
Getty Images
According to the American Academy of Pediatrics, as of October 6th, over 14.8 million children are reported to have tested positive for COVID-19 since the onset of the pandemic. Although the pandemic is subsiding, clinicians are observing that even after recovering from infection with SARS-CoV-2, many still seem to have long-term symptoms, including difficulty thinking or concentrating, headaches, dizziness and even lasting lung damage.
This gave rise to the term “long COVID” which now dominates the headlines. Numerous studies have been done, however there still seem to be more questions than answers. Diagnosing, treating and caring for long COVID patients has proven to be a challenge due to the list of characteristic symptoms that continuously evolves.
Low-field MRI Imaging
But what exactly is long COVID? The World Health Organization defines long COVID as symptoms that persist for a minimum of 12 weeks along with other factors, such as symptoms that result in a new health limitation or worsening of a pre-existing underlying medical condition.
Study of the disease’s long-term effects has accelerated as the number of COVID survivors climbs and more people are diagnosed with long COVID. A recent study, published in the journal Radiology, found that children and adolescents who have recovered from COVID-19, or have long COVID, show persistent lung damage on magnetic resonance imaging (MRI). Ferdinand Knieling, MD, specialist in pediatrics and adolescent medicine from the departments of Pediatrics and Adolescent Medicine at University Hospital Erlangen in Erlangen, Germany, is senior author of this study. Recently, we asked him to share some insight on long COVID, and his findings.
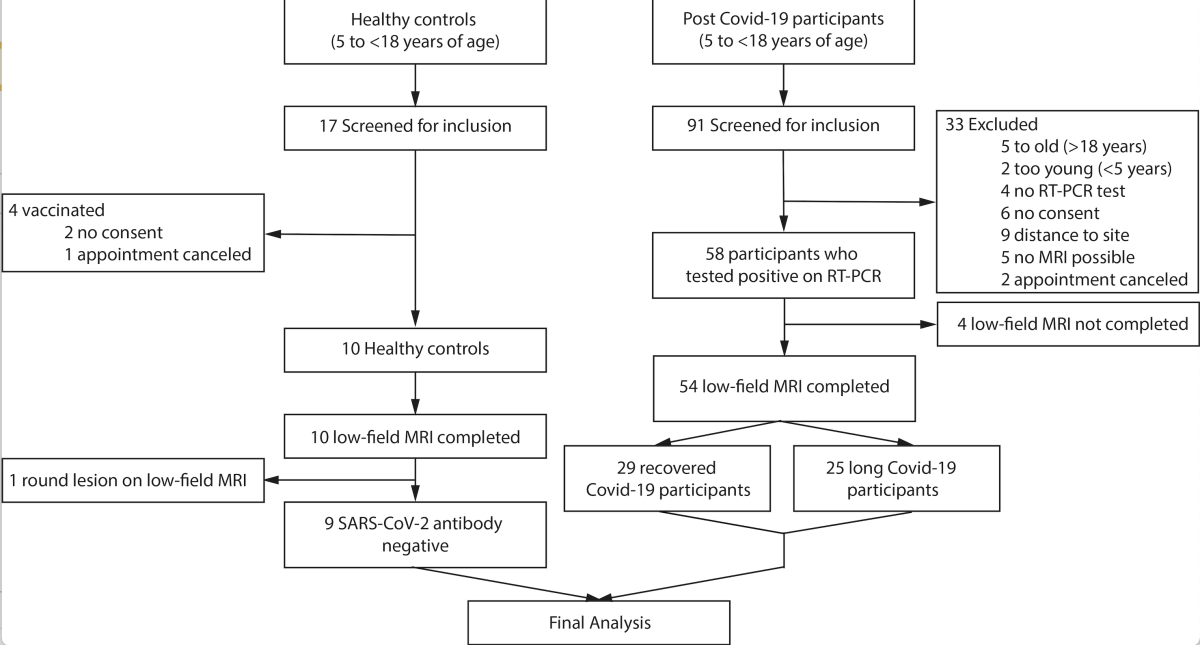
Figure 1. Flow chart of the study. Image courtesy of RSNA
Many past studies and imaging samples of COVID-19 were based on the use of computed tomography (CT). However, this study, titled “Pulmonary Dysfunction after Pediatric COVID-19,” was based on low-field magnetic resonance imaging (MRI) technology. Knieling explained that the nature of the post-acute phase of the infection is poorly understood in younger people. Computed tomography has shown persistent damage to the lungs in adults, but CT uses ionizing radiation and has limited diagnostic value in children, where lung changes due to COVID-19 are less pronounced.
