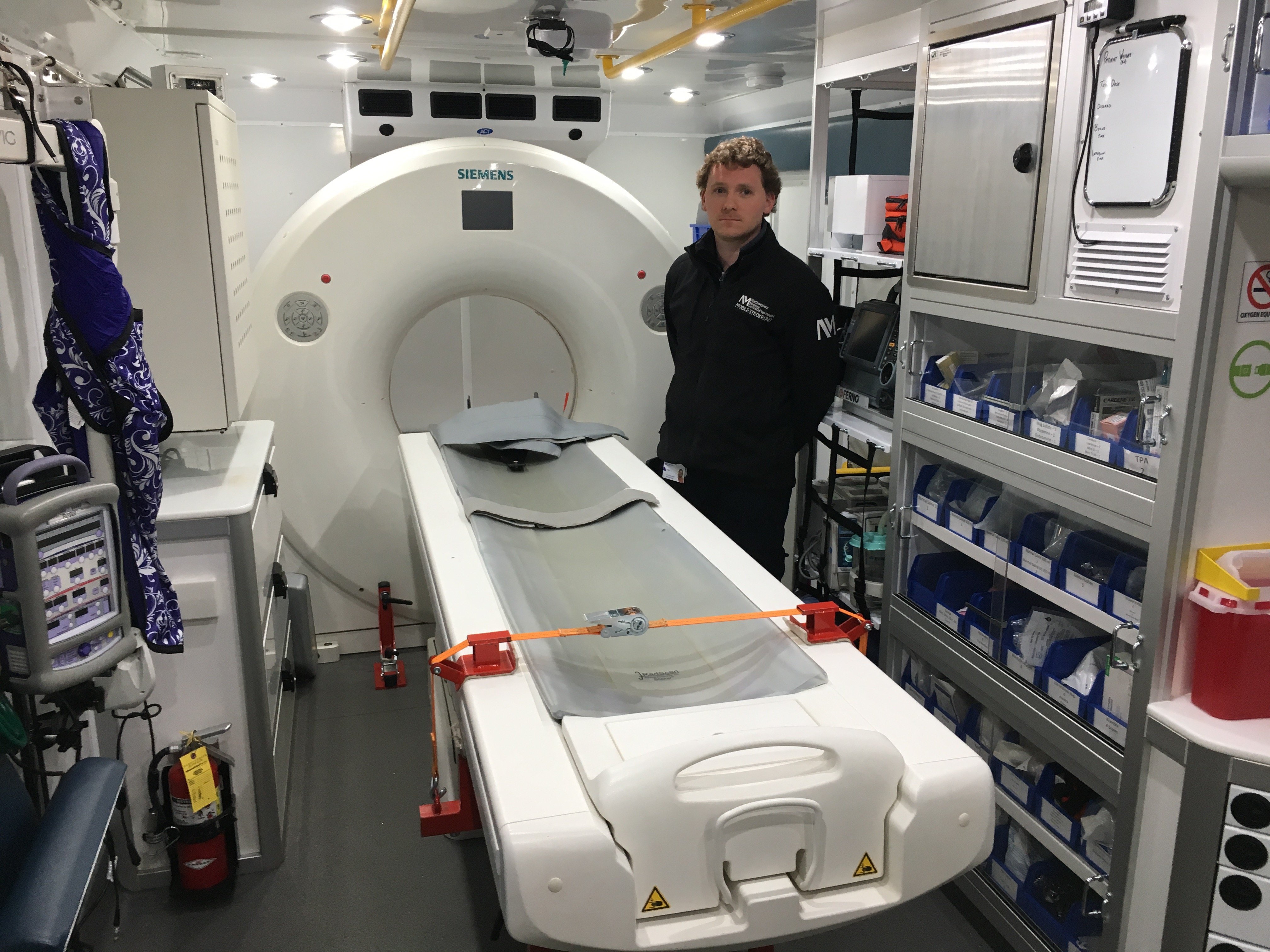
Peter Juodka, RT(CT) operates the 16-slice Siemens Somatom Scope CT scanner in the mobile stroke unit to assess stroke patients immediately at the call site.
Stroke is the fifth leading cause of death in the United States, responsible for more than 140,000 deaths in some of the most recent data.1 When treating stroke patients, perhaps more than any other condition, time is of the essence. “We know that for every 15 minutes you delay treatment, you lose three and a half years of your life,” said Harish Shownkeen, M.D., interventional neuroradiologist at Northwestern Medicine Central DuPage Hospital (CDH) in Winfield, Ill. In an effort to reduce time to treatment and improve patient outcomes, in 2017 Shownkeen and CDH, a Joint Commission-accredited Comprehensive Stroke Center, turned to an innovative solution that has slowly been making its way across the U.S. — a mobile stroke unit.
