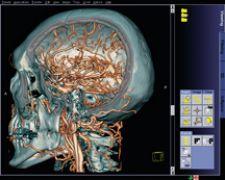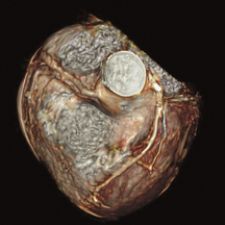
The Ceretom CT scanner can be transported to the ED, aiding in more efficient diagnosis of stroke and brain trauma.
When a sudden interruption of blood flow halts oxygen delivery to the brain, the individual suffers a “brain attack,” more commonly known as a stroke. Medical conditions, such as high blood pressure, carotid artery disease, atrial fibrillation, diabetes and obesity, as well as heredity and age, are common risk factors. As with any disease state, the keys to prevention rest largely on a healthy lifestyle and access to the latest medical advances. Contributing to the latter, the medical industry has made significant headway, according to a Frost & Sullivan research study, in noninvasive imaging of the carotid artery and cerebral neurovasculature, allowing physicians to identify stroke victims sooner than ever.
Physicians prefer effective preventative measures, such as stents and embolic devices, as opposed to working within the narrow and critical time frame they are afforded after a stroke has already occurred, says healthcare analyst Venkat Rajan, author of the F&S study. “CT scans, MRI, angiography, ultrasound and single-photon emission computed tomography (SPECT) are among the myriad novel approaches being explored for mapping out disease states and treatment options,” he explained.
The Need for Speed
The first sixty minutes following a stroke are critical to patient survival. Quick and accurate diagnosis is essential, and CT is one of the best ways to diagnose soft tissue brain injuries. In fact, multislice CT scans can locate injuries from head to toe and provide images of most everything in between, including the vasculature and heart function. In most cases, according to Rajan, CT scans are 95 percent effective in diagnosing potential occlusions or aneurysm sites. They have short acquisition times and can provide highly detailed morphological information.
Unfortunately, CT scanners are expensive and notoriously difficult to maintain, and manning them every hour of the day can add up to hundreds of thousands of dollars. As a result, many rural — and even suburban — hospitals do not have 24/7 CT coverage. A lower-cost, versatile alternative to stationary CT is Neurologica Corp.’s portable CereTom eight-slice head and neck CT scanner, which runs on a rechargeable battery, weighs only 700 pounds and is transportable, meaning that installation may take only minutes instead of weeks. The CereTom transports easily to any point-of-care location within the hospital and transmits wireless images back to a laptop-based workstation. Patients can be scanned immediately upon entry to the ED, dramatically improving their odds for survival. Precious time — between 20 and 60 minutes — of the golden hour can be spent on treatment rather than transporting the patient to radiology.
Recently, researchers at the Mayo clinic discovered that dual-energy CT may help distinguish iron from calcium deposits in coronary arteries. This is significant because the presence of calcium deposits indicate atherosclerosis, or plaque in the artery, a leading cause of coronary artery disease. However, calcium is not the only culprit in blockages. By being able to differentiate iron from calcium, researchers believe CT may prove valuable in differentiating stable from vulnerable plaques.
Imaging in Motion
Another valuable tool for detecting vascular abnormalities is magnetic resonance imaging (MRI), which allows noninvasive evaluation of vascular function using a single modality and without ionizing radiation.
“MRI systems are capable of providing information on flow patterns through phase-contrast techniques, whereby a markedly slow pattern might be identified as a precursor to a developing occlusion,” said Rajan. “A Doppler ultrasound is similarly capable of identifying blood flow speed through noninvasive methodologies and is capable of acquiring information in real time without the risk of radiation. The Doppler system, however, performs with less resolution than an MRI,” he said.
In addition, MRI has the ability to almost immediately detect blockages, not just ruptures, in a blood vessel. As a result, according to study released by the National Institutes of Health (NIH) and published in a January edition of The Lancet, MRI is more sensitive than CT for diagnosing acute ischemic stroke.
“Our results show that MRI is twice as accurate [as CT] in distinguishing stroke from non-stroke,” said the study’s senior investigator Steven Warch, M.D., Ph.D., director of the NINDS Stroke Diagnostics and Therapeutic Section. “Based on these results, MRI should become the preferred imaging technique for diagnosing patients with acute stroke,” Dr. Warch said.
But Walter J. Koroshetz, M.D., NINDS Deputy Director, cautioned that “although MRI is remarkably accurate in detecting early stroke damage, it can’t substitute [a] doctor’s clinical judgment in making a stroke diagnosis and deciding upon treatment. Future studies are needed to determine whether advanced contrast-enhanced CT techniques can afford the same level of clinical information more quickly and with less expense.”
Recent MRI innovations have led to powerful 3T systems, which essentially boast twice the speed and twice the strength of 1.5T systems. While the benefits gained from the higher signal-to-noise ratios may not initially apply to all imaging applications, 3T’s higher spatial resolution and acquisition speeds are key to better diagnostic accuracy for diseases of the arteries and veins.
“3T is very good for vascular imaging,” said Edward T. Martin, M.D., director of Cardiovascular MRI at the Oklahoma Heart Institute. The hope, he says, is that the higher signal will allow for even better imaging of the coronary arteries.
When Less is More
An MRI study of the blood vessels, known as MR angiography, is an excellent tool for assessing artery stenosis — so much so that it has nearly replaced invasive diagnostic angiography at Oklahoma Heart Institute, says Dr. Martin.
Advancements in angiography methodologies now allow for detection and characterization of occlusion or rupture sites in acute hospital settings. “Techniques such as digital subtraction angiography (DSA) allow for identification of specific size and morphology. Angiography and catheter-based imaging have received a significant boost due to refinement of device size and ease of maneuverability,” said Rajan.
While DSA and CTA are currently the gold standards for evaluating blockages in the arteries that supply blood to the brain, data published in the February issue of Radiology indicates that contrast-induced MR angiography produces similar results with less risk to patients. Results were based on comparative studies of contrast-enhanced MR angiography, DSA and CTA and involved 80 patients with narrow or blocked supra-aortic arteries.
“MR angiography, using a small quantity of MRI dye injected into a vein in the arm, can produce detailed images of the arteries supplying the brain and can detect even minor degrees of narrowing or blockage. It does not involve exposure to X-rays and is widely regarded as a very safe, painless test,” Kambiz Nael, M.D., research fellow and radiology resident at the David Geffen School of Medicine at UCLA in Los Angeles, reported in the article. As MR angiography evolves, Dr. Nael believes it will surpass other diagnostic techniques as the method of choice for evaluating the critical arteries that supply blood to the brain.