Gail E. Latimer, MSN, RN, VP, chief nursing officer, Siemens Medical Solutions USA
Information technology (IT) solutions are playing perhaps the most vital role in fulfilling the goals of the 100,000 Lives Campaign initiated by the Institute for Healthcare Improvement (IHI). IT supports four proven interventions in the critical care setting, interventions that are, bottom line, bolstering patient safety in the hospital and reducing hospital deaths by underpinning evidence-based protocols for acute care clinicians.
The IHI campaign is the first national effort to promote saving a specified number of lives by a certain date (June 14, 2006). IHI proposes to achieve this goal by engaging U.S. hospitals in a commitment to implement specific changes in care (a.k.a. “Proven Interventions”) that have been shown to improve patient care and prevent avoidable deaths.
Nearly 3,000 hospitals have enrolled in 100,000 Lives, representing more than 90 percent of all U.S. patient discharges and 89 percent of all acute care beds. Other groups such as the Robert Wood Johnson Foundation, the American Medical Association, the American Nursing Association and the Joint Commission on Accreditation of Healthcare Organizations, as well as several federal agencies, have also pledged their support.
Since its inception in 1991, IHI has become a major force in the healthcare industry over the past decade. A not-for-profit organization dedicated to advancing the quality and value of healthcare, IHI drives broad-scale adoption of changes by spreading improvement knowledge around the globe.
IT Plugs Into the Program
IT solutions can support the 100,000 Lives Campaign and other IHI initiatives to improve outcomes and quality of care by helping to change processes and behaviors in healthcare organizations. In a data-driven approach to Proven Interventions, the IT system can facilitate the process of care delivery through alerts and reminders and then track the clinicians providing the care.
But that’s just the beginning.
Areas in which IT can have a major impact on healthcare safety and quality include:
• Workflow management to ensure that the process and plans of care are executed or delivered
• Evidence-based practice, which creates and pushes knowledge to physicians, nurses and other clinicians to support clinical decision making
• Embedded analytics, metrics and reporting tools to deliver meaningful information to clinicians and healthcare executives
Proven Intervention No. 1: Rapid Response Teams
Deployment of Rapid Response Teams (RRTs) is one example of an IHI Proven Intervention that has successfully incorporated IT. RRTs respond early to critical warnings of a patient's deteriorating condition, preventing a cardiopulmonary arrest. (Seventy percent of patients show evidence of respiratory deterioration within eight hours of arrest, and 66 percent show abnormal signs and symptoms within six hours of arrest, and a physician is notified in only 25 percent of the cases).
Fortunately for my own family, an RRT was initiated when my brother-in-law was hospitalized, resulting in the immediate delivery of clinical expertise to his bedside for interventions that addressed his crisis. Research cited by IHI has shown that in such instances, the presence of an RRT reduced the number of cardiac arrests prior to the patient being transferred to the ICU to four percent (down from 30 percent).
This role requires quick access to patient information, which can be facilitated by the use of an Electronic Health Record (EHR). As the RRT arrives, the patient's pertinent data — such as current lab results with PH, medication, EKG, etc. — are immediately, electronically pushed to the team. In fact, the EHR can be on an electronic wireless tablet in the hands of the team as it arrives.
The future holds the promise of an intelligent EHR. This would use clinical decision support based on logarithms to notify the RRT automatically with critical information, or “triggers,” documented at the point of care by the clinicians.
Proven Intervention No. 2: AMI Protocols
Evidence-based acute myocardial infarction (AMI) protocols are another IT-enabled Proven Intervention. Every year, an estimated 1.1 million people in the U.S. are diagnosed with an AMI, and approximately 350,000 of these patients die during the acute phase. Clinicians in many healthcare organizations are now using protocol-driven, point-of-care documentation tools and order sets to deliver evidence-based care in support of the seven key components for AMI care recommended by the American College of Cardiology and the American Heart Association:
1. Early administration of aspirin
2. Aspirin at discharge
3. Early administration of beta-blocker
4. Beta-blocker at discharge
5. ACE inhibitor or ARB at discharge
6. Thrombolysis or reperfusion intervention
7. Smoking cessation counseling
These evidence-based guidelines are being introduced as a way to standardize care that provides safe, quality outcomes throughout the care continuum.
First, within the admission assessment, IT-supported linkages to knowledge management content (provided by developers such as Zynx Health) can be accessed to support a diagnosis based on the specific findings. Then, patient data and the evidence-based knowledge can be integrated as part of the clinician workflow and plan-of-care, with technology bringing the information to the bedside for the clinician and patient to access. And prior to discharge, links to patient-education information can support dissemination of patient-specific education.
Technology-driven workflows can also benefit the care of an AMI patient. Beyond simple alerts or reminders, a workflow engine is sensitive to time; it escalates tasks, synchronizes multiple events and triggers multiple actions simultaneously. For example, a workflow engine can remind the clinician that a beta blocker was not ordered, give another care provider a prompt to initiate smoking cessation education or inform the physical therapist of the results of the functional assessment done by the nurse.
Embedded reporting and retrospective monitoring can be used to ensure that staff members actually perform the required and recommended activities. At McLeod Regional Medical Center in Florence, S.C., this approach has succeeded in cutting the death rate among its heart attack patients from 10 percent to about four percent.
