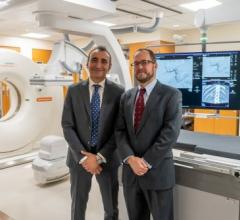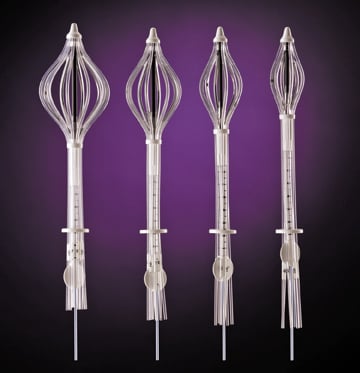
The SAVI device from Cianna Medical has a strut-based, open architecture design that allows physicians to sculpt radiation based on patient-specific anatomy.
Treatment of early stage breast cancer continues to evolve as researchers investigate more novel and efficient methods of radiotherapy. Clinical trials on accelerated partial breast irradiation (APBI) are showing that these newer methods can offer carefully selected patients several advantages over traditional whole breast irradiation (WBI).
“Whole breast irradiation is an integral part of breast conserving therapy,” said Timothy J. Whelan, M.D., MSc, radiation oncologist at Juravinski Cancer Center, Hamilton, Ontario, in a presentation at the October 2012 annual meeting of the American Society for Radiation Oncology (ASTRO). “Despite these benefits, however, it’s estimated that up to 30 percent of women do not receive whole breast irradiation, in part due to the inconvenience of therapy. As a result, investigators have evaluated alternative approaches to whole breast irradiation, including accelerated partial breast irradiation.”
As clinical trials and studies report various outcomes on the recent advances of APBI, controversy remains on whether the radiation therapy alternative really is more advantageous for early stage breast cancer patients when it comes to their long-term recovery.
Types of APBI
In contrast to WBI, APBI localizes radiation therapy to the area immediately surrounding the lumpectomy site, as this is the part of the breast where most cancers are likely to recur. By focusing treatment only on selected regions, vital organs such as the heart and lungs can be spared a significant amount of radiation. The smaller targeted volumes also allow treatment to be delivered in a shorter period of time, typically one to five days. This allows patients to return to a normal everyday life after breast conserving surgery sooner than with a longer course of therapy or with WBI alone.
Despite the documented benefits of APBI, Whelan said it remains labor and resource intensive for many physicians. Within APBI itself there are different forms and techniques. Early APBI involved the insertion of multiple catheters into the breast using a technique called interstitial brachytherapy. Newer, less invasive forms use single entry, multi-channel catheters, also known as strut-based catheters, to deliver radiation more precisely to target sites.
An ongoing clinical trial at Stanford University Medical Center[1], led by Frederick M. Dirbas, M.D., assistant professor of surgery, and Donald Goffinet, M.D., professor of radiation oncology, is studying three of the latest approaches to APBI to treat patients with invasive ductal carcinoma or ductal carcinoma in situ. Intraoperative radiotherapy delivers radiation during the initial surgery, eliminating the need for a follow-up procedure in order to perform the therapy. Intracavitary brachytherapy uses a single balloon catheter that is inserted into the cavity left behind in the breast after a lumpectomy. The catheter then releases radiation to nearby tissue; the MammoSite multi-lumen applicator from Hologic is one type of device that delivers radiation in this manner. Lastly, the trial is looking at 3-D conformal radiation therapy (3D-CRT), which, unlike brachytherapy, involves external beams of radiation that are carefully sculpted to target volumes on the breast. Computed tomography (CT) is used in the planning process to devise the APBI treatments. Overall, these different techniques of APBI can be used to treat a variety of breast cancer patients who may not be suitable for other forms of brachytherapy.
Ongoing Discussions
APBI is not without its critics. While meant to provide a less invasive form of radiation treatment without compromising survival, questions have been raised about rates of recurrence and other important factors.
