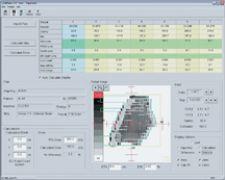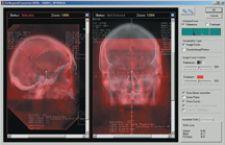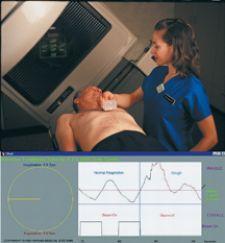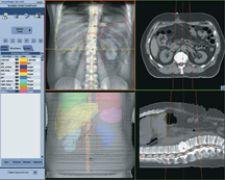
IMPAC's Setup Intelligence tracks clinical quality using the tools to perform planar IGRT, record and trend the parameters within the patient's EMR.
The tremendous accuracy with which a physician can treat tumors with Intensity-Modulated Radiation Therapy (IMRT) is the very nature of the technology’s problem. IMRT’s high degree of accuracy compared to conventional radiation therapy allows physicians to deliver higher radiation doses, yet, its precision in clinical applications is hindered by patient and organ movement. To raise the bar and develop instruments that facilitate greater accuracy in IMRT, vendors are enhancing quality assurance (QA) platforms with the aid of dynamic visualization tools such as respiratory gating, Image-Guided Radiation Therapy (IGRT) and soon 4-D adaptive dynamic radiotherapy.
QA Puts IMRT in Check
Some techniques are all in the wrist, but with IMRT it is all in the planning. Like any good plan, however, it requires a review stage, known as QA in IMRT. During the planning process, once the CT scan is complete and calculates the different structures of the internal anatomy, the physician identifies the objects to avoid – such as the spine, the other lung or the heart. The system then calculates a number of beams to be used from different angles and outputs the parameters at which to set the delivery device. QA verifies that the linear accelerator will deliver the exact same parameters calculated by the computer.
Varian’s QA solution, Argus, analyzes data to ensure that the linear accelerator is operating correctly, and Argus IMRT verifies that the multileaf collimator (MLC) is operating as programmed. Complementary to Argus is PortalVision Portal Dosimetry, which offers another way of accomplishing dosimetric verification of patient treatments. The product complements the Argus IMRT product in that the latter concentrates on MLC motions and turns that information into fluence maps, while the former concentrates on a measured dose map that is then compared to the intended dose map from the treatment planning system.
Typically, the QA program creates a second patient or a phantom and imports the beam parameters into that second patient, upon which it delivers dose to test for accuracy. Other devices perform the QA right within the patient’s chart to assure that the beam parameters are consistent.
“We have built into IMPAC the ability to deliver the quality assurance from within the patient’s chart. So the QA that you perform for a given patient may be performed using the same delivery parameters as with the actual treatment,” said Jacob Philip, director, Radiation Oncology Business Unit, IMPAC Medical Systems Inc. “Additionally, clinical quality may be tracked using Setup Intelligence. This module provides the user the tools to perform planar IGRT, record and trend those parameters all within the patient’s electronic medical record.”
In any QA program, time is of the essence in the verification process. Standard Imaging’s QA BeamChecker, a new wireless QA system, automatically detects the type and quantity of energy coming out of beam design to speed up the measurement process. “There is build-up in the QA BeamChecker unit, so they don’t go into the linear accelerator vault or bunker to put on build-up materials for higher energies,” explained Eric DeWerd, sales manager, Standard Imaging. “It makes it faster to take the measurements in the morning.”
Flexible Beam Execution
In high-resolution conformal radiation therapy the beam head plays a critical role as it allows the physician to conform the dose very tightly to a small or irregularly shaped target.
At the Richardson Regional Cancer Center-UT Southwestern Medical Center, Radiation Oncologist Dr. Edward Gilbert, director of the Lance Armstrong Shaped-Beam Radiosurgery program, uses BrainLab’s Novalis Shaped Beam Surgery System for stereotactic radiosurgery, stereotactic radiotherapy and IMRT. Novalis is applied in highly precise treatments of brain, head and neck tumors and is designed to shape the radiation beam to match the contour of the targeted area. Sophisticated software calculates the ideal access points to the tumor or lesion and defines the treatment plan to produce high-precision of the beam for delivery.
“One thing BrainLab has is a 3 mm micro multileaf that shapes with exact curvature — most are 5 mm. The Novalis is essentially a head. The second addition allows precise radiosurgery delivery with multiple angles. Having control of the beamlets on or off allows further curvature and better shape the angulations. No matter what angle you come into, it allows you to more accurately determine the shape around what you do and don’t want to treat,” said Gilbert. “It’s really easy to use because of the software and its flexible.”
Ease of use prompted Jatinder Palta, professor and chief of Physics, department of Radiology and Oncology, University of Florida, to “transfer patients to an Elekta linear accelerator,” indicated Palta. “Elekta’s equipment provides more of a collision- free zone. Also, it has a more compact treatment head so it is easier for the therapy.”
