the academic and medical establishments.
The story of the birth and growth of nuclear medicine is one of the most fascinating in medicine, an example of the observation that things don’t happen; people make things happen. Nuclear medicine evolved using the tools of physics and chemistry to solve patient problems. But first, political, as well as scientific and technological, challenges had to be faced and solved.
‘Tracing’ the Evolution of Nuclear Medicine
The most fundamental principle of nuclear medicine, the “tracer” principle, was invented in 1913 by a Hungarian chemist, Georg von Hevesy. He discovered that it was possible to “track” molecules as they participate in chemical processes within the living body.
Our team at Johns Hopkins proposed projects [that] were directed toward in vivo imaging of neuroreceptors, starting with C-11 spiroperidol and C-11 diprenorphine. We would concentrate on Parkinson’s disease, Huntington’s disease, tardive dyskinesia, schizophrenia and chronic pain.
Despite skepticism expressed by our superiors, on May 25, 1983, we succeeded in carrying out the first successful imaging of a neuroreceptor in the living human brain. Using the radioactive tracer carbon-11 N-methyl spiperone (C-11 NMSP) and PET, we were able to image the accumulation of a radioactive tracer by dopamine receptors in the basal ganglia of my brain. The chemical synthesis of the tracer and the PET imaging were carried out in the Nuclear Medicine Division at Johns Hopkins Hospital.
Human Guinea Pig
Carfentanil is the most potent of all opioid drugs and is potentially toxic or even lethal to human beings. It is recommended that any game animal which has been given the drug for immobilization should not be consumed for at least 45 days. Some state that it is probably not wise under any circumstances to consume animals that have been immobilized with carfentanil, and there have been reports of humans developing symptoms of drug toxicity from consuming animals given immobilizing drugs. As little as 20 ug (micrograms, an almost invisible drop) of carfentanil is lethal to human beings.
We knew carfentanil was an extremely potent opiate, because of the experience of its use to immobilize wild animals. It had never been given to a human being. We thought (correctly, it turned out) that it would be avidly bound by the subject's opiate receptors.
We had carried out the first imaging of a neuroreceptor (the dopamine receptor) in a human being (I was the subject then, too) in 1983. The carfentanil imaging study of my brain was performed in May 1984. It was the first imaging of an opiate receptor in a human being. The dose of carfentanil that I was to be given would be exceedingly small, but we thought it wise to have an anesthesia machine present in case there was an effect on my breathing.
As I lay with my head held in position in the NeuroEcat PET scanner, I was injected with 25
millicuries of C-11 carfentanil, containing 80 nanograms/kg of the drug. In the room were Jim Frost, Sol Snyder, Jon Links, our chief nuclear medicine technologist, Jim Langan (who had been in nuclear medicine at Hopkins since its inception in 1958) and two other technologists, Jay Rhine and Martin Stumpf.
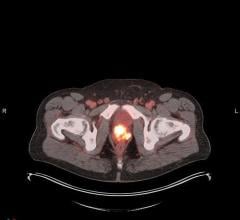
Three imaging planes were viewed, with the cephalic plane passing through the cerebral cortex above the corpus callosum; the central plane passed through the caudate nucleus, putamen, thalamus, and cerebral cortex; the lower plane passed through the cerebellum. Images were obtained for an hour after injection of the tracer.
After 30 minutes, the greatest accumulation of radioactivity was in the medial thalamus, with less in the lateral thalamus. The frontal and temporoparietal cerebral cortex had somewhat less activity, but substantially more than the occipital cortex. In the caudate slice, there was activity in the pituitary and temporal lobes of the cerebral cortex.
Three hours later, naloxone was injected at a dose of 1 mg/kg, followed by a second dose of 25 millicuries of C-11 carfentanil. The radioactivity accumulation was markedly decreased compared to that in the earlier study before naloxone. This provided strong evidence that the carfentanil was binding to my opiate receptors.
A Healthy Skepticism
Under the peer-review system, individual faculty members can bypass the power structures of medical schools, and there has been a steady, annual increase in the NIH budget, which led to a great increase in the size of medical school faculties and increasing numbers of research projects. The steady increase in the number of creative basic and clinical scientists throughout the U.S. resulted in the country achieving the major role in biomedical research.
Individual creativity was the hallmark of biomedical research. Essential to the success of the peer-review system is the expertise and honesty of the reviewers, the objectivity and confidentiality of the proposals and the objective opinions of the peers. Their reviews were returned to the investigators, and resubmissions were commonplace if the initial application failed to be funded. Scientists worked not to gain the favor of their academic or political leaders, but to gain the respect and approval of their peers from throughout the country.
Fortunately, I had seen at an early age the excitement and pleasure of research. I had the good fortune to work in the laboratory of the famous psychobiologist Curt Richter as a student, and then join the stimulating surroundings of the NIH from 1955-1957. My being a medical student and then a “house officer” in internal medicine at Hopkins also encouraged a love and respect for research, which Johns Hopkins has always valued as a principal function of the university and its medical school.
One of my first lessons at the NIH was that the opposite of “to love” is not “to hate,” but “to ignore.” When we presented our work to our peers and leaders, their critical comments were an indication that they took the work seriously. I learned then that one’s best friends are those who will tell you when you are wrong, as well as when you are right.
This skeptical attitude is helpful to a professional scientist. When my students or fellows were to make a scientific presentation or lecture, I encouraged my students and colleagues to ask: Is what I am saying clear? Is it true? Is it new? Is it significant?
AuntMinnie.com contributing writer, Copyright © 2006 AuntMinnie.com


 April 07, 2026
April 07, 2026