Researchers at the University of Texas MD Anderson Cancer Center studied one form of APBI, breast brachytherapy, in a report that was published in May 2012 in the Journal of the American Medical Association (JAMA). The study involved a retrospective analysis of billing claims data for Medicare patients in the United States from 2003 to 2007, and compared the outcomes of one type of breast brachytherapy to those of traditional radiation therapy.
The researchers reportedly found that women who underwent APBI brachytherapy were at a higher risk of later mastectomy, radiation-related toxicities and post-operative complications. “We found that women treated with accelerated partial breast irradiation therapy have a two-fold increased risk for subsequent mastectomy, most likely because of tumor recurrence or local complications,” said the study’s senior author Benjamin Smith, M.D., assistant professor, department of radiation oncology, MD Anderson Cancer Center, in a press release. Smith noted at the time of publication that while APBI offers a shorter, and therefore more convenient, course of treatment in comparison to WBI, there remains a risk of side effects that may not be associated with more traditional therapy.
The study drew criticism from medical societies and other physicians for its potential to discourage eligible patients from pursuing APBI brachytherapy as a possible course of treatment for early stage breast cancer. It should be noted that the MD Anderson study only looked at patients treated with an early form of the technique (the analysis begins in 2003, soon after the 2002 approval from the U.S. Food and Drug Administration [FDA] for the first commercially available single-entry, single-channel balloon catheter), and therefore it would not include any data pertaining to more recent technological advances of APBI.
Another form of APBI, 3D-CRT, also was recently studied by researchers looking to compare its benefits against those of traditional radiation therapy. At the ASTRO 2012 meeting, investigators presented interim toxicity results from the Randomized Trial of Accelerated Partial Breast Irradiation (RAPID) trial, a multicenter, randomized comparison study of traditional WBI and APBI with 3D-CRT. APBI using 3D-CRT is considered a more attractive option for physicians and their patients due to its noninvasive nature and associated lower costs, according to the trial’s investigators, led by Whelan.
“The objective of our trial was to determine if accelerated partial breast irradiation using the 3-D conformal therapy was as effective as whole breast irradiation after breast conserving surgery,” he said at ASTRO.
The trial enrolled 2,135 patients, recruited between February 2006 and July 2011 from 33 centers in Canada, Australia and New Zealand, into two groups: 1,065 patients received WBI treatments, and 1,070 were selected for APBI with 3D-CRT. While investigators noted a recurrence of cancer in the breast, interim analysis was performed for adverse cosmetic outcomes (or cosmesis) only, said Whelan. “This is how the breast looks in comparison to the untreated breast after surgery and radiation,” he said. “Nurses were asked to compare both breasts and grade the shape, location of the nipple and other factors, and then provide a global cosmetic outcome.”
Cosmesis was defined as those graded fair or poor. At baseline — meaning after surgery but before treatment — nurses reported similar rates of cosmesis for both WBI and APBI treatment arms. However, at three years, nurses reported a higher rate of adverse cosmesis for the APBI group than for the WBI group. In addition to the trained nurses, patients themselves were asked to assess their own cosmetic outcomes. A panel of radiation oncologists also assessed cosmesis by reviewing the cases with unlabeled photographs. As a result, the RAPID trial’s investigators reported that patients who underwent APBI 3D-CRT after breast conserving surgery generally had worse cosmetic outcomes than those who underwent WBI. Whelan concluded that this supports earlier research indicating APBI can increase the risk of moderate side effects from radiation, and more study is needed.
What remains constant in the debate over APBI is that, when properly selected patients are treated with the appropriate technique, it can be wielded as an effective tool against many early stage breast cancers. Instead of a prolonged course of whole breast treatment, it allows women to return to a normal schedule almost immediately can be made possible by targeting radiation to affected volumes on the breast.
Reference
1. www.apbitrial.org, accessed March 5, 2013.



 May 19, 2026
May 19, 2026