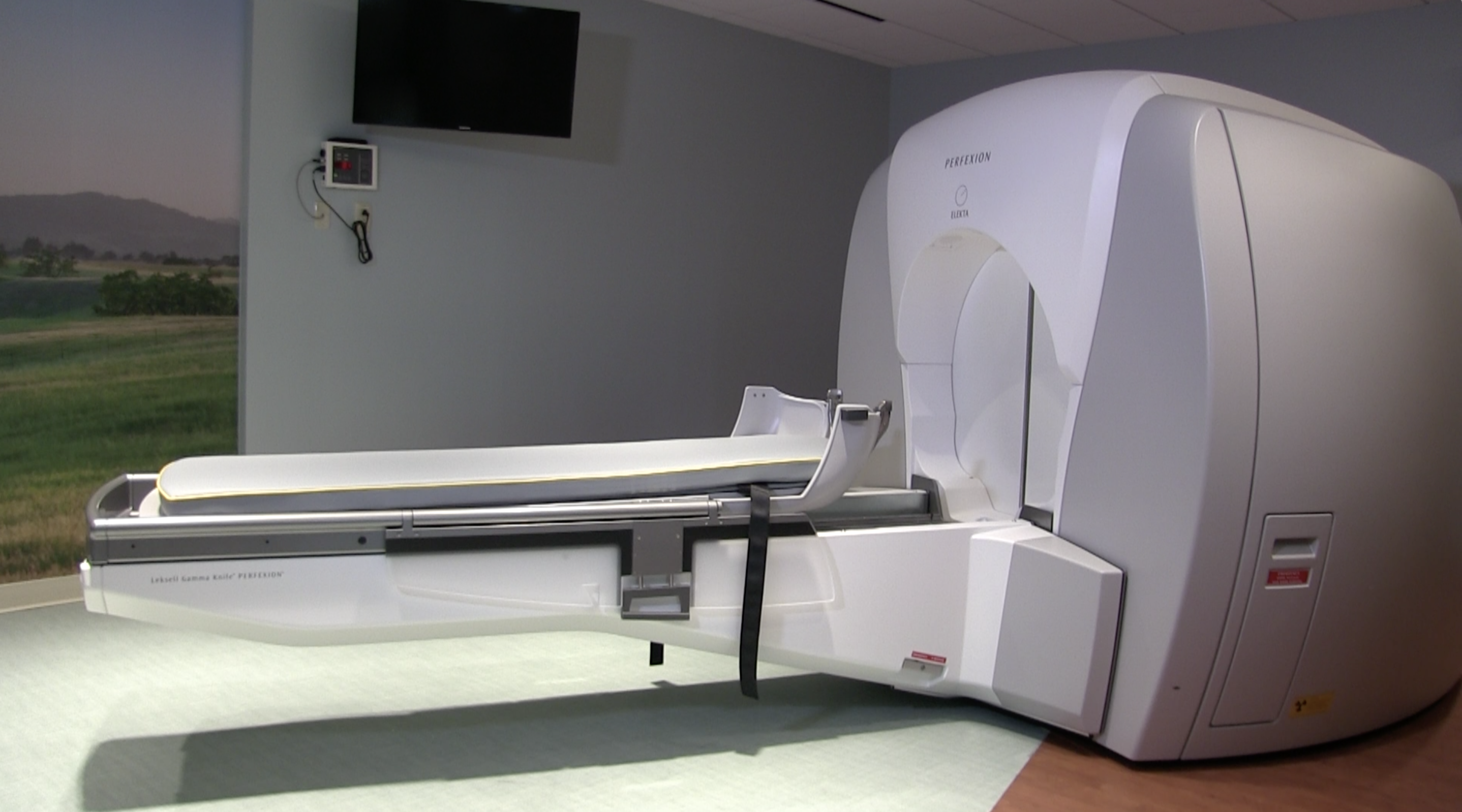
Gamma Knife radiosurgery has become the preferred radiation therapy option for patients with brain tumors at facilities like the Northwestern Medicine Cancer Center, pictured here. The technology is favored largely for its ability to precisely target tumors while sparing healthy tissue.
Brain tumors are some of the most complicated forms of cancer to treat due to their extremely sensitive location. Surgery is the first choice when possible, as it guarantees removal of the tumor. Brain surgery is, however, an extremely invasive procedure and requires weeks to months of recovery time for the patient. Radiation therapy offers a minimally invasive alternative, but it comes with its own set of side effects and complications, including cognitive issues, fatigue, and hair and scalp problems, among others. According to the National Brain Tumor Society, however, only four drugs and one device have been U.S. Food and Drug Administration (FDA)-approved to treat brain tumors in the past 30 years.1 Today, there are several new technologies and investigations into existing technologies offering hope for improved patient care.