Even such high-precision beams are not fully equipped without a QA system. Beams such as Varian’s SmartBeam, engineered to sculpt dose around critical structures, contains tight controls in the QA stage with SmartBeam’s IMRT QA because the beam could damage healthy surrounding tissue.
Take a Deep Breath
Despite advances in contouring capabilities, physicians like Dr. Gilbert are looking for greater accuracy still through respiratory gating. “IMRT exists in every machine, but IMRT still is stuck with the edges of your beam and there is a lack of precision,” indicated Dr. Gilbert. “You have accuracy, but the real quantum leap is the gating – the ability to track when the patient is breathing.”
Gating is one of the many technologies that tracks tumor motion during the respiratory cycle. To check for accuracy, respiratory gating also uses QA to simulate the breathing of a patient and account for respiratory motion. “Respiratory gating tracks the motion. You use IGRT to make slight adjustments caused by the respiration. So you gate the beam. The actual gating is only a couple of minutes. You really don’t realize how much of a change respiration can make,” noted Michael Greenberg, M.D., Dale and Frances Hughes Cancer Center, part of the Pocono Medical Center in East Stroudsburg, PA.
One of the latest QA programs for a respiratory gating platform is by Standard Imaging, which is installed in Varian’s RPM system. “Varian has the RPM Respiratory Gating System that accounts for a person’s breathing while doing IMRT, so our application simulates a patient’s breathing to help physicians commission the RPM software to use respiratory gating on patients,” said DeWerd.
Other methods for tracking breathing are active breathing coordination and passive radiofrequency transmitter technologies where small radio transmitters are implanted into the target structure. As the target structure moves, the transmitters convey the location of the target. “The only thing that gives you an indication of the target in real time are the passive radio frequency transmitters by Calypso, which recently got 510(k) approval and available soon,” Philip added, referring to Beacon transponders by Calypso Medical, that once implanted send signals that generate objective location instructions to the radiation therapist to register treatment target to an isocenter prior to treatment.
However, as Philip points out, “[a]ccuracy is limited by what you can visualize when you are dropping the dose. The information needs to be dynamic because the target is variable.”
IGRT - Beyond Visual Limits
One of the innate resources we take for granted is our own vision. The physician’s ability to see inside the patient with the naked eye can enhance a surgeon’s precision exponentially. IGRT facilitates IMRT visually, using either planar images, cone-beam CT or fluoroscopic imaging – a radiation beam that takes pictures of the inside of the anatomy and produces full motion or video.
The IGRT system assists IMRT by automatically adjusting to the patient’s position through rotational and translational corrections, while at the same time enabling high-quality imaging. “What the IGRT does is controls for the 4th dimension, which is patient and organ movement. It evaluates the movements before and during treatment,” said Dr. Greenberg . “You evaluate organ movement with markers or by using cone-beam. Then you match the CAT scan for treatment planning and just before treatment, using cone-beam when the patient is on the table.”
As with IMRT, “IGRT requires a QA program centered around the equipment itself to check the quality of the images generated and the accuracy of the measurements,” emphasized Philip. “For instance, if I go to measure two points, there is a QA that goes into checking that. It involves different kinds of phantom material – surrogates for anatomical objects and still taking a picture before you deliver. You could use the same equipment to generate images in any three modes. The mode that is preferred for doing IGRT is cone-beam because you have 3-D data not 2-D, and 3-D helps better define location of the tumor.”
As part of Elekta’s strategy to develop more integrated products that address patient and organ movement through IGRT, it recently acquired Medical Intelligence Medizintechnik GmbH (MI) for $24.5 million. One of MI’s more innovative products, the HexaPOD RTC, is an image-guided robotic patient positioning system that approaches patient positioning with a 6-D system designed to correct rotational errors in patient positioning and translational (x, y, z) errors in addition to delivering sub-mm accuracy.
4-D Opens New Doors
The next level of accuracy in radiation therapy is 4-D adaptive dynamic radiotherapy, which optimizes the use of IMRT and IGRT.
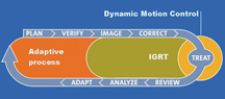
In an IGRT-driven 4-D Dynamic Adaptive Radiotherapy (DART), the 4-D data seamlessly integrates into the planning process, enabling a physician to precisely hit moving targets. The key component of 4-D DART is dynamic targeting – it responds to tumor motion during radiation therapy treatment delivery.
“Where things are going is 4-D adaptive radiotherapy to assess dosimetry on the fly,” said Greenberg. “It will actually change the plan a bit and get the information in real time. It recalculates the plan and gives you new dosimetry every day and gives you a new plan.”
One solution for DART is Varian’s treatment approach that involves tying together the imaging, planning and treatment steps of the radiotherapy process through an integrated network of technology that makes use of new, real-time information to enable clinicians to modify the treatment as time progresses and conditions change.
GE Healthcare has also integrated its 4-D imaging and planning technologies to create AdvantageSIM MD, a simulation and localization program for precise and rapid radiotherapy.
While 4-D may be the next best thing to X-ray eyes, with every leap in imaging for radiotherapy, QA is still a necessary step toward accuracy – even in real time.