VIDEO interviews and tour of the CDH mobile stroke unit
Bringing the Hospital to the Patient
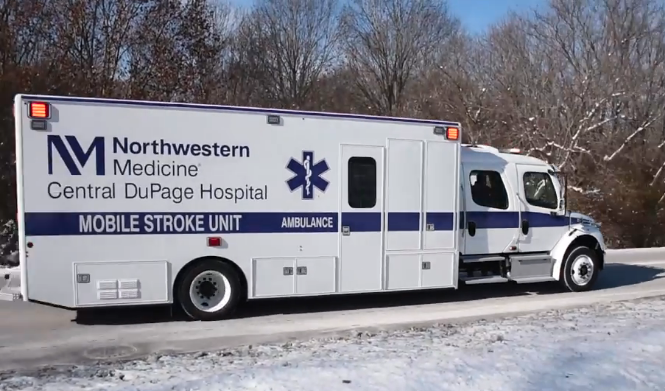
A mobile stroke unit (MSU) is essentially an ambulance with an onboard computed tomography (CT) scanner. When a patient is suspected to be having a stroke, a CT scan of the brain is the fastest way to determine what type of stroke it is — ischemic or hemorrhagic — and therefore which medication is needed. This is the most critical step in stroke care: If the stroke is ischemic (caused by a clot), tPA is required to dissolve the clot and restore blood flow; if the stroke is hemorrhagic (caused by bleeding in the brain), a reversal agent is needed to stop the bleeding. The wrong medication could prove fatal to the patient. The MSU is equipped with all of the traditional medications, tools and resources used to treat stroke patients in a hospital setting.
The Central DuPage MSU runs with four people on the ambulance at all times:
• A medic driver;
• A critical care paramedic;
• A critical care nurse; and
• A CT technologist.
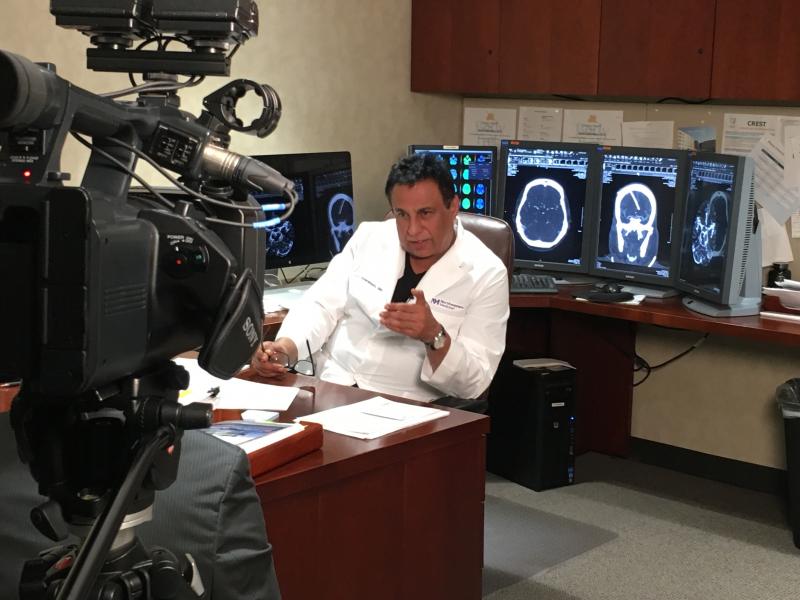
As the CT scan and other on-board tests are being performed, results are sent to a stroke neurologist and a radiologist back at the hospital via a wireless VPN router. “We’re able to live stream those physicians into the back of the ambulance where they can do an assessment of the patient,” said Mehr Mohajer-Esfahani, MSN, RN, program manager of the Mobile Stroke Unit.
None of the MSU team members work with the unit full-time — all team members are rotated in from their respective departments across the hospital.
Take a 360 degree look inside the CDH mobile stroke unit.
History of Mobile Stroke Units
The concept of the MSU originated at Saarland University in Hamburg, Germany, in 2008. A paper describing the venture, published in Plos One in 2010, noted that, “Early treatment with rt-PA is critical for favorable outcome of acute stroke. However, only a very small proportion of stroke patients receive this treatment, as most arrive at hospital too late to be eligible for rt-PA therapy.”2 The researchers found that call-to-therapy-decision times with the MSU settled around 35 minutes.
