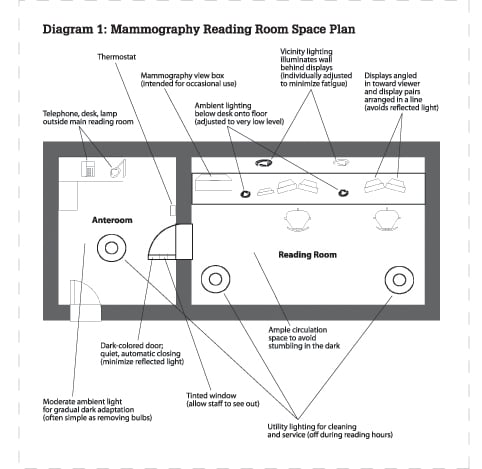
Diagram 1: Mammography Reading Room Space Plan
Millions of women are screened for breast cancer every year, resulting in tens of millions of X-ray images that need to be read. There are vast differences among today’s reading rooms, with many radiologists expressing concern about the conditions in either their workplace or the workplaces of their colleagues. Now that softcopy mammography screening is becoming commonplace, there is an opportunity to revisit the mammography reading room.
This article, based on a recent white paper, describes how to design a mammography reading room to ensure optimum results when screening digital mammograms.
Start by Setting Goals
The first step is to think about what you want to achieve in your mammography reading room. Typically, there are several goals:
• Read a large number of exams each year. High productivity implies an efficient workflow, i.e., minimal time per screening and fast turnaround of cases. “Radiologists surveyed agreed that three variables had the greatest effect on their productivity: ambient lighting, monitor brightness and the number of monitors available.”1
• Detect as many of the breast cancers as possible. The need to find and characterize subtle objects in X-ray images is a classic detection problem. The factors that largely determine the success of detection are radiologist experience, contrast and spatial resolution.
• Provide a comfortable work environment for the radiologists.
• Instill confidence in the quality of the work. Public confidence is very important, as women are more motivated to go to a screening exam if the screening center has a good reputation. A quality assurance (QA) process can ensure excellent quality, a good reputation and repeatable results.
Designing an Optimal Environment
It is common to find mammography radiologists working in a “production environment” in which they will screen exams for an hour or more without a break. Ideally, radiologists should be able to work undistracted, so that all of their attention can be focused on fast and accurate interpretation. Key factors in achieving the optimum reading environment include:
• Viewing height. The chair-table combination should be such that the eye level of the radiologist can be brought up, level with the top of the image.2
• Noise abatement. The room’s noise level can be controlled by several means. Acoustic tiles on the ceiling and carpet on the floor are traditional sound absorbers. The addition of quiet music is a possibility, but this is no substitute for noise elimination.
• Room temperature. The temperature of the room should be well regulated and individually adjustable from within the radiology suite.
What is the ideal arrangement of this comfortable room? Consider the rectangular room in Diagram 1. This design is constructed around the need to both control light and to provide a comfortable work environment. Important elements are:
• Diagnostic displays angled in toward the radiologist. This layout promotes maximum contrast and prevents near-vision deficits by equalizing the distance to all parts of the displays.
• Multiple workstations and any view-boxes are arranged in a single line. There is an important reason for this. If the light from another display falls on the display in use, it will reduce the contrast of that display.
• Ambient vicinity lighting is placed to illuminate the wall behind the displays. This illumination minimizes the fatigue associated with looking back and forth between dark and bright.
• Utility lighting is required for cleaning and service. This is only used during display maintenance.
• The illumination in the anteroom should be moderate — a compromise between the nice, bright typical healthcare environment and the very dark reading room. It can often be achieved simply by taking out one of the bulbs in the overhead lights.
• Walls should be a medium or dark color. Many people are happy with a yellow or orange-yellow paint color for the wall behind the displays.
• Carpeting to absorb both sound and light.
Contrast Ratio of Mammography Film and Displays
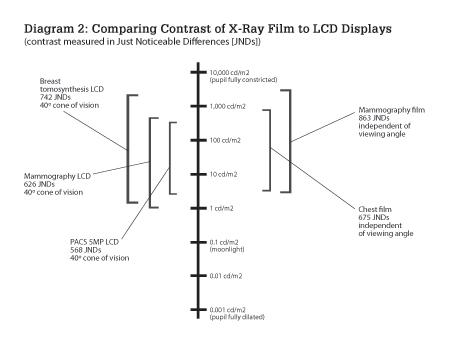
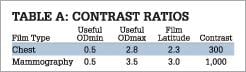
The characteristics of mammography film relate very strongly to the ergonomics and design of the mammography reading room. Softcopy displays are measured in contrast ratio; mammography film is measured in optical density. The contrast ratio equivalent to mammography film is about 1,000:1. Specialized softcopy displays used for mammography allow similar brightness and contrast. (See Table A for an example.)
