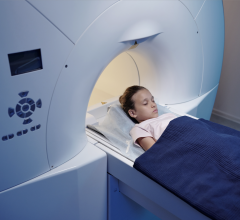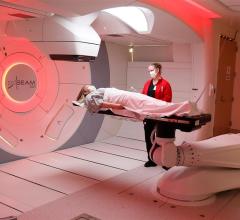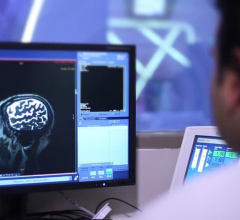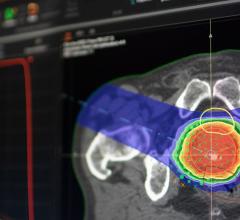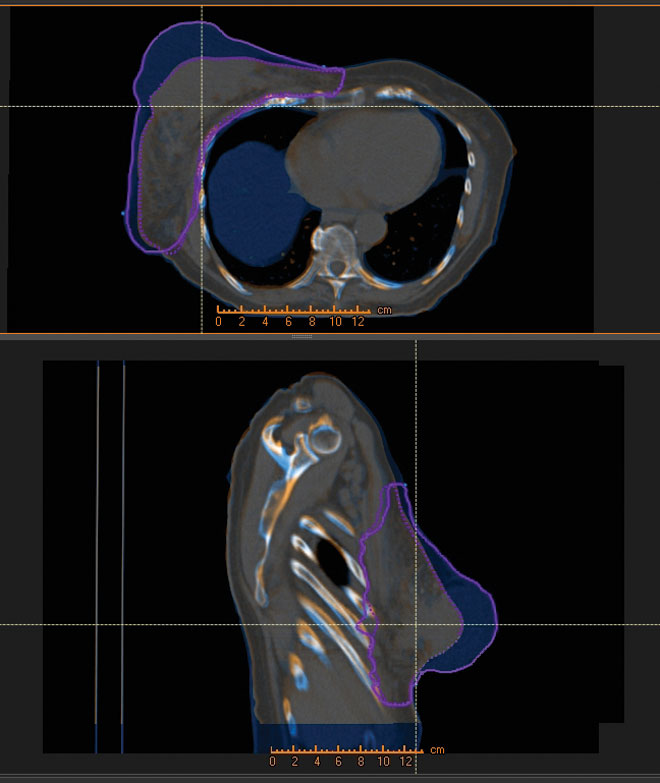
Figure 1: Original treatment plan
Proton therapy is an exciting modality in radiation oncology. It is the target of both positive and negative perspectives - the positive related to the technology itself and the ability of proton beams to deposit energy mostly within the tumor being treated. The negative opinions generally result from the historically high cost to build and maintain a center and the lack of access for patients worldwide. The Provision Center for Proton Therapy has not only embraced proton therapy, but also the concept that it must be used in conjunction with other advanced technologies that will assure treatment accuracy.
Because proton beams are so controllable, it is important to recognize that a treatment can accurately miss a cancerous tumor if the treatment is not planned and monitored carefully. In the case of conventional photon treatment courses, dosimetric errors are not as likely to occur, and corrections are relatively easy to make. With protons, minor variations in patient shape and density, along with positioning error, can result in very significant differences in delivering the planned dose.
To this end the center has very successfully implemented two key technologies with its treatment planning system - robust optimization and adaptive therapy. RayStation from RaySearch Laboratories allows staff to create very advanced plans quickly and efficiently.