While the concept was proven in Europe, mobile stroke units did not make their way to the U.S. until 2014. Memorial-Hermann Texas Medical Center in Houston was the first domestic site to adopt the concept, and now there are an estimated 20 MSUs across the country — with Indiana University Health announcing its intention to be the 21st in late April.
CDH was the first site in Illinois (where stroke is the third leading cause of death3) to adopt an MSU. Rush University Medical Center in Chicago added their own truck later in 2017. Shownkeen was inspired to bring the MSU to Central DuPage after seeing one while visiting friends in Germany.
MSU Protocols
Since the MSU concept is still developing in the United States, every site operates their unit a little differently. According to Shownkeen, many hospitals run their mobile stroke units in a one week on/one week off pattern. This helps reduce costs and also ensures that adequate data is still being collected on conventional EMS stroke care as a basis for comparison. “We are one of the few MSUs that run seven days a week, 12 hours a day,” Shownkeen said.
At CDH, when a possible stroke call comes in inside the unit’s primary service area — a six-town radius encompassing roughly 30 square miles — the MSU is dispatched in conjunction with local emergency services; whichever team arrives first will begin assessing the patient. If it is determined they are not having a stroke, the MSU will be recalled to the hospital.
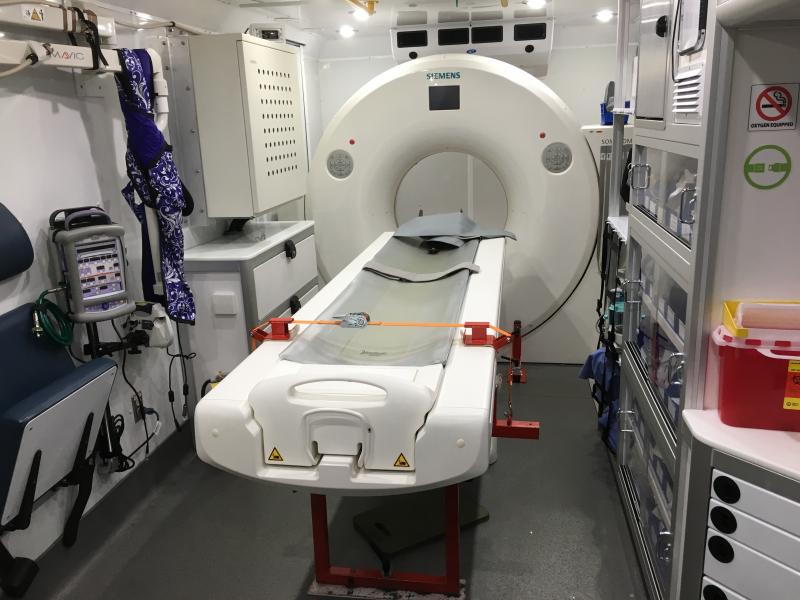
If the patient is exhibiting stroke signs and symptoms, they will be moved to the back of the ambulance for the CT scan. Many mobile stroke units feature a small portable CT system, but the CDH MSU has a full-size, 16-slice Siemens Somatom Scope scanner onboard.
“The biggest difference is when you get on scene, you don’t really know much about the patient,” said Peter Juodka, RT(CT), a CT technologist with the Mobile Stroke Unit. “You kind of gather information as you go, as opposed to the emergency department or even outpatient where you have gathered history through events pre-hospital and in the emergency department.”
While the circumstances are very different from a technologist’s day-to-day experience, radiation safety is still a top priority. The technologist and the patient are the only people in the ambulance during the scan (unless additional assistance is needed), and the truck features a lead-lined booth from which the scanner is operated. For extra protection, the technologist wears a lead apron to cover their backside and a dosimeter to monitor radiation levels. “So the protection is there but you’re considerably closer to the scanner than you would be in a normal radiology suite,” Juodka said.
For the radiologist back in the hospital, the experience is similar to Juodka’s — akin to daily practice in many ways and completely different in others. “It’s pretty much the same workflow but things are done exponentially faster,” said Shownkeen.
MSU Training
An undertaking of this magnitude is not carried out successfully, however, without a great deal of planning and practice. Prior to go-live in January 2017, all MSU personnel underwent 12 weeks of joint training. The focus, said Mohajer-Esfahani, was two-fold: learning to work together in a heightened capacity, and doing so in the confined quarters of the ambulance. He said he was pleasantly surprised at how quickly the unit gelled in this new context.
