May 19, 2020 —
iCAD, Inc. announced positive new clinical data supporting the Xoft Axxent Electronic Brachytherapy (eBx) System for the treatment of glioblastoma multiforme (GBM) will be presented at the American Society of Clinical Oncology (ASCO) 2020 Virtual Scientific Program, which will take place May 29-31, 2020.
“This represents a significant milestone for the company, as it further validates Xoft intraoperative radiation therapy (IORT) in certain types of brain tumors and demonstrates the impact that this unique technology offers,” according to Michael Klein, Chairman and CEO of iCAD. “GBM is the most common and aggressive type of malignant primary brain tumor, with a median survival of 10-12 months.1,2 With almost 297,000 cases of brain and nervous system tumors diagnosed worldwide per year,3 this exciting new application for the Xoft System could substantially expand our addressable market, but more importantly, it has the potential to extend patients’ lives.”
The study, titled “Intra-operative radiation therapy as salvage treatment option for recurrent glioblastoma multiforme,” (abstract #291893) was submitted to ASCO by Nidal Salim, M.D., radiation oncologist and head of the radiotherapy center at the European Medical Center (EMC) in Moscow, one of the largest private medical clinics in Russia and an international leader in comprehensive care and oncology. It involved 30 patients with recurrent GBM who were treated between August 2016 and June 2019. All patients underwent maximal safe resection; 15 patients were treated with IORT without adjunctive chemotherapy, while the other 15 were treated with external beam radiation therapy (EBRT) and temozolomide. According to study findings, as of December 2019, median overall survival (OS) was 27 months in the IORT group, versus 21 months in the EBRT group. The local progression free survival (locPFS) range for the IORT group was between 3.5 to 39 months, versus 2 to 10 months in the EBRT group. As of December 2019, 8 patients from the IORT group were still alive, whereas none of the patients in the EBRT group survived. Kaplan-Meier OS curves in patients with post-operative contrast-enhancing volume (POCEV) of ≤ 2.5cm3 showed more favorable outcomes for patients in the IORT group (p < 0.05). Researchers concluded that IORT of recurrent GBM is feasible and provides encouraging local progression-free and overall survival, with a manageable toxicity profile.
Positive preliminary clinical data from this study was presented in September 2019 by Alexey Gaytan, M.D., Ph.D., neurosurgeon at the EMC at the European Association of Neurosurgical Societies (EANS) Congress in Dublin, Ireland.
“After researching this modality for nearly four years, we are greatly encouraged by these clinical results and the benefits this treatment offers to patients. For the treatment of GBM, IORT with the Xoft System is a promising treatment option that may offer better outcomes for patients, with minimal side effects, compared to traditional radiation therapy,” according to the study’s lead researcher, Alexey Krivoshapkin, M.D., Ph.D. and neurosurgeon at the EMC. “This treatment option not only has the potential to increase overall survival, it may also enhance patients’ quality of life by allowing them to forego weeks of daily radiation fractions and instead spend that time with their families and loved ones.”
Prof. Krivoshapkin will discuss these findings in a European Society for Radiotherapy (ESTRO) Virtual Satellite Symposium hosted by Xoft, titled “Intraoperative Radiation Therapy (IORT) for Brain Cancer: Local Tumor Control in Patients with Recurrent Glioblastoma,” on Thursday, May 14, at 8 am ET and Tuesday, May 19, at 12 pm ET. Registration is available for these events via this link: https://www.icadmed.com/educational-webinars.html.
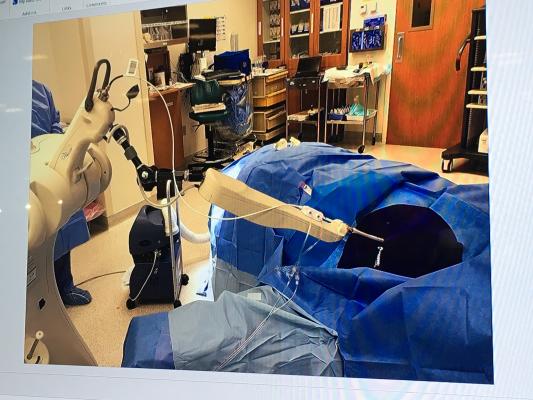
This research adds to the growing body of evidence that continues to support the Xoft System across multiple cancer types, including early-stage breast cancer, gynecological cancers, nonmelanoma skin cancers and recently, brain tumors. The Xoft System uses a miniaturized x-ray source to deliver a precise, concentrated dose of radiation directly to the tumor site, while minimizing risk of damage to healthy tissue in nearby areas of the body. Xoft brain IORT allows radiation oncologists and surgeons to work together to deliver a full course of radiation treatment in one day, at the time of surgery, while the patient remains under anesthesia. Once the tumor has been surgically removed, the Xoft System’s miniature x-ray source is inserted inside a flexible balloon-shaped applicator, which is then placed inside the tumor cavity, filled with saline, and used to deliver a single dose of radiation directly to the tumor bed. For the treatment of certain types of brain tumors, IORT with the Xoft System may allow appropriately selected patients to potentially replace weeks of post-operative external beam radiation therapy (EBRT) with a single fraction of radiation.
