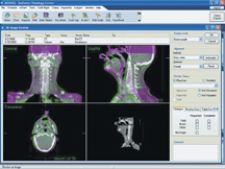
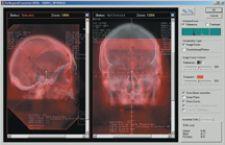
A patient immobilized for a precision radiotherapy treatment on a Trilogy machine with the imaging panel of the On-Board Imager visible just behind her.
Since the 1990s, Americans’ risk of dying from cancer has continued to drop, according to a new report from the nation’s leading cancer organizations.* While lifestyle improvements and screening tools do affect cancer rates, the decline in cancer death rates can partly be attributed to advanced imaging and treatment technologies.
In fact, the rate of incidence for breast cancer in women stabilized in 2001 through 2003 after years of increasing from 1979. Might this be an indication that mammography screening and the efforts to create awareness for earlier detection of this disease by organizations such as the Susan G. Komen Breast Cancer Foundation and the National Breast Cancer Foundation, plus events like the Avon Breast Cancer Walk and National Breast Cancer Awareness Month are finally paying off?
For some experts, the answer is clear – the continued utilization of imaging technology for screening and early diagnosis holds the key to changing the paradigm of cancer care. Dow Wilson, corporate vice president and president, Oncology Systems for Varian Medical Systems (Palo Alto, CA) notes that today the patient is typically seen too late, forging a path of palliative care. “Our mission is to make cancer a chronic disease,” indicated Dow. “As the industry moves forward, we foresee more cooperation between medical oncology and radiation therapy.”
Advancing Imaging Technology and Gauging the Effectiveness of Treatments
“PET/CT is a terrific tool, but how do we make it better?” asked Wilson. “We must use the information more effectively. Anatomical segmentation used synergistically with biological planning will come further into use in the next three to four years as a tool to plan and treat patients.”
According to Timothy Solberg, Ph.D., FACMP, professor and director of Medical Physics in the Department of Radiation Oncology at the University of Nebraska Medical Center (Omaha), the industry’s use molecular imaging, which he characterizes as underutilized today, will become more prevalent in five years. “Radiation oncology departments will move from CT simulation to PET/CT simulation.” As the clinical utility of MR imaging continues to grow, Dr. Solberg believes each department will invest in this technology as well.
Daniel Low, Ph.D., associate professor of Radiation Oncology, Washington University School of Medicine (St. Louis, MO) noted that within the field of radiation oncology, “we will become experts in imaging tumors beyond CT scanning.” His department is investing in its own functional/molecular imaging technology – PET/CT and MRI – as well as the first delivery of the Clinitron 250 Proton Beam Therapy system from Still River Systems (Littleton, MA). “In the next four to five years, we will focus on the ability to detect and image the quantitative characteristics of the tumor.” To accomplish this task, imaging equipment must be in close proximity to the department, with a minimum of spatial distortion and be used in a manner that can yield consistent patient orientation and positioning to further minimize uncertainty at the time of treatment.
“The body moves, and we need images to ensure that our treatments never miss,” said Wilson, who further noted that recent advances in dose painting is heavily reliant on imaging, specifically images obtained immediately prior to treatment delivery.
While the demand is high for imaging technology at the time of treatment, Andreas Schlatter, director of Marketing, Oncology Care Systems, Siemens Medical Solutions (Concord, CA) sees a clear trend toward 3-D imaging. “We believe the use of 3-D imaging capabilities on the linear accelerator will be critical for precise patient positioning,” he said. Yet, even beyond this is the ability to accurately gauge dose delivery. “The direction of Siemens is enabling the linear accelerator to determine actual dose delivery at the time of treatment – essentially to capture dosimetry – for comparison to the original treatment plan. This provides even more information about treatment accuracy.”
Preclinical imaging will also become a crucial tool for evaluating the effects of radiotherapy. Dr. Solberg believes the systematic use of micro-PET, micro-SPECT and optical imaging systems, coupled with parallel imaging studies in humans, will improve our understanding of the effects of radiotherapy at the molecular level and hasten efforts in translating important gains to the clinic.
IGRT and Adaptive Radiotherapy Signal a New Era in Treatment
“The future is going to be image guidance,” said Srinivasan Vijayakumar, M.D., professor and chair of Radiation Oncology at the University of California Davis (Sacramento, CA). UC Davis is gearing for this future by following an approach that provides options for radiotherapy, including the latest technology for IGRT. “We have two Elekta linear accelerators, a TomoTherapy unit and potentially, a smaller version of a proton beam therapy machine in the future,” he explained. The value of this multitiered approach to IGRT will follow the evolution of imaging technology, where one modality has become preferred for a certain procedure over another modality. “This technique will also evolve in radiation oncology.”
IGRT will forge radical changes in patient treatment, believes Jacob Philip, director, Radiation Oncology, IMPAC (Mountain View, CA). “Because we can view physical and physiological changes in patients with both volumetric and functional images with much greater clarity, higher bandwidth and shorter cycle times, prior assumptions are being challenged, and we are discovering that the changes in tumor size, location and movement may be quite different from what we had previously thought,” said Philip.
Recent technological advances are opening new doors, said Del Coufal, vice president of Marketing, TomoTherapy (Madison, WI). “The ability to image prior to treatment improves target accuracy,” indicated Del Coufal, “which should contribute to a reduction in the number of fractions and patient treatments.” Del Coufal foresees a future with the same or better treatment results in less time, which can counteract the fact that resources are not growing at the same rate as the pool of patients. “With the baby boomer generation in the U.S., there is a bolus of potential patients. Our healthcare system must deal with this fact,” noted Del Coufal. Technology, he says, will enable cancer centers to treat more patients, more efficiently, in less overall time.
