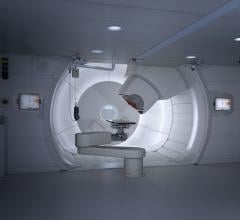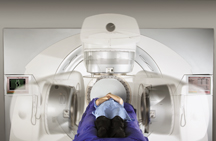
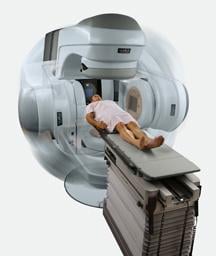
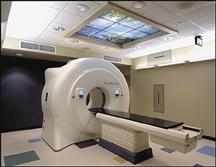
Elekta volumetric modulated arc therapy (VMAT) is a new intensity-modulated radiation therapy (IMRT) treatment technique.
While faster treatment delivery times are driving many radiation oncology clinicians to adopt volumetric modulated arc therapy (VMAT) as their technique of choice, others are holding steadfast to traditional intensity modulated radiation therapy (IMRT) systems.
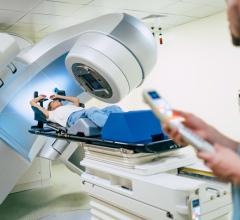
Over the last few years, two companies, Varian Medical Systems and Elekta, have each introduced tools that employ VMAT — RapidArc and Elekta VMAT, respectively. The VMAT technique has cut radiation delivery times significantly, from 10-15 minutes on traditional IMRT down to two minutes or less using VMAT treatment. With traditional IMRT, a complex sequence of fixed beams from multiple angles delivers the radiation. Whereas with the VMAT, it delivers the dose with a single arc during a single rotation of the linear accelerator. Simultaneously, all treatment parameters are modulated, including gantry position, gantry speed, multileaf collimator (MLC) leaves, backup-diaphragms, dose rate and collimator angle. What this reduction in time means for the clinician who uses VMAT is shorter patient visits, increased patient throughput and improved patient comfort.
Elekta VMAT uses the ERGO ++ treatment planning system, which includes the Arc Modulation Optimization Algorithm for creating VMAT plans. It also has the capability to deliver the dose in multiple arcs while the gantry makes two or more rotations or partial rotations, which are more applicable to structures like the head and neck.
Other advantages VMAT offers compared to traditional IMRT techniques include step-and-shoot and sliding window (dynamic) IMRT. For step-and-shoot, current IMRT treatments vary the monitor unit (MU) per degree by stopping gantry rotation during treatment delivery, which lengthens treatment time. Additionally, IMRT plans consist of several fields, or control points. VMAT has an unlimited number of fields. With sliding window (dynamic) IMRT, the gantry remains stationary at fixed angles. While this can provide minimal decreases in treatment time, this technique may be considered a less efficient use of MUs because the radiation beam remains on as dose is delivered through tiny field shapes. VMAT varies MLC leaves, gantry position and speed, and dose rate while the beam is on, creating greater dose conformance and faster treatment times, while using lower total MUs.
“The speed is quite significant,” said Vivek Mehta, M.D., radiation oncologist, Swedish Cancer Institute who uses Elekta VMAT in his practice. “The patients are appreciative because they spend less time on the hard table and/or immobilized by a mask. The staff is appreciative of the fact that they are more likely to stay on time and complete their overall day without having to treat after hours.
RapidArc is an IMRT system that also employs VMAT technology, enabling it to target radiation beams at a tumor, while making a single continuous rotation. Ghiren Shah, M.D., medical director, Cancer Care of Western New York, who uses the RapidArc system, noted, “It really has improved the efficiency in our clinic, improved workflow and improved patient comfort because instead of having to lie still there for 10-15 minutes, which is difficult to do when you’re in a room alone, it allows them to be on the table for one and a half minutes with our treatment. And it has greatly improved patient comfort. If we’ve cut out 10 minutes per patient - you can imagine that at a busy clinic - if we’ve treated 50 patients, that is 500 minutes a day or 8 hours.”
The faster delivery time also means less radiation or ‘beam-on’ time for the patient, resulting in improved treatment and less motion artifact since the patient has to remain still for a much shorter amount of time. According to Dr. Shah, “Dose volume histograms have shown significant improvement in rectal doses for prostate cancer.” Even though he explained that on paper side effects show the potential to improve with VMAT, he believes that it is still too early to determine if there will be a clinical benefit in terms of a reduction in side effects. Because the machine is simultaneously controlling all parameters of treatment, he believes that VMAT is the most conformal dose distribution that can be created of any form of radiation available today.
