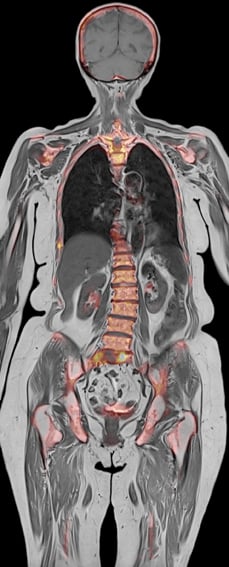
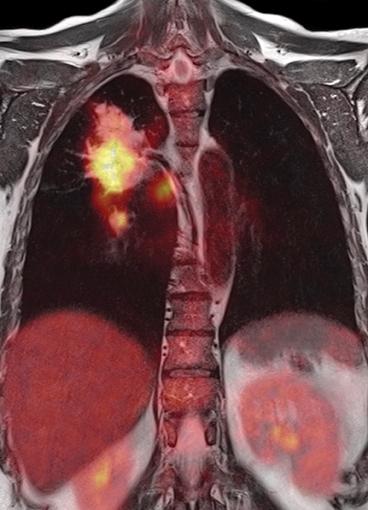
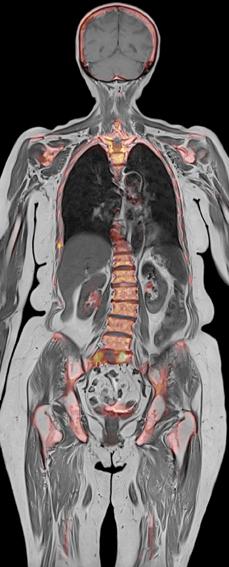
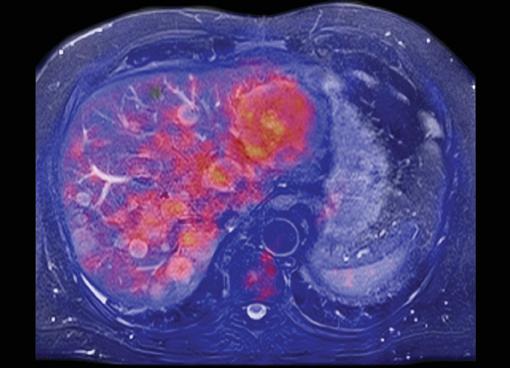
Lung imaging in a cancer case.
Creating the world’s first and only simultaneous whole-body positron emission tomography/magnetic resonance (PET/MR) scanner was no small feat for Siemens Healthcare. But when my engineering colleagues and I began that long, arduous development process more than half a decade ago, we believed that if we succeeded in building such a system, they — specifically, the clinical community — would come.
Clinicians have long recognized the potential of combining these two imaging modalities. MR yields morphological and functional details of the human body, while PET delivers valuable information regarding cellular activity and metabolism. The ability to visualize the anatomy, function and metabolic activity of organs in one image space, at the same point in time, held the promise of aiding physicians in identifying and staging malignancies, improving therapy planning and commencing with cancer treatment earlier than ever.
Clinical interest, then, was largely a foregone conclusion. Unfortunately, so were the formidable obstacles facing the 10-member team of Siemens developers back in 2008, when we set out to create what ultimately would become the Biograph mMR (PET/MR) system. Among those obstacles: How would the PET detectors of a simultaneous whole-body PET/MR system operate in the hostile environment of powerful magnetic fields? What could be done to prevent the PET system from degrading the world-class sensitivity of the Siemens MR receivers? How could MR images be used for PET attenuation correction? And how could the Siemens engineering team effectively reduce the attenuation of the major MR imaging components?
In short, Siemens would need to deliver a series of innovations that synchronized the MR and PET acquisitions and shielded the PET detectors from radiofrequency (RF) interference — while at the same time integrating those system components into the first system of its kind.
Getting Started
As the Siemens research team prepared to tackle those imposing questions, we were fortunate enough to be guided by expert manager Elmar Rummert, who previously led the development of key Siemens computed tomography (CT) systems. Establishing the Siemens Knoxville campus as our home base, my nine colleagues and I entered into an extended period of strenuous development. As systems engineer for the project, I was responsible for matters pertaining to hardware attenuation. Looking back on that time, I often joke that I disappeared around July of 2008 and reappeared about three years later. (My wife, incidentally, didn’t think it was quite so funny.)
Fortunately when it came to PET/MR research, Siemens had a head start — literally. The company had been developing a dedicated MR/PET imaging prototype for the brain — known as BrainPET — as early as 2004, when some of the engineers began designing solid-state, avalanche photodiode (APD)-based detectors that could operate in the magnetic field of an MR scanner. That experience with BrainPET was the engineering team’s foot in the door; it provided them with enough experience to convince Siemens to aim for a product rather than a prototype. This product would be a whole-body system with the delicate electronics of the PET detector again functioning inside the field of a 3.0 Tesla magnet. The potential advantages for a whole-body system were so enticing that Siemens shifted its development efforts immediately from the BrainPET system to the whole-body PET/MR project (which I dubbed “Mr. PET”).
