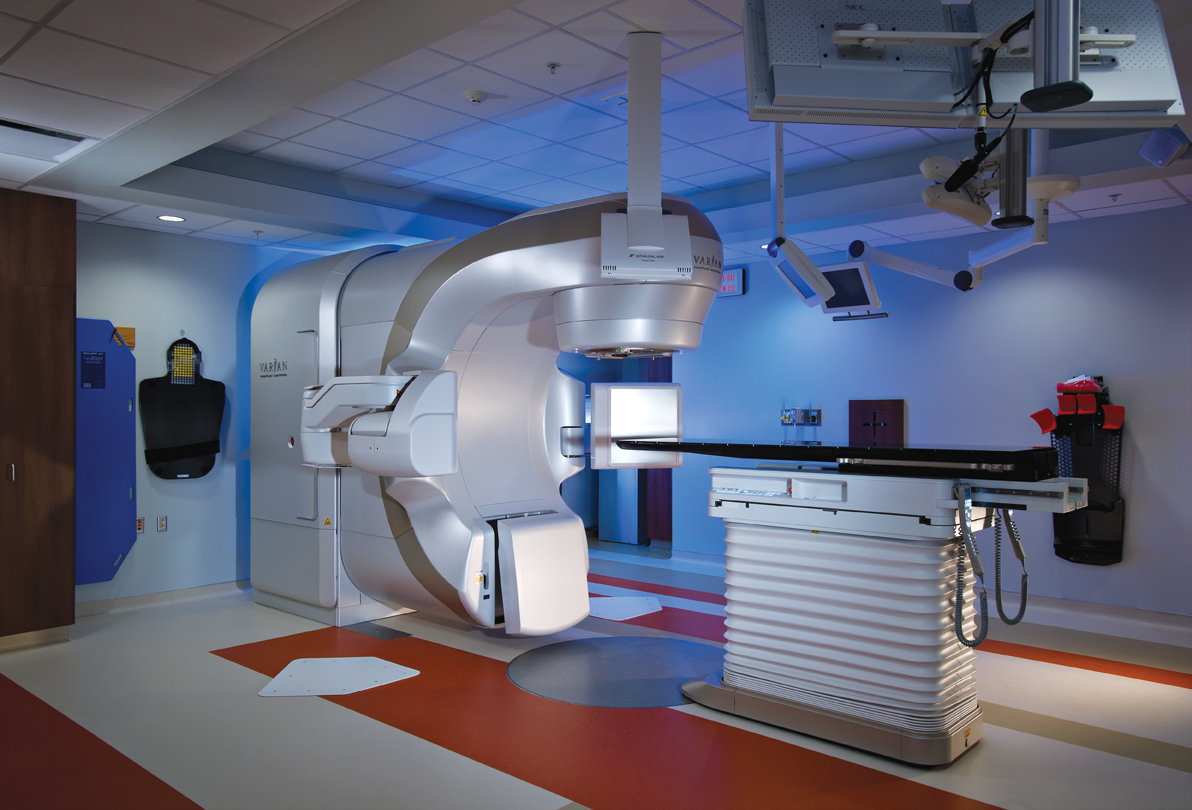
There are currently three linear accelerators in operation at Banner MD Anderson Cancer Center, all of which are Varian TrueBeam models.
Since opening in September 2011, the Banner MD Anderson Cancer Center has become a premier regional center for cancer patients in the greater Phoenix area. With some of the latest state-of-the-art technology in place, the Gilbert, Ariz., facility prides itself on offering patients the same level of care that they would receive at the University of Texas MD Anderson Cancer Center. “The philosophy is to treat patients with the same protocols and philosophy that they would get as if they went to Houston,” said Stephen Sapareto, Ph.D., DABR, director of medical physics, division of radiation oncology, Banner MD Anderson Cancer Center.
A Partnership Emerges
While MD Anderson has a number of affiliates around the United States — as well as one in Istanbul, Turkey, and Madrid, Spain — this particular center in Arizona was the first to arise from a unique partnership between MD Anderson and the nonprofit health system Banner Health. Based in Phoenix, Banner Health had been exploring the idea of developing a cancer center partnership for years, said Sapareto. Eventually Banner Health and MD Anderson came together and negotiated the establishment of the Banner MD Anderson Cancer Center. The center currently has a full staff of physicists, therapists, nurses, administrators and more.
“All our clinical care is overseen by MD Anderson Houston,” stated Matthew Callister, M.D., division chief of radiation oncology, Banner MD Anderson Cancer Center. “We have a very strong clinical relationship with them, where they have set guidelines and we’re contributing to those guidelines.” Callister added that the center strives to maintain conformity of care, ensuring that patients treated in Gilbert receive the similar quality of care as they would have received in Houston.