While VMAT offers faster treatment times, which directly affects patient comfort and throughput, many clinicians prefer TomoTherapy’s Hi-Art system for treating their patients, despite somewhat longer treatment times and a higher price tag for the equipment.
Robert Miller, M.S., medical physicist, Meridian Park Radiation Oncology Center, and Normal Willis, M.D., medical director, Meridian Park Radiation Oncology Center, chose TomoTherapy’s Hi-Art system because of its universal application for many anatomical locations — including more complex areas like the spine — and for its ease in conducting IGRT along with IMRT. TomoTherapy combines integrated CT imaging with conformal radiation therapy to deliver sophisticated radiation treatments with speed and precision, while reducing radiation exposure to surrounding healthy tissue.
“From a physicist’s perspective, TomoTherapy is a form of VMAT,” indicated Miller. “It is volumetric therapy, but it is doing it with multiple helical arcs that overlap and we can actually control that overlap. Whereas VMAT and RapidArc are maybe one, maybe two, maybe three arcs total. [TomoTherapy] is doing that but it is doing it many, many, many times. The treatment times can be significantly longer and the treatment times we’re talking about are 10 minutes versus maybe a 2 minute time on RapidArc or VMAT.”
According to Dr. Willis and Miller, the longer treatment time is a result of the radiation beam being on longer in order to achieve a greater degree of definition and accuracy and to keep doses to surrounding tissues low. “As a physician, the main advantage to TomoTherapy is that you target the volume that you are trying to get your dose into through many different angles, while the machine goes around in these concentric, overlapping helical arrangements. Any one area of normal tissue gets very little radiation so we are able to keep the toxicity down really low in a lot of situations where we used to get a lot of toxicities,” said Dr. Miller.
TomoTherapy is working to cut treatment times by applying the concept of accelerated hypofractionation to overcome tumor repopulation for non-small cell lung cancer, incorporating the technique into its conformal dose-delivering platform with helical IMRT and IGRT. Preliminary evidence demonstrated that this type of treatment schedule can safely be achieved along with better tumor control and possible survival improvement.
While it is clear that VMAT techniques and TomoTherapy differ in radiation delivery speed, what is yet not clear is which treatment is more efficacious. That determination is left in the hands of each radiation oncologist.
One success story with TomoTherapy at their clinic involved a patient who had a recurrence of endometrial cancer in one of her retroperitoneal lymph nodes following multiple treatment regimens and after being referred to three other radiation oncologists who viewed her condition as untreatable.
Dr. Miller explained, “With Tomotherapy, we were able to outline the retroperitoneal lymph nodes that were abnormal on her CT scan and PET scan and to treat them with a great deal of accuracy and limit the dose to the normal adjacent small and large bowel to the point that she had absolutely no side effects during treatment and she continued to work full-time. She is now approaching two years with no signs of cancer.”
For these two radiation oncology professionals, the extra 8-13 minutes are worth the time given the quality of treatment that they are able to offer with TomoTherapy. Dr. Willis stated, “We could get treatment times the same as VMAT by basically degrading the modulation points, the detail of what we do—something comparable to VMAT to reach comparable treatment speeds. But instead we chose to use the full advantage of helical tomotherapy, which is a more intricate, more involved way of treating.” Miller echoed this sentiment, “I can give you a 2-minute treatment on a plan, but it won’t be anything approachable to what TomoTherapy has the potential to deliver. VMAT and RapidArc are really designed from a gantry machine to compete with TomoTherapy. They do it in a very time effective manner.” For Dr. Willis, the extra time also affords the opportunity to give the patient the type of individual attention and care that he feels is also important to the overall treatment.
In a Phase I trial, researchers escalated the biologically-effective tumor dose via hypofractionated treatment regimens using 25 fractions over five weeks instead of the traditional six to seven weeks or longer . In essence, the radiation dose is raised and delivered in less time. Preliminary evidence from a study conducted by Minesh Mehta, M.D., radiation oncologist and professor of Human Oncology at the UW School of Medicine and Public Health, demonstrated a 2-year survival rate of 46.8 percent for the 46 patients treated with this new technique compared to 21.5 percent from a database representing all clinical, surgical-pathological, and follow-up information for 5,319 patients treated for primary lung cancer. Lung and esophageal toxicities were also lower than expected in comparison to previously reported outcomes for dose-escalated studies. Overall, preliminary evidence demonstrated that this type of treatment schedule can safely be achieved along with better tumor control and possible survival improvement in a set of patients with non-small cell lung cancer compared to traditional radiotherapy techniques.

 July 09, 2024
July 09, 2024