
Breast cancer screening has been on the forefront with the issue of breast density taking center stage. However, controversy surrounds the many contradicting studies that currently dictate the standards for breast cancer screening.
At the recent 25th Annual Interdisciplinary Breast Center Conference (NCoBC), Sarah M. Friedewald, M.D., division chief of breast and women’s imaging, and medical director at Lynn Sage Comprehensive Breast Center, Northwestern Memorial Hospital in Chicago, discussed the main criticisms of screening mammography. These include recommendations by the United States Preventive Services Task Force (USPSTF) and the Swiss Medical Board, as well as concerns regarding overdiagnosis of breast cancer and the survival benefit in women who have been screened.
Mammography is only approximately 70 percent sensitive for all breast types. For women with dense breasts, it’s even more limited — closer to
50 percent.1 According to Friedewald, because of these major differences in standard mammography, the limited sensitivity and high recall rate, traditional mammography has been highly criticized.
USPSTF Recommendations
The USPSTF was formed in 1984 as an independent volunteer panel of 16 members, with a mission to improve the health of the U.S. population. These members specialized in prevention and primary care, and targeted areas such as behavioral health, family medicine, geriatrics, internal medicine, pediatrics, OB/GYN and nursing. The task force made evidence-based recommendations about clinical, preventive services such as screening, counseling services and preventive medicine.
In 1998, the Agency for Healthcare Research and Quality (AHRQ) was authorized by Congress to convene the task force and provide ongoing scientific, administrative and dissemination support. It continues to provide an annual report for Congress, which includes critical evidence gathered in research that relates to clinical preventive services, and also recommends key areas that deserve further examination. The result is a scorecard that was released in 2009, which is currently in the process of being updated. The new USPSTF set of recommendations is anticipated to be released this summer. In late April, USPSTF declined to expand its recommendation on which women should receive regular mammography screening, instead issuing a draft of new breast screening guidelines that parallel its 2009 findings. According to the U.S. Preventive Services Task Force website, the task force’s draft recommendations are designed for women 40 and older who do not show any signs or symptoms of breast cancer, who have not been previously diagnosed with breast cancer and who are not at high-risk for breast cancer, meaning they do not have a known genetic mutation or a history of chest radiation at a young age. Women at high-risk of breast cancer should consult their doctors for individualized recommendations regarding screening. It goes on to say that the task force recognizes mammograms can help women in their 40s reduce the risk of dying from breast cancer. Because the risk of developing breast cancer is lower in women under 50, the potential benefit of mammography for women under 50 is also smaller, according to USPSTF.
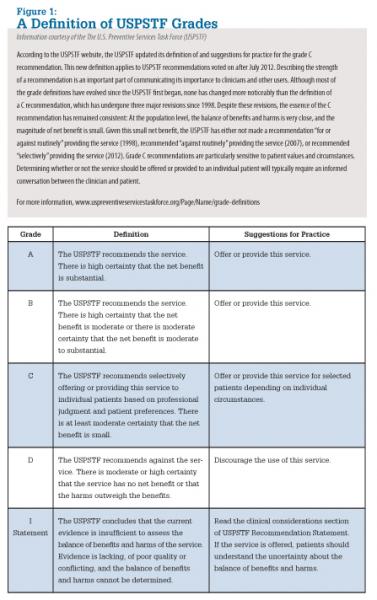
As of April 20, 2015, the USPSTF screening recommendations were proposed as follows. For a complete definition of what these grades mean, see Figure 1: A Definition of USPSTF Grades.
Women ages 50-74
The USPSTF recommends screening mammography every two years for women ages 50 to 74 years.
B recommendation
Women ages 40-49
The decision to start screening mammography in women before age 50 should be an individual one. Women who place a higher value on the potential benefit than the potential harms may choose to begin screening between the ages of 40 and 49 years. C recommendation
Women 75 and older
The current evidence is insufficient to assess the balance of benefits and harms of screening mammography in women 75 years and older.
I statement
In a rebuttal to these new proposed recommendations, the American College of Radiology (ACR) and Society of Breast Imaging (SBI) have issued a statement saying that adoption of the proposed USPSTF breast cancer screening recommendations draft would result in thousands of additional and unnecessary breast cancer deaths each year. Thousands more women would experience more extensive and expensive treatments than if their cancers were found early by a regular mammogram. Adoption of these USPSTF recommendations could also strip millions of women over 40 of private insurance coverage with no copay for mammograms at the time of their choosing previously guaranteed by the Affordable Care Act (ACA).