Adaptive Planning
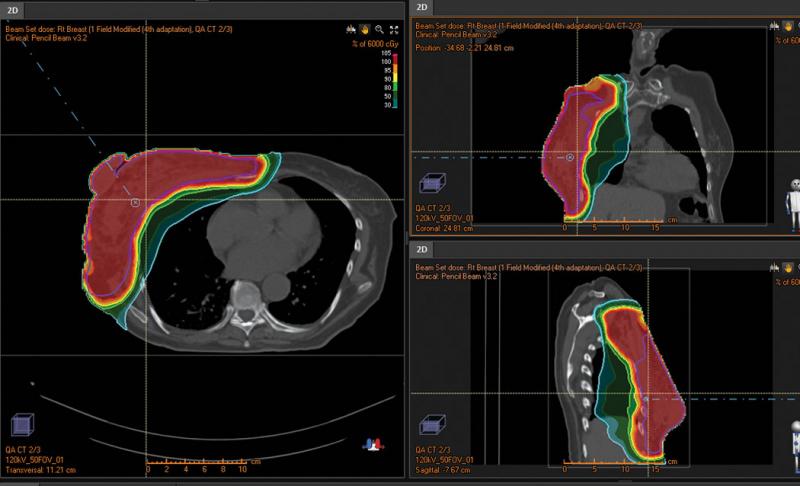
The first example demonstrates how important it can be to modify plans based on changes during treatment. A woman presented with a right breast cancer that was very large and invasive. It was expected that the patient would have a fast response so weekly QA CTs were performed during treatment. Deformable registration was used to determine if the existing plan had adequate coverage. Soon after the treatment commenced, the scans showed significant changes that warranted replanning. The center used the adaptive planning function in RayStation to quickly replan the case and get back to the prescribed dose. The adaptive planning function does not require that the user re-enter the beam parameters or the inverse planning objectives. In total four adapted plans were implemented over the course of treatment with only a day or so needed each time to complete the planning and quality assurance. The sum of the doses was easily displayed so that an overall analysis could be made on the efficacy of the delivery. Adaptive planning in a case like this is simply unavoidable - in the case of protons that are sensitive to density and anatomical changes in the body, it would be impossible to plan this in an efficient and/or safe manner without advanced technologies such as deformable registration and adaptive therapy.
Robust Optimization
Protons are very sensitive to changes in density and patient shape.
Therefore, variations in patient positioning can have dramatic effects on the dose distribution. The use of planning target volumes (PTVs) to account for these variations is not always sufficient to achieve a robust plan. To enable the creation of robust plans for cases, where conventional margins do not work, RayStation implements, instead, robust optimization, which explicitly takes these variations into account and aims for a plan that is as good as possible with respect to the worst case variation.
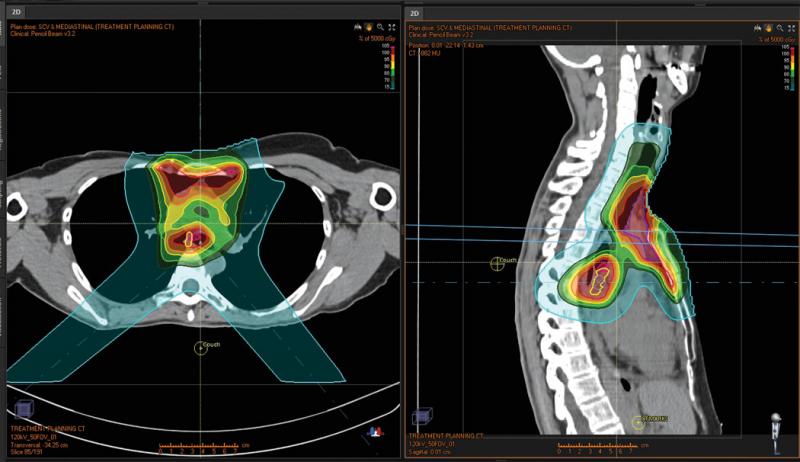
The patient in a second clinical case (Figures 3 and 4) had a clinical target volume (CTV) that was anterior on the sternum but also a CTV in the mediastinum behind the great vessels. A plan was designed to treat the anterior CTV with an AP beam and the posterior CTV with posterior obliques. However, the lung interface and the fact that the CTVs overlapped superior/inferior presented a challenge. Instead of treating single field uniform dose (SFUD) and irradiating more lung and heart tissue, robust optimization was utilized. This allowed the team to account for range uncertainty in a very heterogeneous area, and ensure that with setup error and range uncertainty there would be no unacceptable hot or cold spots. Uniform dose was achieved in a robust manner, even where the CTVs overlapped. Robust optimization further eliminated the need for beam specific PTVs and a complicated optimization process.
Proton therapy requires a very high level of focus and treatment planning technology. Intensity modulated proton therapy (IMPT) in RayStation allows for quick, efficient, robust and adaptive planning for effective proton treatments.
Case study supplied by RaySearch Laboratories.



 May 06, 2024
May 06, 2024