The relationship between Banner MD Anderson and the main campus in Houston is a close one, added Donald Schomer, M.D., chief of diagnostic imaging, Banner MD Anderson Cancer Center. “We are an adjunct to MD Anderson Houston. Many of the faculty here, and most of the leadership, are from MD Anderson,” explained Schomer, who himself was previously a tenured associate professor at MD Anderson, and had moved to Colorado before being recruited back to MD Anderson and landing at the new cancer center in 2011. “Our goal is to really try and bring the culture of MD Anderson Houston to the desert.”
State-of-the-Art Technologies
The range of therapies available at Banner MD Anderson features many of the latest technological advances in cancer treatment. Some options include external beam radiation therapy (EBRT) and intensity-modulated radiation therapy (IMRT). The center also offers image-guided radiation therapy (IGRT) performed with the volumetric modulated arc therapy (VMAT) technique, in which radiation beams sweep in uninterrupted arcs around the patient.
Currently there are three linear accelerators (linacs) in operation at Banner MD Anderson, all of which are Varian TrueBeam models. One of the systems is a TrueBeamSTx, which is specialized for both radiosurgery and stereotactic body radiation therapy (SBRT) applications, according to Sapareto.
In addition the facility features a Nucletron remote afterloader unit for internal high-dose rate (HDR) brachytherapy, which at Banner MD Anderson is primarily used for partial breast irradiation (PBI) and gynecological treatment. The HDR suite also serves as a procedure room for the placement of fiducial markers when they are needed in treatments where sharp precision is required, said Sapareto.
Also found in the Nucletron vault is a computed tomography (CT) scanner, making Banner MD Anderson the only center in the state of Arizona to have a CT system in the same vault as the HDR unit, according to Sapareto. “It is extremely convenient, because that means once applicators are in patients for this remote afterloader procedure, they don’t have to be moved to be treated,” he said. While other facilities have to transport patients undergoing HDR brachytherapy from the imaging suite to the treatment room, doctors at Banner MD Anderson don’t have that problem. This minimizes the risk of applicators shifting during transition from planning to treatment.
Elsewhere in the facility, imaging systems include a positron emission tomography/CT (PET/CT), single-photon emission computed tomography/CT (SPECT/CT), regular CT and a 3.0T magnetic resonance imaging (MRI) scanner. In addition Banner MD Anderson uses the Pinnacle3 treatment planning system for all courses of radiation therapy, from the very conventional to the more “advanced SBRT-type treatments and the VMAT,” said Sapareto. It also uses the Mosaiq oncology information system (OIS) from Elekta for recording and storing patient information.
Looking Ahead
Having only been open a couple of years, the technology at Banner MD Anderson has the advantage of still being very much state-of-the-art, stated Sapareto, adding that “nothing’s older than two years here.” The center is due to receive even more new imaging and treatment systems, as construction continues on a Phase II expansion that will double the space of the current facility.
“All of the departments will essentially be doubling their space,” explained Sapareto. Three more vaults will be added, two of which will be filled with Elekta Versa HD linacs, bringing the center’s number of linacs up to five. The center is also adding a large bore CT scanner from Philips and a second PET/CT system. Phase II is scheduled for completion in April 2014, and will feature implementation of new technologies such as radio frequency (RF) patient monitoring, and ultrasound and laser positioning guidance.
Banner MD Anderson also plans on developing more as a research organization in addition to a clinical one focused on excellent patient care, according to Schomer. One such program in development that ties both the core ideas of research and care together is the notion of express diagnostics, which focuses on “moving image-based procedures closer to the point of service,” he said. In conjunction with the pathology department, the imaging department at Banner MD Anderson aims to cut down on the time between when patients come into the clinic for a scan and when results are delivered and a diagnosis is given. For example, a woman coming in for a mammogram may soon be able to receive a diagnosis within a single day or visit, rather than having to wait three weeks from the time she comes in for the original scan to when a biopsy is performed and her team of doctors can deliver the correct diagnosis. The idea, according to Schomer, is to reduce costs not only for the healthcare provider but also for the patient, who may have to arrange for childcare or time off work in the interim.
With such plans in place, carrying the same esprit de corps, as Schomer puts it, as the main comprehensive cancer center in Houston should be a natural task for the Banner MD Anderson Cancer Center, and it is poised to continue moving forward as a fast-growing center of excellence and care for patients in Arizona and beyond. Concluded Sapareto: “Our philosophy is to prepare for the future of healthcare.”
Editor’s note: Imaging Technology News (ITN) sought reader nominations for the top cancer centers to watch in 2013, based on use of technology in radiation oncology. Key factors considered included how new technologies are being used to help improve patient outcomes, increase efficiency, reduce costs, increase patient volume or increase reimbursements/revenues.
ITN received a record number of entries, and from these, narrowed them to seven top centers that are striving to make a difference in patients’ lives. ITN congratulates these facilities for their achievements, and will feature a new center in each issue in the months ahead. Thank you to everyone who shared their stories of success with us.



 April 18, 2024
April 18, 2024