Friedewald explained that according to the 2009 recommendations, it claimed that the harm of the screening outweighed the benefits, and there was psychological harm and unnecessary imaging tests for women without cancer, a significant inconvenience to the false positive screening results, and an overdiagnosis of cancer.
“I’m going to tell you a little bit about the USPSTF,” said Friedewald. “There were no oncologists, radiologists or surgeons on the committee, none of the members were involved in breast cancer care, and their recommendations really were for average-risk women, which I think gets lost in the shuffle here. So we have a lot of women who are at high risk, but a lot of people just latch on to these recommendations and think that they are for everybody.
“This review was based on data going back to 1963, rather than gathering new information, so there wasn’t a big study that came out that led to these new recommendations,” she continued. “Their data did not incorporate digital mammography. Interestingly, they were commissioned by Congress to determine the recommendations, but that was also the same year that the Affordable Care Act was passed into law. So there are some questions as to what the motivations were of the USPSTF.”
To break this information down further, it’s important to look at the recommendation for screening given at age 50. “Age 50 is an arbitrary threshold not supported by trials, and it was historically chosen because it was a marker for menopause,” said Friedewald, explaining there is a concept of breast cancer being related to hormonal status. “But again, there is no data to support that screening should be given starting at age 50. In fact, we have data showing that it really should begin at age 40. We also did dispute the fact that there was a 15 percent reduction in mortality of women in their 40s, but they felt that the absolute number of women benefitting was small because of the incidence of cancer in that age group. There are varied numbers of people in this age group depending on the population at this time. So with the baby boomers, there were a lot of women in this age group; just because there may be a lower incidence, there still may be an absolute large number of women in this age group that would benefit from screening.”
That’s starting at age 50, but what about bi-annual screening? The difficulty with this, said Friedewald, is that it decreases the opportunity to identify cancers at an earlier stage. She suggested that optimal screening time for women really should be half the sojourn time. Sojourn time is defined as the time between a tumor first becoming mammographically visible and the moment when the tumor was actually detected by mammogram.2
“The longer the screening intervals make the screening less effective. It’s important to recognize what the sojourn time is,” stressed Friedewald, explaining why screening every other year is problematic. “Estimates for the sojourn time are dependent on multiple factors, but the study done at Mass General used a median doubling time of 130 days and we were able to calculate the mean sojourn time for invasive breast cancers at 1.7 years. The USPSTF concluded that the harms could be cut in half if there was a change to biannual screening, but the benefit would be reduced if greater than 24-month intervals between screening. They obviously didn’t recognize the issue of sojourn time.”
CNBSS Study
Another controversial study is the Canadian National Breast Screening Study (CNBSS), where nearly 90,000 women participated. It was a prospective randomized control trial for women aged 40 to 59, broken down into two groups: women who had physical examinations plus screening mammography, and women who had a physical exam and usual care after the initial physical examination without screening. The patients were divided into two age groups: women in their 40s and women in their 50s. These seven-year results were published in 1992.
“Their conclusion was screening with yearly mammography plus physical examination decreased significantly more, with no negative small tumors in the control group, no impact on the rate of death of breast cancer up to seven years follow-up from entry,” said Friedewald, stressing that a greater than seven-year follow-up is needed because a statistically significant number of women will need to die to demonstrate a benefit in the group. “Seven years is basically too short to show that there was no statistically significant difference in mortality.”
A 25-year follow-up was conducted on patients in this study, and their conclusion was the same: It did not reduce the mortality of breast cancer beyond that physical examination and usual care, when screening for breast cancer is readily available.
“Let’s dive a little bit deeper into the problems with this study,” said Friedewald. “There was poor randomization, all women had a physical examination prior to participation, allocation was not blinded and randomization was performed
by a study coordinator at each of the study’s
15 sites. I think what shows proof of this is there is an excess of node-positive women in the screened group, which was statistically significant, and the survival in the control group was better than expected.” She explained that this meant there were healthier people in the control group, more than anticipated, and there were more serious cancers in the screened group. In addition, there was contamination and non-compliance.