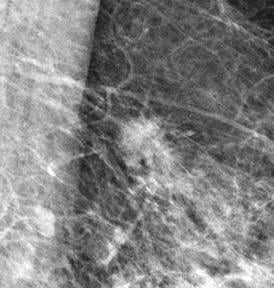
Why do mammography films have such a high-contrast range? Low-contrast calcifications and masses are difficult to detect. Objects are easier to detect when this slight contrast difference is amplified. This effect is well quantified in the concept of just-noticeable-differences (JNDs).3 The perceived contrast of a subtle object is greater when the overall dynamic range of the object is increased. (See the photos for an example and Diagram 2 for a comparison of contrasts.)
Ambient Lighting a Critical Factor
Ambient light is the single most important factor in productivity. The Mammography Quality Standards Act (MQSA) requires that ambient light should be kept to a minimum in the room where images are evaluated.4
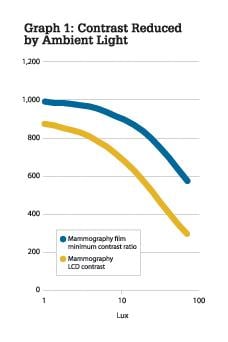
In Graph 1, the greater sensitivity to ambient light of the LCD is shown. With ambient illumination above 10 lux, the LCD begins to exhibit decreasing levels of contrast, resulting in a brighter black level than that portrayed in a typical mammography film on a view box. A reasonable level of ambient illumination when using displays of 500-600 cd/m2 is 5 lux. With brighter displays, proportionally more ambient illumination is appropriate.
When measuring the ambient light with an illuminance meter, the meter should be held flat on the surface of the display, aimed out toward the radiologist. The meter integrates light from all directions. Some displays include an illuminance meter. If the built-in meter has an integrating hemisphere, then it will be able to collect light equally from all directions.
Dedicated Mammography Displays
The perfect reading room for digital mammography also includes medical display systems that feature excellent imaging performance and high contrast over a wide viewing angle to optimize mammography screening.
Important considerations include:
• High brightness 5 megapixel displays. The higher the calibrated brightness, the higher the perceived image contrast. LCDs specifically designed for mammography should include features like pixel uniformity, long-life lamps and compensation for motion blur on cine images.
• Display controller with a large frame buffer. The memory and GPU on the display controller should enable extremely fast image download of large mammography studies. Other important features include: Expanded grayscale, up to 1,000 simultaneous shades; acceleration of critical functions like window/level and cine; and the ability to instantly flip between “hangings.”
• A software package for softcopy QA that allows remote review of quality control results.
• Medical-instrument quality video cables capable of perfectly transmitting the high-speed pixels.
Quality Assurance the Final Key
The two most important aspects of a quality control system for mammography displays and the reading room itself are having a well-defined procedure and a responsible person with sufficient interest and authority.
Softcopy QA products and services are widely available with softcopy display systems. An agent, installed on each softcopy workstation, allows automatic QA tasks to be scheduled and records all results in easy-to-read tables and graphs. A server allows secure, Web-based control and monitoring of all the softcopy medical displays in the entire facility or even system of facilities.
With the combination of a QA agent and server, a facility can add softcopy QA without adding much to the workload of its QC technician.
Albert Xthona is the product manager for mammography display systems at Barco. He collaborates with the engineering team and clinical experts in radiology to develop specialized equipment for cancer screening. Xthona has been an invited speaker at conferences in Europe, Asia and the United States on the topics of mammography displays and quality control.
References:
1. Optimization of Filmless Radiology Room Design: Survey Results of Experienced PACS Users. Eliot Siegel et al., June 2000.
2. OSHA Publication 3092, 1997.
3. ACR-NEMA Gray Scale Display Function Standard
4. Mammography Quality Standards Act, 42 USC § 201:262b Pub L No. 102-539 (1992)
Sidebar:
Mammography Reading Room Checklist
• Room layout with good traffic flow
• Viewing equipment oriented in a linear fashion
• Displays with high brightness and contrast
• Ambient light below 10 lux
• Adjustable vicinity lighting
• Ergonomically configured chairs and table height
• Noise levels below 45 dB
• Adequate airflow
• Utility lighting
• Thermostat and temperature control
• Quality control procedure
• Quality assurance responsibility
For additional reading:
• “Cornell Digital Reading Room Ergonomics Checklist,” http://ergo.human.cornell.edu/AHProjects/Hronn06/CDREC.pdf
• “Rethinking the Radiologist’s ‘Office’”, Gerald R. Kolb, JD, http://www.anthro.com/images/ergonomics/CarlTable_byGeraldKolb.pdf
• “Practice Guideline for Determinants of Image Quality in Digital Mammography,” American College of Radiology, Oct 2007
• “Computer-Aided Design and Modeling of Workstations and Radiology Reading Rooms for the New Millennium,” Ratib et al, November 2000 RadioGraphics, 20, 1807-1816.


 May 07, 2026
May 07, 2026 