Hippocampal Sparing Improves Whole-brain Radiotherapy
Whole-brain radiotherapy (WBRT) has typically been a last resort for brain tumor patients because by nature it is harder to minimize dose to healthy tissue. This can also lead to memory issues for patients. “Obviously, [treatment] is a balancing act and in many scenarios involves choosing a more potent but more toxic treatment over a less potent but gentler option. In this case, WBRT is both less potent and more toxic,” said James J. Urbanic, M.D., a radiation oncologist and associate professor of radiation medicine and applied sciences at the University of California San Diego.
Despite these concerns, certain clinical scenarios still require use of WBRT — usually based on the number of lesions or if there is doubt about hidden lesions, according to Vinai Gondi, M.D., director of research and central nervous system (CNS) neuro-oncology at the Northwestern Medicine Cancer Center in Warrenville, Ill. To try to enhance patient care in these scenarios, Gondi and a team from Northwestern investigated using WBRT while sparing the hippocampus, a central region of the brain that regulates both short- and long-term memory.
For the study, 518 patients with brain metastases were randomized to receive whole-brain radiotherapy plus memantine (a drug that alleviates cognitive side effects from radiation), and the hippocampus was either spared or not. Total dose for both groups was 30 Gy over 10 fractions. The hippocampal sparing group had a 26 percent relative reduction in cognitive toxicity risk, and the time to neurocognitive failure (as determined through various neurocognitive tests) was significantly higher for this group as well.2
“This study demonstrates that we can deliver whole brain radiotherapy with similar cognitive outcomes as radiosurgery,” said Gondi. “These trial results revolutionize our understanding of the cognitive effects of brain irradiation in a manner that has far-reaching implications in terms of the safer radiotherapy treatment of primary or metastatic brain tumors.”
Gondi said this study may just be the tip of the iceberg for enhancing the utility of WBRT. “We believe that [the hippocampus] is very sensitive to radiation — even very low doses of radiation — because it houses neuro stem cells that are specific to memory formation. So that has a significant impact on all brain tumors that we manage, and our ability to use more advanced technologies like proton therapy,” he said.
Stereotactic Radiosurgery Advances
The preferred radiation therapy technique for brain tumor cases is usually stereotactic radiosurgery (SRS) because it targets cancers with millimetric precision, largely avoiding the cognitive side effects of WBRT. It also only requires a single treatment of high-dose radiation, so the patient does not have to make multiple trips to the cancer center for treatment. “Instead of treating the whole brain with radiation, we can use Gamma Knife radiosurgery to treat each lesion we can see,” Gondi said.
Radiosurgery came into fruition in the 1960s with the advent of the Gamma Knife, a system that is still in use today. While the technology has become an integral, integrated part of radiation oncology, there are still efforts to enhance its utility. The Mayo Clinic is currently recruiting patients with five to 15 brain metastases as part of a Canadian-sponsored Phase 3 clinical trial comparing SRS to whole-brain radiotherapy. The study will assess overall survival and neurocognitive progression-free survival in an estimated 206 patients divided between two arms:
• One arm will receive 3,000 cGy of whole-brain radiation therapy plus memantine in 10 fractions;
• The other arm will receive 18-20 or 22 Gy in a single fraction of stereotactic radiosurgery.
Each group will be followed up out to 3.5 years after treatment. The trial is projected for completion in mid-2022.3
Proton Therapy for Children and Adults
Proton therapy has grown in prominence in recent years as another radiotherapy technique that spares healthy tissue. Unlike photons, which travel all the way through a target and come out the other side, protons can be programmed to stop inside the target, delivering the entire dose to a tumor.
Proton therapy particularly offers attractive benefits for pediatric cancer patients, as they are susceptible to more long-term effects of radiation. Gondi and colleagues at Northwestern presented another study at the 2018 American Society for Radiation Oncology (ASTRO) meeting comparing neurocognitive effects of proton versus photon therapy in 125 children with brain tumors. The median age at diagnosis was 7 years old, and the median time from treatment to last assessment was four years. According to Gondi, the children treated with proton therapy scored higher post-treatment in full-scale IQ, processing speed and parent-reported practical functions.4
Proton therapy also offers opportunities for treating adults with brain tumors, particularly gliomas, one of the most common types of primary brain tumors. In particular, Gondi is interested in low-grade gliomas, a slow-growing tumor that can develop earlier in life. “The average age of someone with a low-grade glioma is actually 37 — that’s the prime of these young adult lives. Their cognitive function is so important. So we’re using proton therapy to try to treat that tumor, avoid as much unnecessary radiation dose to normal brain tissue, and see if we can’t help preserve that cognitive function,” he said.
“It’s about that survivorship and how we can optimize that survivorship,” he added.