Surmounting Challenges
A crucial factor in the success of the Biograph mMR was the fact that it was built on Siemens’ proven MR experience: our TIM (total imaging matrix) RF technology and 70 cm magnet technology. TIM facilitates seamless whole-body MR imaging; the magnet designed for a 70 cm bore provides room for a thin, solid-state detector assembly without compromising the size of the patient gantry (resulting in a 60 cm diameter bore).
Vaulting the project’s sizable technical hurdles was tricky, as many of our engineering decisions regarding Siemens’ simultaneous whole-body PET/MR system involved extensive research and yielded new and proprietary technologies. One early decision we faced was whether to cool the system detectors with water or air. We chose water, which proved to be the right choice. Ultimately, water revealed itself to be a superior coolant to air because of its heat capacity. Also, water can be delivered more precisely than air to a given point in the electronics assembly, whereas air is merely blown in the assembly’s general direction. Functionally, development aimed to keep the architecture of the MR system as consistent as possible with the stand-alone MR product. The development effort to make the MR compatible with PET came in less challenging ways; for example, selecting different materials for the patient handling system and moving MR electronics out of the imaging field of view to minimize photon attenuation.
Early in the genesis of the Biograph mMR, our engineering team developed solid-state PET detector technology with APDs that solved the problem of compatibility with the main magnetic field. Nevertheless, this development was a mega-challenge — solving the RF and gradient interference of MR with the PET. Inherently, MR gradients run hot, causing nearby PET detectors to be subjected to undesirable heat. Our solution, which was critical to the development of simultaneous whole-body PET/MR, required the addition of a specially designed cooling layer to the gradients. This was a significant MR system redesign. The problem of RF interference also required innovations — suffice it to say that we did much more than optimize the copper shielding.
To guide us to our solution of how to use MR images to correct for human attenuation, our engineering team was fortunate to have as reference the work of nuclear medicine visionary Axel Martinez-Möller, Ph.D. — then a doctoral research fellow at the Technical University of Munich and now a professor at that institution. Basing our efforts on his research, our team developed an algorithm to segment MR images into fat, soft tissue and air.
The Biograph mMR project also owed a major debt to our Siemens engineering colleague Yvonne Candidus, who redesigned several of the RF coils to reduce their attenuation. This feat involved moving RF circuits out of the way of the 511 keV photons and thinning the plastic housings. Without the willingness of both the Siemens MR and PET research teams to pursue significant redesigns of existing technology, we never would have been able to realize a finished product.
Testing and Implementation
I still clearly recall the day in the fall of 2009 when our team was first able to scan on our whole-body PET/MR prototype. When we realized that the system was stable, I felt confident. The prototype’s detector response was spatially uniform and linear with respect to the tracer’s activity over a huge dynamic range — that is, when imaging either low or high quantities of tracer, the system’s behavior was predictable. Both of those factors were critical to the project’s success.
By the spring of 2010, Siemens had installed a PET/MR prototype at the Institute of Medical Physics in Erlangen, Germany. That fall, roughly a year after evaluation of the first prototype, Siemens formally christened the system the Biograph mMR (or molecular MR) and unveiled it to the public, with the grand opening of the installation at of the Technical University of Munich in Germany. That November, it was introduced to the global imaging community at the annual Radiological Society of North America (RSNA) meeting in Chicago. Emerging from the intense development period in early 2011, I felt as though I woke up one day wondering what I would do with the rest of my professional life.
My answer was not too long in coming — I was presented with the opportunity to follow the Biograph mMR out into the field. The position involved serving as team leader for PET/MR research collaborations in the United States. Relocating from Knoxville to New York City, I now support research collaborations at Siemens customer sites such as NYU Langone Medical Center, which installed New York City’s first Biograph mMR in June of 2012. I have the pleasure of being surrounded by gifted physicians and scientists who have jumped at the chance to work on this cutting-edge hybrid system.
Continuing my work in the field with the very PET/MR system I helped create roughly half a decade ago has been extraordinarily gratifying. Having followed this “baby” out into the field, I’m watching it rise to prominence and am eager to see it give birth to a host of new clinical applications — applications that could enable physicians to diagnose and treat patients with greater confidence and increased efficiency. itn
David Faul, Ph.D., is a senior scientist at Siemens Healthcare and the former systems engineer of the Biograph mMR PET/MR system. He is currently based in New York City, where he serves as Siemens’ Biograph mMR collaborations manager for the United States.




 May 04, 2026
May 04, 2026