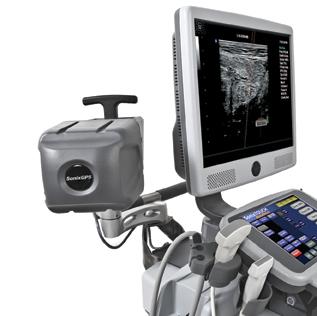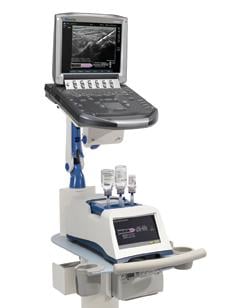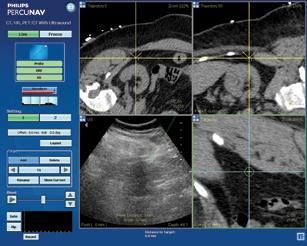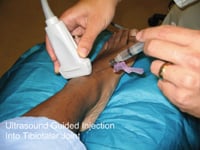
Figure 2: The Navigator DS is set up, with the image-guided needle placing medication into the ankle joint.
Musculoskeletal impairments are reported by more than one out of every four Americans, and in 2008 an estimated 46 million, or one in five adults, reported arthritis.1 That number is expected to increase to 67 million by 2030.2
Treating Musculoskeletal Impairments
To address the growing number of patients with musculoskeletal impairments who complain of joint pain and decreased functions, physicians typically use a variety of therapies. The traditional cascade of care is initiated with oral pain medication, followed by injection of corticosteroids or viscosupplementation, and finally, in end-stage disease, total joint replacement.
While the use of oral pain-killers has been the most common early intervention for joint pain, physicians and patients are increasingly concerned about the long-term side effects of systemic drugs.
Intra-articular and periarticular injections of corticosteroids, anesthetic agents and viscosupplementation products are increasingly being used by physicians as early interventions for pain relief. They are used to reduce inflammation, pain and stiffness, and to diagnostically identify symptomatic structural changes. The shoulder, elbow, knee and foot are among the most common joints that are aspirated and/or injected.
Local injections of therapeutic agents into articular structures can lead to rapid decreases in pain and inflammation without many of the serious side effects associated with systemic medications. In many instances, these minimally invasive and cost-effective treatments can delay and even eliminate the need for surgical intervention. However, as with any diagnostic or therapeutic procedure, success depends on the expertise of the clinician and the accuracy with which the medications are injected into the affected joint space.
Current Injection Accuracy Challenges
The accurate injection of therapeutic or diagnostic agents into the intra-articular space depends on a variety of contributing factors, including patient anatomy, physician skill and the patient’s tolerance of the procedure itself. The standard method for intra-articular injection involves the use of manual palpation and anatomical landmarks to identify the target location and injection pathway, also referred to as a “blind” injection. The degree of pain relief and functional improvement is greater when the injection is delivered accurately to the intended location.
Misplaced injections can also pose risks, such as soft tissue damage, tendon weakening, skin depigmentation with corticosteroid injections, and inaccurate images with extra-articular contrast dye.
Ultrasound as a Guidance Tool
In musculoskeletal practice, ultrasound is an emerging imaging modality which affords dynamic, real-time, cost-effective and physician-controlled visualization of anatomic impairments. Ultrasound can be used at the time of injection to locate the joint space, during the procedure to follow the needle in real time, or after the needle placement to adjust an incorrectly placed needle. Recent data has demonstrated that the use of ultrasound imaging improves accuracy rates in joint injections.3, 4
The Yale University School of Medicine has implemented the Navigator DS delivery system, a computer-controlled, image-guided injection system intended to increase the accuracy, efficiency and safety of musculoskeletal injections.
The Navigator DS prepares physician-prescribed injections from standard multi-dose anesthetic and steroid drug vials, while the ultrasound screen provides the physician with real-time visualization of the needle position, fluid delivery process and prescription volume. This is important, as accurate drug delivery may help to reduce the need for repeat injections, which in turn reduces costs and improves patient care. Precise dose preparation also helps to ensure that doctors use no more or less drugs than needed.
By simplifying the injection set-up process and utilizing ultrasound guidance, preparation time is reduced to just minutes and the procedure can be performed by a single operator. After the injection is delivered to the painful joint, the system records the treatment data and automates a record for transfer to an electronic record management system or direct printout. Initial studies demonstrate that a moderately busy practice can save more than 30 minutes in preparation time in a typical day.
Additionally, the Navigator DS assures the sterility of each vial and eliminates needle exposures to healthcare workers, as the drugs are accessed a single time with a sterile, filtered, needle-free vial adapter.
A Case Study
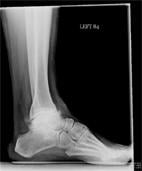
Mr. RS is a 54-year-old active gentleman who has had severe ankle pain over the past six years. He had an ankle injury while serving his country in the military and now has large bone spurs, joint space loss and significant loss of function, with difficulty walking on uneven ground. His primary care physician initiated a course of nonsteroidal anti-inflammatory medications, physical therapy and brace treatment to no avail: The pain continued to affect his life and activity level. After considering his options, Mr. RS elected to proceed with image-guided injection of local anesthetic and steroid mixture into his ankle joint. The goal of the image-guided injection was to improve his function, decrease his pain and diagnose the source of it.
As can be see on his X-rays (Figure 1, below), there was significant joint destruction in both the ankle (tibiotalar) and subtalar joints. Sequential targeted injection into first the ankle joint, followed (if needed) into the subtalar joint, would allow Mr. RS to “test-drive” any further intervention on these related, but separate, joints. Figure 2, above, shows the Navigator DS setup with the image-guided needle placing medication into the ankle joint. The procedure was completed in less than two minutes.
Mr. RS reported immediate 100 percent relief of pain, confirming symptomatic disease in only the ankle and not the subtalar joint. At three months he continues to be pain-free and back to full function.
Image-guided injections through the Navigator DS allow physicians to specifically target hard-to-reach joints. As our active population continues to pursue full function and exercise, despite traumatic and over-use injuries, there is a pressing need to provide cost-effective, but accurate, treatment modalities. Image-guided injections stand as the crossroads between medical treatment for such disorders and surgical debridement and joint replacement techniques. Image-guided injections represent an intervention that is more invasive than a pill, but less traumatic than the knife. They allow the treatment of a wide variety of patients experiencing pain and loss of function in anatomic locations as disparate as the spine and the small joints in the pinky finger.
References:
1. “United States Bone and Joint Decade: The Burden of Musculoskeletal Diseases in the United States.” Rosemont, Ill. American Academy of Orthopaedic Surgeons, 2008. www.boneandjointburden.org/pdfs/bmus_executive_summary_low.pdf.
2. “Arthritis: Meeting the Challenge.” Atlanta, GA: National Center for Chronic Disease Prevention and Health Promotion. 2009. www.cdc.gov/NCCDPHP/publications/aag/pdf/arthritis.pdf.
3. “Accuracy of ultrasound guided injections in the foot and ankle.” Foot Ankle Int. 2009 March;30(3):239-42.
4. Daley E, Sarvottam B, Bisson L, Cole B. “Improving Injection Accuracy of the Elbow, Knee and Shoulder.” American Journal of Sports Medicine.Vol 39, No 3, pp 656-62, March 2011.