New Brachytherapy Technology Shortens Treatment Time
In February, a new brachytherapy-based technology was implanted for the first time that provides a new treatment option for recurrent brain tumors, which are traditionally difficult to treat. GammaTile — developed by GT Medical Technologies and cleared by the FDA in July 2018 — consists of a bioresorbable, conformable 3-D-collagen tile embedded with a cesium radiation source. The concept, according to GT Medical Technologies CEO Matt Likens, is to shorten the treatment period while optimizing dose distribution.
The current standard of care for brain tumors is to start with surgical resection followed by some form of external beam radiation therapy (EBRT) after the patient recovers from surgery. This can be up to six weeks, Likens told ITN, and the treatment will require daily trips to the cancer center — a taxing prospect for already-sick patients. Likens added that “half of brain tumor patients have a recurrence 12 months after resection, and the neurosurgeon is often reluctant to do another surgery because adjuvant radiotherapy won’t be possible because the patient has already had a lot of dose.”
GammaTiles are placed during the last five minutes of tumor resection surgery directly into the tumor bed. According to Likens, the radiation seeds inside the device are designed in a structural offset so only cancerous tissue is targeted. He said that this counteracts the uneven dose distribution of other brachytherapy treatments. The number of tiles implanted is customized for each procedure — Likens has seen cases use as few as three and as many as 10 — but the company is currently selling six to a pack. GammaTile was assigned its own ICD-10 code by the Centers for Medicare and Medicaid Services (CMS).
The technology was featured in a clinical study published in the Journal of Neurosurgery in January 2019. Nineteen patients with 20 recurrent tumors that had received prior radiation were treated with GammaTiles. Median follow-up showed local failure in two cases (10 percent). Median overall survival after treatment was 26 months, with nine patient deaths. Two patients required surgery for complications and two patients experienced radiation necrosis that was treated medically.5
Reducing Radiation Resistance of Gliomas
Another avenue for enhancing radiotherapy could lie in lowering the radiation resistance of cancer cells. Glioma cells are particularly known for their radiation resistance, and a recent study offers a possible blueprint for improving the effectiveness
of treatment.
Researchers at the University of Michigan studied a mutation in the isocitrate dehydrogenase 1 (IDH1) gene, found in about 50 percent of primary low-grade glioma cases. Patients with this mutation are generally younger and live longer, and it is often accompanied by two other key gene mutations, TP53 and ATRX. After implanting tumors in mice, the researchers realized the IDH1 mutation made glioma cells less aggressive. At the same time, the IDH1 mutation made the cancer cells radiation-resistant when in the presence of TP53 and ATRX.6
Ultimately, the researchers were able to extend the life of IDH1 mutation mice by combining radiation with anti-cancer drugs designed to block DNA repair. Treating with one or the other had no effect.
“These findings have the potential to impact many younger glioma patients with low-grade tumors by either ‘curing’ them or extending their lives,” said Jane Fountain, Ph.D., program director, NIH’s National Institute of Neurological Disorders and Stroke.
References:
1. Quick Brain Tumor Facts. National Brain Tumor Society. http://braintumor.org/brain-tumor-information/brain-tumor-facts/
2. Gondi V., Deshmukh S., Brown P.D., et al. Preservation of Neurocognitive Function (NCF) with Conformal Avoidance of the Hippocampus during Whole-Brain Radiotherapy (HA-WBRT) for Brain Metastases: Preliminary Results of Phase III Trial NRG Oncology CC001. International Journal of Radiation Oncology • Biology • Physics, Dec. 1, 2018. https://doi.org/10.1016/j.ijrobp.2018.08.056
3. Stereotactic Radiosurgery Compared With Whole Brain Radiotherapy (WBRT) for 5-15 Brain Metastases. ClinicalTrials.gov. https://clinicaltrials.gov/ct2/show/NCT03550391?term=NCT03550391&rank=1
4. Gross J., Powell S., Zelko F., et al. Neuropsychological Outcomes of Pediatric Brain Tumor Patients Treated with Proton (PRT) or
X-ray (XRT) Radiation Therapy. International Journal of Radiation Oncology • Biology • Physics, Nov. 1, 2018. https://doi.org/10.1016/j.ijrobp.2018.06.154
5. Brachman D.G., Youssef E., Dardis C.J., et al. Resection and permanent intracranial brachytherapy using modular, biocom patible cesium-131 implants: results in 20 recurrent, previously irradiated meningiomas. Journal of Neurosurgery, Dec. 21, 2018. https://doi.org/10.3171/2018.7.JNS18656
6. Nunez F.J., Mendez F.M., Kadiyala P., et al. IDH1-R132H acts as a tumor suppressor in glioma via epigenetic up-regulation of the DNA damage response. Science Translational Medicine, Feb. 13, 2019. DOI: 10.1126/scitranslmed.aaq1427
Related content:



 May 05, 2026
May 05, 2026