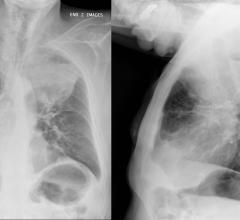
Tablet computers are ideal for reviewing clinical images during rounds, but only for images upon which primary diagnosis has already been performed.
Mobile devices have become a part of everyday life. The cell phone has become as important as your wallet to take with you wherever you go. Some would argue that it’s even more essential now that handheld computers have morphed into a ubiquitous Internet access device for most physicians.
As screen quality on these devices has improved and tablet computers have rapidly proliferated, their viability for use in medical imaging has become a common expectation among physicians. In fact, nearly 80 percent of physicians are using smart phones and mobile devices in their medical practice, with interest in mobile viewing of patient images increasing daily.
The pixels on today’s cell phones and mobile tablets are numerous and small enough to feed your eyes as much as they can see, and are sufficiently bright to be seen in most lighting conditions. So, why not rely on them as a convenient, portable diagnostic imaging tool around the hospital?
DICOM Matters
For one, today’s mobile devices are not specifically designed for diagnostic imaging applications, mostly because they are unable to maintain continuous, accurate digital imaging and communications in medicine (DICOM) calibration due to a lack of internal or external sensors necessary to achieve it. Secondly, in order to utilize a mobile device for diagnostic image review, it must be DICOM-compliant, i.e., maintain image quality similar to a high-resolution radiology display.
A DICOM-calibrated image provides accurate image representation and confidence for the medical professional. Once a screen is calibrated properly, radiologists can diagnose images from most modalities, like computed tomography (CT), magnetic resonance (MR), ultrasound, computed radiography (CR) and digital radiography (DR), which have been cleared by the U.S. Food and
Drug Administration (FDA) for diagnostic reading
on a mobile tablet when proper quality measures are in place.
The Mobile Imaging Calibration Challenge
Several options exist for calibrating mobile tablets based on the use of a “tap test.” A visual calibration process provides DICOM performance based on a user’s eyesight level and dynamic contrast available in the given ambient light conditions to make proper diagnosis. The calibration is conducted using a third-party software tool integrated into any authorized mobile viewer application that has obtained all required registrations and certifications as specified by the FDA.
Once properly calibrated, the mobile tablet can display images with excellent clarity and precision for modalities currently deemed acceptable by the FDA. A DICOM-calibrated tablet can be a convenient alternative in case of emergency situations when a diagnostic display isn’t available, when a primary diagnosis has already been made using a full-size display, for consulting with other clinicians and in patient consultations.
Form Follows Function
Imagine trying to navigate a path across the United States on a screen the size of your wristwatch. Regardless of how many pixels are crammed onto the display, and no matter how much zooming and panning you do, it’s nearly impossible to get a good feel for the path with such a limited viewport. The same applies in viewing medical imaging studies: Overall size of the device is an important factor with respect to the image area.
For example, it’s difficult to properly evaluate an entire radiograph of the chest on a three- to four-inch diagonal smart phone screen. While it may be possible to accurately read a large-matrix image like this on a tablet computer, no radiologist would desire to read 100 chest X-rays on such a small device. It’s just too cumbersome to do on more than an occasional basis; it’s time-consuming and just plain ill-advised. Furthermore, radiography has larger demands when it comes to luminance. For primary diagnosis, no less than 350 cd/m2 should be used and ideally 400 cd/m2. But, that’s only if primary diagnosis is required.
By the same token, the luminance of most smart phones and tablets is perfectly acceptable in cases where a primary care doctor is reviewing findings made by a radiologist using a full-size display. For smaller size modalities like CT and MRI, most smart phone screens are typically up to the task, as long as luminance is around 200 cd/m2. Naturally, the larger 9-inch tablet screens are even better suited for viewing these images. The FDA has cleared the use of some mobile device software for small matrix images (non-radiography) only when there is no access to a full workstation. Their evaluation of these software programs continues to evolve.
The Pixel/Image Quality Paradigm
As the new American College of Radiology (ACR) guidelines point out, the number of pixels is a handy way to describe a display, but it’s not really important when it comes to medical imaging. What matters most is the size of those pixels relative to the distance you hold the device away from your eyes. The closer you hold it, the smaller the pixels should be to maximize what you can see.
In the Apple “retinal” display, the pixels are just below the threshold of what your eye can discriminate (so, theoretically, there’s no point in making them any smaller). The larger the screen, the further away one tends to hold it and, therefore, the larger the pixels can be. So, while every display has a number of pixels you can count, that number alone is insufficient to describe the resolution characteristics of a display.
Convenience in the Clinical Setting
Tablet computers are ideal for reviewing clinical images during rounds, and by residents and attendings as a portable viewer — but only for images upon which primary diagnosis has already been performed. They can and should replace the clipboard, we believe. We also would argue that a radiologist can perform primary diagnosis on one if it is properly calibrated, and only if sufficient time is spent thoroughly examining the image with optimal zooming and panning to view enough of the original pixels. We urge caution in cases where residents are inclined to make primary diagnoses themselves — such as in intensive care units (ICUs) and other tertiary care settings. Extreme care should be exercised to use proper displays for those purposes, lest they improperly treat a patient due to use of a substandard or uncalibrated display.
On the Horizon
The usability of mobile devices in diagnostic imaging will be enhanced by increased speed and coverage of wireless networks and faster processors with lower power requirements, resulting in longer battery life. Further improvements are necessary to guarantee an effective method of ensuring image quality — including DICOM compliance — as well as tracking and documenting that information. The user-interfaces of these devices will continue to improve, making these tools even more useful and intuitive in the future. itn
David Hirschorn, M.D., is director of radiology informatics, Staten Island University Hospital, and researcher in radiology informatics, Massachusetts General Hospital. Ketan Thanki is market development manager, healthcare for Barco.


 April 22, 2024
April 22, 2024