“These guys are all a wonderful group of professionals,” he said. “They each bring a unique set of skills and characteristics that once they were able to work together, they essentially complemented each other.” Finding individuals with those complementary skills was paramount when selecting MSU personnel, Mohajer-Esfahani added. For example, all of the critical care paramedics have backgrounds in flight, specialty transport and the hospital setting. Medic drivers have a minimum of 20 years’ experience operating large vehicles. MSU critical care nurses are drawn from the Neuro Intensive Care Unit.
Mohajer-Esfahani noted that while such individual levels of experience are important, none of the MSU’s success would have been possible without the help of local EMS. “A lot of us, our backgrounds are in the hospital,” he noted. “So to start applying the things we know how to do in the hospital in the pre-hospital setting, we needed [their] guidance.”
Shownkeen added, “It takes time to get this thing going but once you establish that, now it’s like a very efficient machine.”
Time to Treatment Coming Down
While the theory behind mobile stroke units may be sound, it must be proven effective in practice to be considered a viable solution for stroke care. CDH did extensive data collection in the MSU’s first year of operation, taking an estimated 450 stroke calls in approximately 14 months. Over that span, the team has reduced the average time to initial tPA delivery from 82 minutes to 52 minutes — and they are hoping to reduce that number down to 40 minutes. In total, about one-third of patients received tPA within the “golden hour,” a key paradigm of stroke care.
“Thirty minutes in the stroke world doesn’t sound like a lot of time, but it can be the difference between living and dying, between walking out of the hospital versus going to an extended care facility, being able to talk or not talk,” Mohajer-Esfahani said.
The Future of Stroke Care
While the data is bearing out the positive clinical impacts of the MSU, whether it is a viable long-term solution is up for discussion.
As with many new technologies or endeavors, initial cost is a considerable impedance to long-term sustainability. The CDH mobile stroke unit is literally a million-dollar investment. It was made possible through a grant from Northwestern Medicine, a large health system that employs more than 4,000 medical staff at over 100 diagnostic and ambulatory sites across Chicago.
Cost considerations are two-fold, according to Shownkeen: At present, the various elements of mobile stroke care are not reimbursed by the Centers for Medicare and Medicaid Services (CMS), the benchmark by which private insurers guide their policies. Furthermore, drugs like tPA are expensive — a 2016 study found that a standard 100 mg vial of the thrombolytic agent cost approximately $6,400, representing a 111 percent price increase over a decade.4
“It’s going to take a certain amount of patients that are treated to get something that is statistically significant to make a decision whether this is a better way to go about things ... But in the meantime we all agree that giving the drug earlier is the best way to treat stroke,” said Shownkeen.
If these cost hurdles can be surmounted, the idea could eventually be a boon for underserved areas as well. “When we are envisioning the future behind mobile stroke units, there is a huge opportunity to be able to take something and put it in a mobile device and be able to put it in areas that otherwise don’t have access to stroke care of this nature,” added Mohajer-Esfahani.
“It’s just a wonderful opportunity for the community and for us as healthcare providers to be able to own and operate, and experience, something that’s such a grand scale of care,” said Juodka. “We’re treating patients that are extremely time-sensitive with brain matter because it’s something that you potentially don’t ever get back. We’re trying to save people’s brains [and] save their livelihood.”
VIDEO interviews and tour of the CDH mobile stroke unit
References
1. Murphy S.L., Xu J., Kochanek K.D., et al. National Vital Statistics Reports: Deaths: Final Data for 2015, Nov. 27, 2017. Centers for Disease Control and Prevention.
2. Walter S., Kostpopoulos P., Haass A., Helwig S., et al. Bringing the Hospital to the Patient: First Treatment of Stroke Patients at the Emergency Site, PLOS ONE, Oct. 29, 2010. https://doi.org/10.1371/journal.pone.0013758
3. Leidig R.C. Illinois Stroke Data Report, September 2015, Illinois Department of Public Health. http://www.healthcarereportcard.illinois.gov/files/pdf/9_24_15_OPPS_IL%20Stroke_Data_Report.pdf
4. Kleindorfer D., Broderick J.P., Demaerschalk B.M., et al. The Cost of Alteplase Has More Than Doubled Over the Past Decade. International Stroke Conference 2016, Poster Board Number P78 / Presentation Number WP78. https://professional.heart.org/idc/groups/ahamah-public/@wcm/@sop/@scon/documents/downloadable/ucm_471706.pdf


 May 19, 2026
May 19, 2026 