“In our study, we used a new functional low-field MRI technique to examine pediatric and adolescent patients after COVID,” he explained. “The results of the study were compared with healthy children and adolescents. We found that both children and adolescents fulfilling the criteria for long COVID disease and those who subjectively had no symptoms after infection showed abnormalities of lung function on MRI. We could see that the regular function of the lungs — which is ventilation and blood circulation — were disturbed in contrast to healthy controls. The changes were still detectable months after first infection.”
Knieling said that low-field MRI technology was chosen because, unlike CT, it is completely radiation-free. The technology relies on a lower magnetic field than conventional MRI and no breath hold is required, which makes scanning more feasible in children. “It had already become apparent from the literature that mildly affected children and adolescents in particular might not show any abnormalities on CT,” he stated. “In contrast, the MRI enabled not only a very good imaging quality for the parenchyma but also a functional representation of the function — which is ventilation and blood flow.”
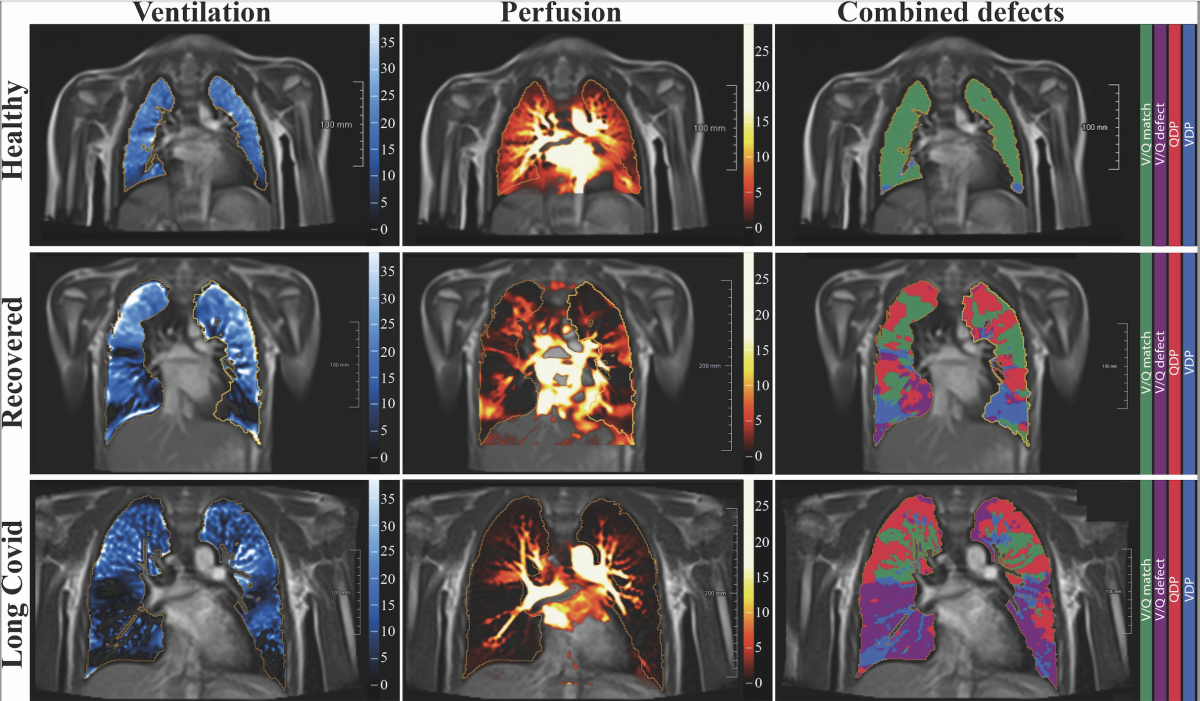
Figure 2. Free-breathing phase-resolved functional lung (PREFUL) low-field MRI at 0.55T with calculated parameters at an axial plane after automatic registration to a mid-expiration position and lung parenchyma segmentation. From left to right, representative color-coded images of functional show ventilation defects (VDP, blue), perfusion defects (QDP, red), ventilation/perfusion (V/Q match, green), ventilation/perfusion defects (V/Q defect, purple) in a healthy control (upper row, 7-year-old male), a participant recovered from COVID-19 (middle row, 10-year-old male) and a participant with long COVID (15-year-old male). Image courtesy of RSNA
The Multidisciplinary Challenges
The study looked at changes in lung structure and function in 54 children and adolescents with previous SARS-CoV-2 infection. Of the 54 patients, 29 had recovered, and 25 had long COVID. All but one of the patients had been unvaccinated at the time of original infection. Key findings coming out of this study showed that a large proportion of children and adolescents still show abnormalities in blood flow and ventilation to the lungs months after infection. “This is independent of the symptoms reported during or after the infection,” explained Knieling.
