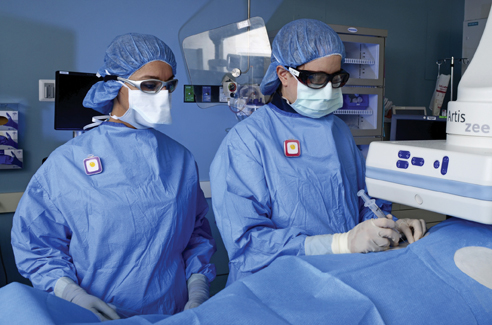
Staff at Lawrence General Hospital are wearing the RaySafe i2 color-coded dosimeters to monitor personal radiation exposure while performing a procedure.
It’s the invisible elephant in radiology — radiation exposure. As physicians, we know all too well that exposure to radiation should be limited to the least amount possible. We have all learned about the ALARA principle for keeping exposure low. We also take precautions on our patients’ behalf and educate them. But what about us? The physicians and technical staff who treat patients every day cannot avoid radiation exposure entirely. However, there is growing evidence that not only is radiation exposure detrimental to our health, but also many long-term cumulative effects are still unknown.
According to the National Council on Radiation Protection and Measurements, diagnostic imaging tests have increased Americans’ average radiation exposure seven times since 1980, and increased exposure has been shown to increase cancer risk. Recent research shows interventional radiologists and cardiologists have at least three times the risk of left side brain tumors than the general public, a truly startling fact. I personally know of at least two interventional radiologists who have died from brain tumors.
So what are we as physicians and technologists to do about our desire to ensure our patients get the best possible treatment without jeopardizing our own health?
Education, Awareness and Precautions
At best, physicians can monitor their exposure and take precautions to mitigate it. Traditionally, that means being aware of the proper collimation, positioning and angling of the equipment in order to decrease the dose exposure to staff. It also requires wearing the proper, sometimes awkward or cumbersome, protective gear. Additionally of course, there are warning signs posted on walls to remind staff to work responsibly. Now, however, there is new technology that could make people think about what they can’t see. Radiation is invisible. I believe people just don’t think about threats they cannot see.
Healthcare organizations have been mandated to provide some level of protection to staff such as lead vests and lead goggles. Protective surgical caps are also gaining popularity in the imaging community. The use of such protective gear relies on awareness, training and enforcement. Arguably, those are the variables that could mean the difference between a dangerous dose of radiation or a safe and long career. Over time, repeated exposure carries long-term effects, the extent of which are still being discovered.
For our patients, there are organizations that advocate for patient safety such as Image Gently for pediatric care and Image Wisely for adults. It’s a great example of the industry coming together from all vantage points including organizations, healthcare professionals and vendors.
But the move to advocate for physicians is somewhat of an uphill battle. And that has a lot to do with changing a mind-set. In an industry previously dominated by innovation above all else, the consensus has too often been “nothing bad will happen to me” or “the treatment advances are more important.” Many would turn a blind eye to the reality that too much exposure to radiation — even low dose exposure over a long period of time, such as the life of a person’s career — is harmful, regardless of gender. Just over 80 years after Marie Curie died from radiation exposure, let us not forget her wonderful accomplishments that made our profession possible, or her unfortunate example of how important radiation protection can be.
Media Influence
Understandably, we as physicians need to make a stronger push for change, and although that push needs to come from us, we also need to engage the media to get our collective voices heard.
For example, in California, a well-known Los Angeles hospital disclosed that it had mistakenly administered up to eight times the normal radiation dose to 206 possible stroke victims over an 18-month period. State and federal health officials were involved in the investigation that followed. Also in California, a 2 ½-year-old boy complaining of neck pain after falling off his bed was subjected to over an hour of CT scans. These are egregious situations, but they can be used to heighten awareness and elevate the conversation. Instead of whispered concerns in the hallways of the radiology department and among members of the interventional community, heightened awareness should be brought to the level of national consciousness.
Those cases draw much-needed media attention to the industry and technological advances that can be implemented to make everyone safer. We need the same media awareness to pursue and pressure the change for physician safety.
Technological Advances
One of those advances in technology now allows radiation exposure to be monitored in real-time while physicians and technical staff treat their patients.
When the opportunity presented itself to install a new interventional radiology suite at Lawrence General Hospital in Lawrence, Mass., I made sure it wasn’t only with the patients’ care in mind. It was important for me to also protect the staff.
When I was attending my fellowship at INOVA Alexandria Hospital in Alexandria, Va., there was a strong emphasis on the seriousness of radiation exposure and the proper precautions that need to be taken to mitigate the effects of exposure both for the staff and for the patients.
I understand a physician’s dedication and desire to get the best result for the patient, but being too close to the patient during a procedure has many risks. Emerging data shows the clear connection between cataracts, thyroid cancer, breast cancer and even increased instances of left-side brain tumors among radiologists. I strongly advocated for the installation of a RaySafe i2 system from Unfors RaySafe, Hopkinton, Mass., because it was a way to make radiation exposure increasingly visible to the staff. I had to make them aware so that they would decrease their dose. Thanks in large part to the hospital administration’s forward-thinking desire to protect their staff and to Debra Ralls, RTR, MBA (director of radiology) for her assistance in my petitioning of the administration, the one-of-a-kind system was incorporated into the new interventional radiology suite.
The staff’s response was immediate. As soon as they saw real-time what was going on they were quite motivated to participate. In fact, colleagues were keeping an eye on each other’s levels, advising one another to step back if exposure was unnecessarily reaching a high level.
The conversation about awareness and care, since the system was installed, has spread outside of the interventional radiology suite and people are starting to take notice. In fact, the hospital is considering putting the system into several suites that are currently under construction in a new OR and the cath lab. Since the vascular surgeons have seen it in use, they want it in the new suite, too.
This is an occupational health issue. I want to help raise awareness and protect the young people entering this industry. If somebody were going to hit you, you would instinctively protect yourself because you see it coming; it’s no different with radiation exposure. We know it is happening and we know there are sophisticated ways to track it and reduce the exposure over the course of a career. When you can see it, you can do something about it.
It was eye-opening for the staff. They feel more supported now that they realize this was put in for them, which creates a good working relationship with the facility. With the dose monitoring solution in place, each staff member wears a lightweight badge called a dosimeter to measure and record radiation every second. Dose data is transferred wirelessly to the real-time display, which then displays a bar with colors based on real-time exposure. The dosimeter can be personalized with different names and badge colors.
These types of advancements in technology in the radiological industry will no doubt help future generations of physicians. I’ve been practicing for 11 years, and already have three times the risk of getting a brain tumor than the general population. But that reality won’t stop me from advocating for a better way to do things, which necessitates true culture change. And one of those things is insisting on more studies; the results of those studies should be shared not only with the medical community, but also the general population.
You shouldn’t have to kill yourself to treat your patients. With the correct protection you should be able to do what you love and remain healthy.
Lori M. Weir, M.D., specializes in vascular and interventional radiology. She was a resident in diagnostic radiology at St. Lukes-Roosevelt Hospital (Columbia University) in New York City from 2000-2004, and then an interventional radiology fellow at INOVA-Alexandria Hospital in Alexandria, Va., from 2004-2005. After several years at a large tertiary care practice in Dallas, she came to L&M Radiology in 2009.


 May 26, 2026
May 26, 2026 









