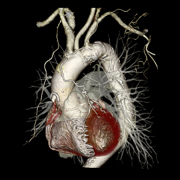
This 3-D image of a coronary artery bypass graft was acquired using variable helical pitch (vHp) scan mode on Aquilion 64.
Over the past decade, multiple-detector computed tomography (MDCT) scanners have transformed the imaging field. Systems such as the Toshiba Aquilion 64 provide physicians and patients with many diagnostic benefits, since they are a faster, less invasive modality for diagnosing various conditions. Even though the systems may be very expensive, studies and physicians are finding them to be increasingly cost-effective.
Tony DeFrance, M.D., clinical associate professor at Stanford Medical School, SCCT Board of Directors and a national director of SCCT workgroups, has been using various MDCT models since 2002. He is a strong believer that the technology could revolutionize medicine.
“[MDCT] has really become the workhorse of imaging,” he says, “and it will eliminate a large number of invasive tests.”
Seeing for the First Time
Although it still uses X-ray technology, an MDCT scanner rotates around the patient’s body, taking snapshots from thousands of vantage points and creating a virtual 3-D image of the target area. Using that dataset, physicians can rotate and view the desired area from thousands of viewpoints, which DeFrance says is impossible with a standard X-ray.
Since tissues have different densities, physicians can also virtually dissect and differentiate various organs, tissues or vessels.
“In the heart, that becomes very important because you’re able to tell different types of plaque or blockages in the artery,” DeFrance said. “So you can tell a cholesterol-filled plaque from a calcified plaque from a fibrous plaque.”
This makes MDCT the only technology available that lets a physician noninvasively see into the walls of an artery. Stress tests and other diagnostic methods only look at the end results.
Diagnostic Benefits
Chest pain alone does not necessarily signify an urgent need. So when a patient comes to the clinic with chest pain, physicians need to quickly determine whether the pain is due to one of three potential life-threatening conditions: coronary artery disease (CAD), an acute pulmonary embolism or an aortic dissection.
DeFrance said MDCT can quickly and noninvasively diagnose all three. In fact, the procedure is so fast that it often takes longer for the images to come up on screen than it does to perform the test.
As a result, MDCT has become what DeFrance refers to as an “excellent gatekeeper to the cath lab,” which benefits patients and physicians. Patients often need not undergo long, painful procedures, and physicians only need to perform them on those who need it most.
And although invasive cath procedures are very safe, they still carry a 2 to 3 percent risk of complications. With more than 1 million people having such procedures each year, MDCT could help thousands of people avoid major complications.
The benefits extend beyond the cath lab, too. The technology can be used to diagnose many different types of pathology, from cancers to gallstones to aneurysms.
In a cardiac setting, an MDCT scanner has an extremely high negative predictive value, meaning if a physician sees a normal study with no signs of disease, they can typically rule it out. This is especially helpful when the physician does not suspect coronary disease.
Additionally, even though an MDCT still exposes patients to radiation, the dose is much lower than a stress nuclear test or an invasive angiogram, which are often used in similar circumstances.
Despite the potential benefits, DeFrance stresses that MDCT is not the most appropriate modality for certain patient groups. These include patients with advanced or severe coronary artery disease. Typically, patients in this group have heavily calcified arteries and the scans have a hard time seeing through the dense deposits.
Cost Benefits
MDCT systems have a very high, and sometimes prohibitive, upfront cost. But DeFrance said studies are increasingly showing the technology is cost-effective and cost-efficient in both clinical and hospital settings.
Before an emergency room (ER) can properly diagnose a patient complaining of chest pain, it must administer and evaluate several tests, such as electrocardiograms (ECG), stress tests and blood tests. In the United States, the average chest pain evaluation takes between 12 and 14 hours. In many centers, that process takes even longer.
In the hospital setting, the goal is to diagnose, treat and release the patient as quickly as possible. Quicker tests translate into greater revenue. Although they have been relatively small, studies have shown MDCT can reduce the chest pain evaluation time by up to 66 percent, meaning the entire process could take as little as three hours.
Studies have also found that MDCT is more cost-efficient when compared to other modalities, meaning it is cheaper to use it to get to the diagnosis. At a minimum, they have found that MDCT can result in a 25 percent cost reduction.
However, DeFrance cautions that clinics must weigh several factors before purchasing an MDCT system. To begin with, the clinic must have a high enough patient volume to offset the initial costs. Also, it must consider the extensive training that technicians and physicians must receive to properly use and interpret the technology.
“The business model would need to be looked at very closely,” DeFrance said. “It’s an expensive piece of equipment.”
One way to combat the high capital cost is to share the machine among several departments.
“I think it’s fairly difficult, unless you have a very, very large cardiology group or cardiovascular imaging group to keep a machine economically viable with only cardiac CT,” DeFrance said.
A Bright Future
Despite the initial costs, MDCT does have several clear benefits. It can quickly and accurately let the physician look at things other modalities simply cannot see. It often rules out or takes the place of painful invasive procedures. Studies are starting to show that MDCTs are becoming more cost-efficient. Advanced versions also offer extremely high resolution.
Overall, DeFrance said the industry will continue to progress to MDCT as a noninvasive imaging system.
“I think it’s really going to end up being the fastest, cheapest way to evaluate chest pain, both in the hospital and outside,” he explained.


 April 29, 2026
April 29, 2026 