MRI allowed the researchers to derive the ventilation perfusion scan (V/Q) match, a measure of air and blood flow in the lungs. If lungs are working properly, both should match. Knieling stressed that their findings showed that caring for such patients presents a multidisciplinary challenge.
“First, it is a challenge for science. We still do not understand enough about the pathophysiology of long COVID disease. Especially as pediatricians we have the problem to distinguish this from other diseases. At the same time, there is a lack of clear therapeutic approaches and clinical studies. Much more support for scientifically structured approaches is needed here,” he said. “Second, it is a clinical challenge. We are already seeing an increasing number of patients who may be suffering from such disorders. We need to take this seriously and set up specialized outpatient clinics where families can receive broad, interdisciplinary support. This begins with the rule-out of possible other diseases and ranges to psychological or rehabilitative measures for affected families.”
Long-term implications of these lung changes remain unclear, but the results warrant further surveillance of persistent lung damage in children and adolescents after COVID-19, Knieling said. Lung MRI is already widely available, he noted, making these imaging approaches easy to integrate into clinical routine care. More research will help show the full potential of MRI in COVID-19 survivors.
“Unfortunately, some of our study participants are still only able to manage their daily lives to a very limited extent,” he shared. “Some suffer from pronounced pain that often worsens with exertion. Others actually have symptoms such as shortness of breath and only manage to walk very short distances. Some only manage to attend a reduced number of lessons at school. As described in the study, this contrasts with the other study group, who subjectively report no problems after infection.”
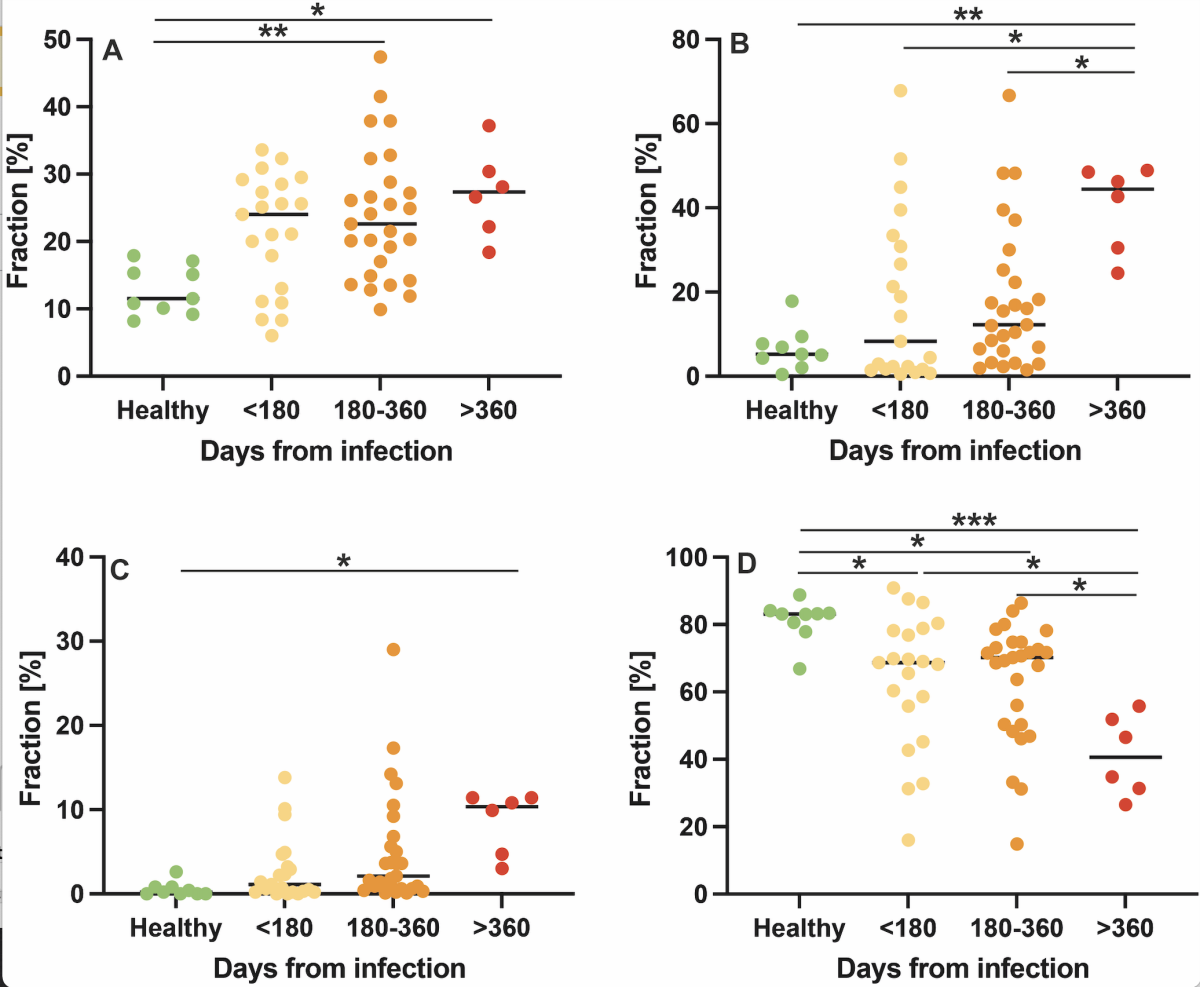
Figure 3. Comparison of low-field MRI parameters with respect to interval from first infection with dot plots for ventilation defects. The y-axis shows the fraction of defected or non-defected lung parenchyma on the automated measured axial plane. (A), perfusion defects (B), ventilation/perfusion match (no defects, C)) and ventilation/perfusion match (defect, D) in healthy controls, at less than 180 days, 180-360 days, and more than 360 days after SARS-CoV-2 infection. Image courtesy of RSNA
