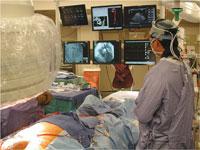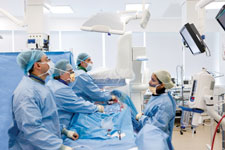
Dr. Krassi Ivancev and staff in the University College London Hospitals in the United Kingdom perform a hybrid procedure in their GE-installed hybrid OR.
One of the biggest trends is the creation of hybrid operating rooms (ORs) that bring together the best of both surgical and interventional technologies. They are centered around a high-quality angiographic X-ray imaging system, allowing new collaborative treatment strategies and new types of procedures. Users say the shift to hybrid ORs is more than a change of venue for procedures, it is a paradigm shift in medicine.
The hybrid suites will facilitate the use of the transcatheter valve replacement and repair technologies. They also are being used to increase efficiency in patient care by combining open surgical and interventional procedures in cardiac, vascular, neuro and electrophysiology (EP).
The advantage of hybrid ORs is the ability to perform multiple, complicated procedures in one location at the same time, especially on patients with multiple co-morbidities, said Syed Hussain, M.D., director of vascular and endovascular surgery, OFS Healthcare System, Proctor Hospital, Peoria, Ill. He said combined procedures include endarterectomy of the carotids, abdominal aortic aneurysms (AAA), and peripheral vascular bypass graft combined with percutaneous coronary interventions (PCI).
His hybrid was installed in December 2010, and is centered around a GE Innova system capable of 3-D rotational angiography reconstructions for better diagnostics and procedures.
“Complicated procedures is where everything is moving today,” he explained. “The perk of using a hybrid lab is you can do all the procedures, all in one shot. It’s also nice for the patients, because it does not waste their time...There are so many procedures now where a cardiologist and a cardiac surgeon need to work together.”
In the case of cardiac patients brought in from the emergency room, Hussain said they can be sent to a hybrid OR for a diagnostic angiography and then either cardiac surgery or PCI can be performed in one location.
Planning Ahead is Key
Hussain said you need to consider all players who would use the room and include them in the planning process. This may include vascular surgeons, cardiac surgeons, interventional cardiology, electrophysiology and interventional radiology.
Any specialties that will be using the OR need to be involved in the planning so their needs are met, said Joe Coatti, M.D., FACS, senior vascular surgeon, Middlesex Hospital in Middletown, Conn. In addition, nursing staff should have a say during planning so in-room procedural storage needs and how patients are brought into the room are considered. Anesthesiologists also should be included. Coatti said discussions at his facility resulted in gas lines being installed as part of a movable overhead Nu Boom system.
Another factor to consider is where the growth in patient volume is coming from and if it requires a hybrid OR. Hussain said much of the patient volume increase at his hospital has been from vascular cases, not cardiology. The hybrid OR is needed in these cases because high-quality angiography is needed, surgical cut-downs are sometimes used and surgical bypass procedures are frequently performed. The high-quality imaging also is needed for precise deployment and detection of endoleaks in aortic stent grafts.
“Vascular surgeons are the biggest advocates,” Hussain said. “Any hospital that has a large vascular volume needs to consider a hybrid OR.”
TAVI and Hybrid ORs
While transcatheter aortic valve implantation (TAVI) is viewed as the poster child hybrid OR procedure, experts warn that TAVI volume may remain small and concentrated in only a handful of specialty centers.
The Cardiopulmonary Research Science and Technology Institute (CRSTI) in Dallas, Texas, created two hybrid operating rooms specifically for participation in the PARTNER trial for the Edwards Sapien transcatheter aortic valve. While the devices could be implanted in a cath lab, the facility wanted the option of converting to an open surgical procedure if needed, said Angela Riley, RT, CRSTI executive director. However, of the 200 implants performed, she said only two have converted to an open chest surgical procedure.
Riley cautions cardiology departments from creating a hybrid lab in anticipation of doing transcatheter valve procedures once these devices are cleared by the U.S. Food and Drug Administration (FDA). She said the FDA already plans to limit the number of sites allowed to perform the procedure to about 20 centers, due to the complexity and the need for enough volume to create experienced operators.
“I think it’s going to be a very slow adoption rate, because the technology is not that user-friendly,” Riley said. She feels it will be several years before TAVI technology expands to a large number of centers.
She said the rapid expansion of vascular procedures is a more compelling argument for building a hybrid suite.
“You want to build your case for a hybrid OR and present to your CEO based on your vascular program – not your cardiac program,” Riley said.
Cross-Training is Key
Hybrid procedures will become increasingly more important to patient care in the next few years, said David R. Holmes, M.D., Mayo Clinic, Rochester, Minn., during an ACC 2011 session on new cardiovascular devices and advances over the next decade. He said this will require several specialties working together in the hybrid space to achieve better patient outcomes. This will require cross-training of cardiovascular surgeons, interventional cardiologists, vascular radiologists, intensivists, OR and cath lab procedural techs.
“The next decade is going to be about group training,” Holmes said.
Make sure everyone knows their role in a procedure and understands the protocol for an OR and working near radiation fields, Riley said.
“We had a lot of problems when the cath lab team came down to the OR. They just did not have the same level of sterility in the cath lab,” she explained. “Everyday is a school day.”
Hybrid OR Requirements
Cath labs usually are not suitable to convert into a hybrid OR because they were not designed to meet OR requirements, said Linda D. Gillam, M.D., FACC, Columbia University Medical Center, during a packed presentation at ACC 2011.
She said the top requirements for a hybrid OR include:
• Higher capacity airflow
• High-quality fluoroscopy system (mobile systems generally do not have a high enough image quality)
• Money – at least $2.5 to $3 million for a hybrid space
• “Marry” the cath lab and OR cultures
Planning considerations include:
• Location for equipment
• HVAC installation with minimal vibrations to aid image quality, so involve structural engineers in the planning
• Radiation concerns – need to educate staff
• 14-foot ceiling clearance for a fixed C-arm
• Use of hybrid as “swing space,” where it can be used for either PCI or surgical cases (so the pricey investment does not sit idle)
She also said hospitals need to consider reimbursement and procedural volume issues. In some cases, a hospital might only be reimbursed for one procedure (PCI or OR). Many hybrid procedures being developed are still investigational procedures, which are not reimbursed. Also, if another area hospital already offers the hybrid procedures you are considering, is there a need, or will the new hybrid OR just split and lower procedural volume at both hospitals?
However, in an era of expanding patient consumerism, a hybrid OR may offer a marketing advantage over competing hospitals. “If the goal is state-of-the-art care, then the hybrid OR is right for you,” Gillam said.
High-quality, fixed angiography systems are a key component of the hybrid, providing better image quality than mobile C-arms.
“Mobile imaging systems are just not good enough,” Riley said. “You can’t see your bony landmarks. Imaging is critical.”
Size Matters
The hybrid rooms need to be larger to accommodate both surgical and interventional equipment, especially a large, fixed angiography imaging system. An average cath lab or OR is about 650 to 700 square feet. Estimates for the ideal-sized hybrid OR from facilities that have created such suites range between 900 and 1,000 square feet.