Friedewald went on to explain that the quality of imaging was poor, the technologists weren’t taught proper positioning and the radiologists had no specific training, which left it open for interpretation. “And then finally there was the separation of the two age groups. The women in their 40s really lacked the physical power, there weren’t enough people in those groups to show statistical significance,” she said. “There is no biological significance between the two age groups. For example, women who are age 49 are not statistically different from women who are 52.”
Overdiagnosis
In a paper published in JAMA, Laura Esterman, M.D., discussed the difficulties of overdiagnosis, which Friedewald summarized in her presentation, saying that physicians, patients and the general public must recognize overdiagnosis as common, and that it occurs more frequently with cancer.3
“So what is overdiagnosis? The concept is that many cancers detected by mammography are not clinically significant and do not cause death in patients,” said Friedewald. “When we’re talking about overdiagnosis we’re usually referring to ductal carcinoma in situ (DCIS). But it’s very difficult to estimate overdiagnosis because at the time of diagnosis, you can’t tell whether it’s a problem concerning a lesion or not. It really can only be estimated by the excess of incidence of breast cancer over a long period of time when you are screened compared to those who were not.”
Many estimates wrongfully state an increased incidence of cancer in the screening group because they don’t have enough lead-time bias. “Screening mammography detects cancers prior to being clinically evident, but at the beginning of the screening program prevalent cancers get incorporated with the incident cancers because they are detected earlier, and by physical examination,” said Friedewald. “There’s a false sense that there are actually more cancers, but there is no change in the state of depth. That’s really what the lead-time bias is. So not only do they not account for the lead-time bias, but there is also too short of a follow-up.”
It’s important to keep in mind that the incidence of invasive breast cancer is decreasing over time — about 1 percent per year, said Friedewald. “This is likely due to environmental factors, medication, increase in age, childbearing and the number of children a woman has,” she explained. “It’s not clear that all DCIS at some point will progress to this invasive cancer, or whether it will just stay as DCIS. So at the time of diagnosis we don’t have any way of knowing which ones will be the ones that are going to hurt the patient and which ones are not.”
Friedewald said the focus should be on the understanding of molecular characteristics of DCIS so physicians can better understand the behavior of those cells and modify a treatment, rather than not screen patients.
Swiss Medical Board Assessment
The Swiss Medical Board, an independent health technology assessment board, prepared a review of mammography screening which was released in February 2014.4 This task force consisted of medical ethicists, clinical radiologists, surgeons and clinical pharmacologists. They published their perspective in the New England Journal of Medicine. Friedewald explained that their conclusion recommended against screening completely. They felt that the survival benefit may not be related to screening, citing studies from 1963-1991 showing a 20 percent reduction in mortality with screening mammography.
The Swiss Medical Board concluded that the harms of screening mammography outweighed the benefits. They based this conclusion, in part, on a Canadian study that showed 22 percent of cancers were “overdiagnosed,” and there was no mortality decrease. They also cited that in a survey of women’s perceptions, women overestimate the value of mammography versus its actual benefit.
Current U.S. Screening Recommendations
According to the American Cancer Society (ACS), American College of Radiology (ACR) and the American Congress of Obstetricians and Gynecologists (ACOG), annual screening mammography can begin at 40 as long as the woman is in good health.
The ACS recommends that for early breast cancer detection, mammograms are a substantial benefit for women in their 40s, noting that mammography will miss some cancers, and sometimes can lead to follow-up, including biopsies, that are not cancer.
“Women should be told about these benefits and limitations, and mammograms for older women should be based on the individual’s health and other serious illnesses such as congestive heart failure, end-stage renal disease, chronic obstructive pulmonary disease and dementia,” Friedewald said. “Age alone will not be the reason to stop having a regular mammogram.”
References
1. Bird, RE, Wallace TW, Yankaskas BC. “Analysis of cancers missed at screening mammography.” Radiology 1992. 184:613-617.
2. Querci della Rovere, G, Warren R, Benson J. “Early Breast Cancer” Second Edition, Taylor & Francis Group, 2006.
3. Esserman, L. “Viewpoint: Overdiagnosis and Overtreatment in Cancer: An Opportunity for Improvement.” JAMA Aug. 23, 2013. Volume 210:8.
4. “Abolishing Mammography Screening Programs? A View from the Swiss Medical Board.” New England Journal of Medicine. May 22, 2014.


 May 07, 2026
May 07, 2026 