“This research is particularly relevant as COVID-19 continues to be a major global health concern, as it is in line with recent clinical guidelines issued by several national medical societies that recommend an abbreviated course of radiation, when appropriate,4,5” noted Klein. “IORT with the Xoft System offers a transformative solution that may help to alleviate the burden placed on many hospitals and healthcare facilities during the COVID-19 de-escalation phase. The ability to treat patients with a full course of radiation in just one day may not only free up space in hospitals and allow clinicians to focus on other critical needs, it may reduce immunocompromised patients’ time in hospitals and minimize their potential exposure to the virus.”
This research builds upon a retrospective analysis published last year in World Neurosurgery by Prof. Krivoshapkin, et al., which examined the repeat resection and the various methods of IORT for the treatment of malignant brain gliomas (MBGs), including high-energy linear accelerators and modern, integrated brachytherapy solutions using solid and balloon applicators.6 The conclusions of this review identified IORT with balloon applicators to be particularly promising.
iCAD also recently announced the first metastatic brain tumor was treated in the U.S. with IORT using the Xoft System at the James Graham Brown Cancer Center at the University of Louisville. The procedure marked the start of a clinical trial on IORT for patients with large brain metastases treated with neurological resection with the Xoft System, led by Shiao Yuo Woo, MD, FACR, radiation oncologist, James Graham Brown Cancer Center at the University of Louisville.7
“Our technology is world-class, and we remain steadfast in our mission to unlock its full potential as we explore the clinical development of FDA-cleared, CE marked Xoft technology across an ever-expanding array of various types of tumors,” Klein added.
References:
1. Tamimi AF, Juweid M. Epidemiology and Outcome of Glioblastoma. In: De Vleeschouwer S, editor. Glioblastoma [Internet]. Brisbane (AU): Codon Publications; 2017 Sep 27. Chapter 8. Accessed via https://www.ncbi.nlm.nih.gov/books/NBK470003.
2. Pan E, Prados MD. Glioblastoma Multiforme and Anaplastic Astrocytoma. In: Kufe DW, Pollock RE, Weichselbaum RR, et al., editors. Holland-Frei Cancer Medicine. 6th edition. Hamilton (ON): BC Decker; 2003. Accessed via https://www.ncbi.nlm.nih.gov/books/NBK12526/.
3. WHO, IARC, Globocan Cancer Incidence and Mortality Worldwide in 2018. Accessed via https://gco.iarc.fr/today/data/factsheets/populations/900-world-fact-sh….
4. American Society for Radiation Oncology (ASTRO) COVID-19 Recommendations to Radiation Oncology Practices. (2020). Accessed via https://www.astro.org/Daily-Practice/COVID-19-Recommendations-and-Infor….
5. The American Society of Breast Surgeons (ASBrS), the National Accreditation Program for Breast Centers (NAPBC), the National Comprehensive Cancer Network (NCCN), the Commission on Cancer (CoC) of the American College of Surgeons, and the American College of Radiology® (ACR®) joint recommendations. Recommendations for Prioritization, Treatment and Triage of Breast Cancer Patients During the COVID-19 Pandemic. (2020). Accessed via https://www.facs.org/-/media/files/quality-programs/napbc/asbrs_napbc_coc_nccn_acr_bc_covid_consortium_recommendations.ashx.
6. Krivoshapkin A, et al. Repeat Resection and Intraoperative Radiotherapy for Malignant Gliomas of the Brain: A History and Review of Current Techniques. World Neurosurgery (2019) 132: 356-362. Accessed via https://doi.org/10.1016/j.wneu.2019.09.037.
7. University of Louisville. Study of Intraoperative Radiotherapy for Patients With Large Brain Metastases Treated With Neurosurgical Resection. Accessed via https://clinicaltrials.gov/ct2/show/NCT04040400. ClinicalTrials.gov Identifier: NCT04040400.
8. Conant, E et al. (2019). Improving Accuracy and Efficiency with Concurrent Use of Artificial Intelligence for Digital Breast Tomosynthesis. Radiology: Artificial Intelligence. 1 (4). Accessed via https://pubs.rsna.org/doi/10.1148/ryai.2019180096.
For more information: www.icadmed.com


 May 06, 2026
May 06, 2026 