Proven Intervention No. 3: Prevention of ADEs
Nationally, the occurrence of adverse drug events (ADEs) averages two to eight percent per 1,000 doses. However, prevention of many ADEs can be achieved through clinical solutions creating a “closed loop” workflow. Components of the loop include medication reconciliation, computerized physician order entry (CPOE) and bar coding of medications.
Medication reconciliation is the process of creating the most accurate list possible of all medications a patient is taking — including drug name, dosage, frequency and route — and comparing that list against the physician's admission, transfer, and/or discharge orders. The goal is to provide correct medications to the patient at all transfer/hand-off points within the hospital and across the continuum of care (including outpatient to inpatient, pre- and postintrahospital transfers and discharge).
The collection of home medications is a crucial part of the process. The home list and active Medication Administration Record follow the patient through every care setting. CPOE users can view a summary of the home medication(s) before placing inpatient medication orders in the system. As new medications are ordered, the system coordinates justification documentation with ordering and, through IT-enabled workflow, notifies and escalates any unreconciled medications.
Embedded analytics within an IT system can monitor the process, reviewing charts and discharge summaries for adverse drug events that occurred as a result of inadvertent discontinuation of a medication or a missed order at a point of transition.
To assist with reconciliation, comparisons can also be made with external data sources/warehouses that can bring the interdependent list of the patient's medications into the assessment. One such source is RxHub, a health information exchange company that electronically routes up-to-date, patient-specific medication history and pharmacy benefit information to caregivers at every point of care. In a single quarter, RxHub may receive more than 500,000 requests for medication histories.
CPOE integrates technology directly into the decision-making processes and workflow of physicians and nurses, providing clinicians with a concurrent clinical decision support tool that helps improve patient safety by increasing compliance with evidence-based guidelines. Through its data-driven protocols, CPOE helps reduce ADEs in several ways:
• Automated clinical checking for drug allergies and drug interactions as the physician places the order
• Avoidance of errors in interpretation, via clear, legible physician orders (In the past, nurses were regularly faced with the challenge of reading and interpreting the physicians' written orders.)
• Automated alerts when certain lab values (e.g., potassium level) are abnormally high or low
• Automated alerts on medication doses that may be too high or too low
• Automated adverse drug reaction reporting
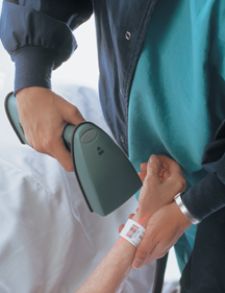
Medication administration using bar codes involves several levels of electronic safeguards to ensure that the “5 Rights” (right patient, drug, dose, route, and time) of medication administration occur and that drugs aren't given without these checks. First, nurses scan their bar-coded employee ID badge to sign on and identify themselves (or touch a biometric computer mouse, which reads the nurse's fingerprint), setting the appropriate security access level to automatically track and document every detail of system use. Then the medications themselves are checked by their bar-coded labels.
When all medications have been scanned and verified, the system prompts the nurse to scan the patient's bar-coded ID wrist bracelet. The system verifies the correct patient, or immediately warns of the wrong patient, helping to prevent the most serious potential errors with an audible alarm and a visual alert. Once the patient has been positively identified, the nurse is able to chart additional information such as vital signs, pain scale, pain location, reasons and administration sites.
By creating a culture of safety and a “no blame” environment, health systems are encouraging clinicians to identify and report medication errors. In addition, IT decision support with built-in rules can alert nurses and physicians of potential harm. The Institute for Safe Medication Practices (ISMP) has developed a trigger tool that signals when an ADE may have occurred, based on the point-of-care documentation, CPOE and lab results. For example, a blood sugar level below 50 in a diabetic patient may suggest an insulin dose error.
Proven Intervention No. 4: Prevention of Infections
Similar to ADEs, prevention of infections such as central line infections, surgical site infections and ventilator-associated pneumonia can be supported by standard order sets, alerts, embedded analytics supported by a data warehouse and workflow escalation coordinated with documentation and orders.
For example, simple rules can alert clinicians that a patient is at risk for nosocomial infections and other adverse events. From these alerts, the system can suggest potential interventions. This online decision-making support makes it easy for clinicians to adhere to standards of care.
Measuring Outcomes
As we face a potential future of pay for performance, healthcare organizations will increasingly leverage technology to measure outcomes and integrate clinical practice standardization. Solutions are being implemented today that monitor and generate clinical knowledge, measure performance to improve best practices, collect and manage data for quality reporting and use the generated data for ongoing quality improvement efforts.
By documenting care in an EHR, for example, that information is permanently captured, allowing evaluation of care delivery based on metrics for outcomes and processes. A Clinician Report Card can be used to provide ongoing feedback, encourage the adoption of new processes and examine historical data to develop benchmarks (which can be unit- or department-specific, disease-specific, or individual physician/nurse-specific). Institution leaders can use these tools to help identify where the clinicians need to focus, determining who has adopted new processes and who requires additional coaching or mentoring.
Patient safety requires a comprehensive approach backed by people, processes and technology. To support the outstanding work driven by IHI, healthcare IT systems can help identify, capture, analyze and share best practices, adding to the body of clinical knowledge and effectively transforming existing standards of care, based on clinical evidence.
Statistics reprinted from www.IHI.org with permission of the Institute for Healthcare Improvement (IHI), (c) 2005.