A key function of IGRT is the continual monitoring of the target site. “If we know how much radiation was delivered to the target and outside the target, then we can adjust the plan, perhaps daily. At the end of treatment, we’ll know exactly what was delivered,” Del Coufal explained. Adapting the radiotherapy plan will make a significant difference in long-term outcomes. Del Coufal cites that some side effects of current radiation therapy continue to create long-term consequences for the patient. Until this shift is complete, the unfortunate byproduct remains that clinicians are “treating a disease today, but creating additional healthcare problems tomorrow,” he added.
Information Technology Enables Adoption of Advanced Technology
By its very nature, radiation oncology is a technically advanced specialty, one that involves a multidisciplinary approach to medicine, says Philip. This has significantly encouraged radiation oncology to embrace information technology (IT). He also believes radiation oncology is “the beacon of light that provides an excellent prototype for an electronic environment in healthcare services.”
IT solutions are a fundamental tool to handling the ever-increasing volume of information, Schlatter noted. “Integrated software solutions will enable the delivery of information in an easy-to-use format, available everywhere and anytime.” Yet, he believes that information must be provided in a format tailored specifically to each team member in the radiation oncology department – the physicist, dosimetrist, therapist and oncologist.
Philip foresees in the next three years a continued evolution toward a fully electronic environment. “Sites that have integrated an electronic medical record will find the transition to IGRT much easier than those sites that have not.” According to Philip, the comparison of predelivery images and information to reference images and plans will be performed using historical data and clinical decisions made with the aid of automated decision-making tools and algorithms.
“Volumetric image guidance will be a huge eye opener, challenging existing longstanding assumptions further entrenching our reliance on IT and the now broadly accepted standard of a multidisciplinary approach to radiation oncology,” Philip added.
For Low, understanding the differences in tumors will help facilities better “fine-tune fractionization.” Information technology and data mining are critical factors to creating a greater understanding. “As we increase on-board and modality imaging, data analysis will also increase. The use of informatics is a logical extension,” he explained.
Dr. Vijayakumar agrees that IT is crucial to the process of replanning and redosing the patient, yet he sees a broader utilization that will tap into the “unbelievable volume of information being collected.” He envisions a robust, computational system that promotes data mining and outcomes management. “It is more than that, but we need to do (data mining and outcomes management) right first. With physics, biology and technology, if we integrate these disciplines correctly, then we can come full circle and address other diseases beyond cancer.”
Biology and Molecular Imaging Key Contributors
While radiation oncology has witnessed revolutionary progress in technology, physics and engineering, there has been a less noticeable tapping of the revolution in biology. “These parallel evolutions must bridge together to improve outcomes and enhance patient care,” noted Dr. Vijayakumar.
Molecular imaging will move beyond PET, says Dr. Vijayakumar. “When the breakthroughs happen, we will target tumors at multiple dimensions. Molecular imaging will identify areas that are more hypoxic, that possess more growth potential and identify areas that are more resistant to radiation.” By identifying these areas, different types of technology can then be utilized to their full potential to deliver dose to the targets.
“Clearly, the past five to 10 years have been technology-driven, based upon physics and focused primarily on delivery devices and techniques,” said Dr. Solberg. “In the next 10 years we will see a movement away from physics and back to biology.” Molecular imaging in both the preclinical and clinical settings, to look at specific processes associated with cancer such as proliferation, hypoxia and angiogenesis, will greatly expand the use of radiation as a targeted therapy.
The Result: Personalized Treatment
Motion management, either with external or internal markers, will take on a heightened importance as more facilities embrace IGRT. “Motion, coupled with precise identification of tumor location and structure, will lead to dynamic adaptation,” said Wilson. Clinicians will leverage information at each step of the treatment process to increase performance and capabilities. “We will evaluate the patient across the enterprise” by integrating radiation oncology information with other patient data, he added.
Low noted that continued research will quantify the biological response of tumors to radiation therapy and lead to personalized radiotherapy. “We will encounter a new realm of imaging technology that will allow the invivo monitoring of how tumors act and respond to further differentiate one patient’s tumor versus another.” He notes that treatment planning is “all about prediction” and tomorrow’s technology will provide the necessary information that will enable clinicians to make modifications to those predictions.
The industry has already learned a one-size-fits-all approach doesn’t work with each patient. Added Dr. Solberg, “We will modify patient treatment based on imaging the biology of the tumor – in particular, the tumor’s response. The ‘diagnose-plan-treat-assess’ cycle that molecular imaging enables provides an excellent opportunity for individualizing cancer care to an extent never before possible.”
*The North American Association of Central Cancer Registries Inc. (NAACCR); the National Cancer Institute (NCI); the American Cancer Society (ACS); and the Centers for Disease Control and Prevention (CDC). Published in the October 15 issue of Cancer, the “Annual Report to the Nation on the Status of Cancer, 1975-2003, Featuring Cancer among U.S. Hispanic/Latino Populations” analyzed comprehensive data that demonstrates the long-term decline in overall cancer death rates through 2003.
Mary Beth Massat is a healthcare freelance writer based in Crystal Lake, IL. She is president of Massat Media, a public relations and communications firm for the healthcare industry and can be reached at [email protected] or 224.578.2388.