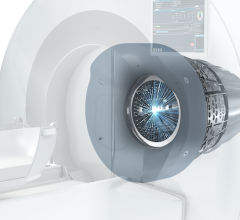
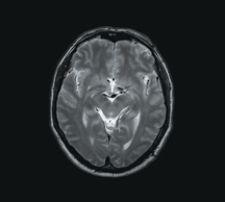
T2W TSE with 0.6 mm in-plane resolution acquired with 3.0 mm slices courtesy of Philips Medical Systems
The number of magnetic resonance imaging (MRI) procedures has grown at an average of 10 percent annually over the last 10 years, and there are no signs of stopping as continuous advancements in MR have generated more precise diagnosis for brain and cardiac imaging, bringing it to the forefront of cutting-edge imaging technology.
Ramping up the presence and power of MR in the future are 3.0 Tesla (T) MR systems, which have already gained access to the clinical environment, where physicians are leveraging its higher signal-to-noise ratio (SNR) to produce enhanced image quality and faster acquisition. As 3.0 T MR moves ever closer to becoming the gold standard, cost and implementation difficulties are holding back its complete adoption by the MR community.
The main prohibitive factor deterring a number of healthcare facilities from acquiring these systems is the high price tag of the 3.0 T MR. Among the facilities that may be left on the outside looking in for now are outpatient centers and mid-sized hospitals whose budgets may only allow for a 1.5 T system or one of even lesser field strength.
Experts note, however, that the prices of 3.0 T systems are beginning to drop and will continue to fall, eventually allowing more mid-sized hospitals and outpatient facilities the opportunity to reap the benefits of doubling their systems’ field strength.
High-Field MR Accelerates Neurological Imaging
Neurology is one field that is really beginning to apply the advantages of 3.0 T MR toward its diagnostic purpose. Increased SNR of high-field MRI allows more detailed visualization of smaller vessels in the brain. Using identical acquisition parameters, 3.0 T can show small vessels that are not even visible with a 1.5 T.
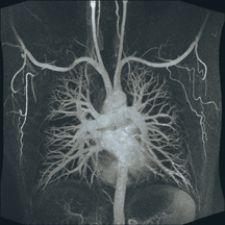
“[Increased field strength] is very good when you are trying to look at angiography of the brain, which is important for tumor growth because when you have tumors growing, they form their own feeding vessels,” said John Patrick, general manager, Philips MRI. “You can visualize that much better at a higher field strength.”
MR of any field strength can image both surface and deep brain structures with a high degree of anatomical detail, and can detect small changes in these structures. Also, a radiologist can discover how a normal, diseased or injured brain is working with functional MRI (fMRI). fMRI sees images of blood flow in the brain as it is occurring, allowing the visualization of changes in brain activity as patients perform various tasks, such as thought, speech, movement and sensation. The radiologist can then determine what part of the brain is used for each specific function, which can be a valuable tool for treatment planning.
Cardiac MR Proves Effective Over Other Imaging Options
3.0 T MR is being used in the cardiac imaging arena, but there is hope that the advantages of it’s improved SNR will be truly realized down the road. There is a current disadvantage of 3.0 T cardiac imaging when it comes to greater susceptibility artifacts, but research is being conducted to work out the kinks, and should be completed within the next couple of years. While radiologists wait for 3.0 T to clearly overtake 1.5 T, cardiac MR still has advantages over other cardiac imaging options such as echocardiography, nuclear medicine and computed tomography (CT).
“MR is a very flexible technology,” stated Warren J. Manning, M.D., professor of Medicine and Radiology, Harvard Medical School and section chief of Noninvasive Cardiac Imaging at Beth Israel Deaconess Medical Center. “The sort of bread and butter of MR is it is widely recognized as the most accurate technique for assessing the size and contractility of the heart, the size and contractility of the left and right ventricle and the atria.”
Compared to echocardiography, MR has enhanced definition of the borders of the chambers. About 15 percent of the time, all the walls of the ventricle cannot be seen with echocardiography, as opposed to being able to locate endocardial borders with MR 98 percent of the time. According to Dr. Manning, MR is far more quantitative than echocardiography with regard to the size of the ventricles.
Nuclear medicine is very good for perfusion and looking for global systolic function. However, MR can identify much smaller infarctions because of the spatial resolution advantage that it holds over nuclear medicine.
“MR doesn’t use radioactive tracers and gives us information about valvular heart disease in the right ventricle, which is not assessed by nuclear medicine,” added Dr. Manning.
The major benefit of cardiac CT over MR is that it is easier to implement and for physicians to train on, but it is not as flexible. CT’s technology for imaging the coronary arteries is also more developed. It is faster and easier, but at the current time, the accuracy for each is about the same. The quicker and easier acquisition from CT does come at a price however. Unlike MR, it exposes patients to a considerable amount of radiation and ionated contrast with the risk of renal toxicity and allergic reaction.
7.0 T MR Gains Interest on the Research Front
Preclinical research is currently underway on 7.0 T systems to determine how they will be most effectively utilized, and physicians have high hopes for the technology. GE Healthcare, Philips Medical Systems and Siemens Medical Solutions have all developed 7.0 T systems and are currently conducting research to determine how they will be used effectively if cleared by
regulatory agencies for marketing specific claims.
“To a certain extent they are preclinical research systems, and there are really several different thoughts on how they will be used the best,” said Patrick. “The neurodegenerative work is one area of keen hope for the technology. In 7.0 T, you would have more signal-to-noise ratio than a lower field strength machine.”
The ultra high-field strength of the 7.0 T systems more than doubles the field strength of its predecessors, yet, according to Patrick, the FDA has declared the level of significant risk at above 8 T. Over time, significant risk levels from the FDA may change as further research is conducted on emerging higher-field strength MR systems. This is not to say that magnet strengths above 8 T are dangerous, but that there has not been enough research completed to determine otherwise.
The ability to visualize previously unseen information in certain applications may be amongst 7.0 T most indispensable abilities.
“Like I said, you would increase the signal-to-noise and in some cases you increase the contrast noise,” said Patrick. “In some applications, they can give you, or may be giving you, additional information that you wouldn’t have gotten at the lower field strength.”
There are no signs of the 7.0 T systems becoming available for clinical use as they are strictly research platforms at this time. It has not been reviewed by the FDA for 510k clearance, and until then the exploration will go on.
As higher-channel MR systems evolve, and implementation becomes more widespread, neurology and cardiology will continue to see the advantages. 7.0 T research also gives a peek into the future of a technology that may be on the verge of becoming even better.


 April 28, 2026
April 28, 2026