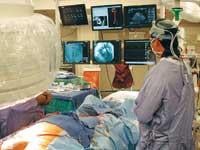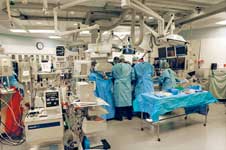
The barriers that once separated interven-tionalists, cardiac surgeons, vascular surgeons and electrophysiologists are rapidly being reduced by the convergence of transcatheter technologies and the need for high-quality fluoroscopic imaging systems. All these specialists are now using cath lab technology and finding that combining these labs with the assets of an operating room (OR) brings together the best of both worlds.
However, planning for hybrid suites involves much more partnering and multiple departmental involvement than planning for an OR or cath lab alone. These rooms are used not only by surgeons and interventional cardiologists, but also by electrophysiologists, neurosurgeons, structural heart specialists and vascular surgeons.
“It really takes a village when planning a hybrid suite,” said David L. Brown, M.D., FACC, FACP, co-founder of The Heart Hospital Baylor Plano, Texas.
He serves there as president and chairman of the medical staff, director of interventional cardiology and co-director of cardiovascular research and the structural heart program. Brown also started a consulting business to help hospitals in their planning for hybrid suites. He explained how to plan for a hybrid during a presentation at the Philips Healthcare and American College of Cardiology (ACC) hybrid exhibit at the ACC meeting in March.
Group Planning is Key
Before approaching the hospital administration about the need for a hybrid suite, consensus needs to be built among all the potential users. A site visit should be made to a hospital that already has one of these suites. Brown suggests including the hospital administrator, OR management and the architect during the visit.
The key people who should serve on hybrid suite planning committees include the surgeons and cardiologists who will use the facility, the OR and cath lab staffs, OR nurses, information technology staff, the OR and cath lab directors, the facilities manager, infection control personnel and the architect.
Brown said it’s also a good idea to include the OR and cath lab equipment vendors chosen for the project so they can coordinate. All four of the big angiography system manufacturers already have partnerships with key OR equipment vendors for smoother hybrid planning and installation. Weekly planning meetings can help keep everyone informed of changes in the plans or design. This enables everyone to have a chance to speak up prior to any final decisions.
Utilization of the Hybrid Lab
“We are no longer cutting things out of people,” Brown said. He explained the future of surgery is going to be minimally invasive, using cath lab techniques instead of traditional, open surgical methods. This includes ablation instead of excision, image-guided over visual navigation, reconstruction without suturing and access via natural orifice or blood vessel instead of incision. This trend is evident with the widespread adoption of endovascular repair of aortic aneurisms, the spread of transcatheter heart valve and shunt occluders, and percutaneous interventions instead of traditional vascular surgery. Brown said hybrid suites are ideally suited for aortic arch repair, implantation of percutaneous left ventricular assist devices (LVADs), transcatheter heart valve replacements, peripheral vascular procedures, thoracic and abdominal aortic endografting, electrophysiology (EP) procedures and combo coronary artery bypass graft (CABG)/percutaneous coronary interventions (PCI). He said completion angiography of a CABG helps detect defects before closing the patient, but high-quality imaging systems are needed.
Location of the Hybrid Suite
“I think all this is better served by a hybrid suite located in the OR,” Brown said. “It is easier to bring the OR into range for imaging than it is to convert a cath lab into an OR.”
He said ORs need positive ventilation, access to a scrub room, sterilization equipment and surgical equipment and supplies. All of these are already located in the surgical department. Cath labs can be converted into a hybrid, but the cost to bring these rooms up to surgical standards is often high. Brown also said it is often less expensive to share existing OR resources, than to duplicate scrub rooms, supplies and equipment in another area of the hospital.
“It is a new workplace,” Brown said. “It’s not making a cath lab into an OR, nor is it making an OR into a cath lab.”
Dual-Use Room
When one of these suites is not being used for a hybrid procedure, it can be used as a normal OR, cath lab or EP lab. “We use our hybrid room for cardiac (surgical) cases when it’s not being used for hybrid cases,” Brown said. Vascular surgeons also use the room for endovascular cases. He said many prefer the OR area to a cath lab because they feel more comfortable in their own environment. Also, if a patient suffers a major complication requiring surgery, they would already be in an OR.
The Imaging System
High-quality imaging is key to all hybrid suite procedures. Cath labs utilize top-of-the-line fluoroscopic X-ray angiography systems. New technology is also making these systems more useful, such as stent enhancement modes, integration with 3-D ultrasound, intravascular ultrasound (IVUS), intracardiac echo (ICE), trans-esophageal echo (TEE) and 3-D rotational angiography. To improve navigation within the heart, especially for more complex structural transcatheter procedures, hybrid imaging systems will become commonplace in the future, Brown said.
As an example, he said Philips is developing the Heart Navigator System, which uses preloaded computed tomography angiography (CTA) data sets. The images can be manipulated to show multiple views of the same anatomy, such as an aortic valve, for easier procedure planning. These images can be overlaid on live fluoroscopy to support navigation. The image can be edited to show only the 3-D anatomy of interest.
Brown suggests imaging systems that are compact and easy to move out of the way are the best for a hybrid lab. For this reason he prefers monoplane systems, because they take up less space. Brown also said ceiling-mounted gantry systems are easier to move out of the way and do not impede floor space. Give consideration to the size of the digital X-ray flat panel. Standard cardiac imaging uses a 12-inch panel, but vascular work usually requires a 16-inch panel. Systems should include digital subtraction software, an analysis package for hemodynamic measurements and picture archiving and communication systems (PACS) compatibility.
When purchasing the imaging system, Brown said it’s best to prepare a request for proposal (RFP) and solicit bids from several vendors. “We found RFPs to be a very useful aid that allows for an apples-to-apples comparison,” Brown said. He said the key vendors include GE Healthcare, Siemens, Philips and Toshiba. Also, request site visits from each vendor so they can see firsthand what a facility’s needs are.
Specialized Equipment
Other imaging equipment not frequently used in the cath lab, but important to surgeons and neurologists, includes video endoscopy devices and transcranial Doppler. Cardiac surgeons also require a heart-lung machine and anesthesia. Specialized software systems required in a hybrid include hemodynamic monitoring, access to PACS and reporting systems for the various specialties using the suite.
Endovascular Repair
A key use of hybrid suites is for endovascular abdominal aortic aneurism (AAA) and thoracic aortic aneurism (TAA) repair.
“As we move from AAA to thoracic aortic arch repairs, there are fewer open procedures now,” Brown said. “We almost never see an open abdominal or thoracic procedure anymore. Everything is done endovascularly now.”
Preprocedure planning for these implants is crucial, because proper sizing is needed to prevent complications. Periprocedural navigation aids are also important to prevent the occlusion of side branch vessels. For these reasons, Brown said advanced visualization software plays a key role in the hybrid suite. The software takes CT or magnetic resonance imaging (MRI) data sets to create accurate 3-D images of the anatomy prior to the procedure.
EP in the Hybrid
Brown said combo EP/cath/ORs are going to be the next big trend in hybrid suites. These suites are ideally suited for the minimally invasive surgical procedures required to implant pacemakers, implantable cardioverter defibrillators (ICDs), cardiac rhythm therapy devices (CRTs) and implantable cardiac monitors. If EP will play a role in a hybrid suite, EP navigation systems are needed for complex procedures, such as catheter ablations.