Finding New Diagnostic Approaches
There are some key takeaways from this study that the imaging community, pulmonologists and even cardiologists can learn from these outcomes, and help them treat post COVID patients better over time.
“We are still in the early stages of understanding what COVID infection means to the health of children and adolescents. However, we must keep in mind that the impact on younger patients — despite otherwise routinely unremarkable findings — can still be significant. Such new diagnostic approaches may help to better objectify and hopefully quantify the extent of subjective symptoms,” Knieling stressed.
Knieling’s study concluded that the results warrant further surveillance of persistent pulmonary damage in children and adolescents after being infected with the SARS CoV-2 infection. A follow-up trial has been started that takes a closer look at other organs, and how it correlates with previous findings.
“The new study aims to answer several questions: First, we examine at two time points 6 months apart to understand how the imaging findings may change over time. In addition, all participants will receive detailed cardiac diagnostics to better objectify potential individual performance limitations — and how the rate to MRI findings,” he concluded. “In addition, we examine the very small vessels by means of capillary microscopy. This should provide information about possible vascular involvement throughout the body. Furthermore, we examine the mechanical properties of the blood cells by means of a new high-throughput method.”
Related COVID Content:
Long COVID Implications: Increased Health Care Use After Infection With SARS-Cov-2
Lasting Lung Damage Seen in Children and Teens after COVID
PHOTO GALLERY: How COVID-19 Appears on Medical Imaging
COVID-19 Fallout May Lead to More Cancer Deaths
Kawasaki-like Inflammatory Disease Affects Children With COVID-19
FDA Adds Myocarditis Warning to COVID mRNA Vaccine Clinician Fact Sheets
CMS Now Requires COVID-19 Vaccinations for Healthcare Workers by January 4
Cardiac MRI of Myocarditis After COVID-19 Vaccination in Adolescents
Small Number of Patients Have Myocarditis-like Illness After COVID-19 Vaccination
Overview of Myocarditis Cases Caused by the COVID-19 Vaccine
Case Study Describes One of the First U.S. Cases of MIS-C
NIH-funded Project Wants to Identify Children at Risk for MIS-C From COVID-19


 May 22, 2026
May 22, 2026 









